Session Information
Date: Monday, October 22, 2018
Title: Metabolic and Crystal Arthropathies – Basic and Clinical Science Poster I
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Evidence is conflicting concerning dementia risk in gout patients, with hyperuricaemia proposed to exert a neuroprotective effect. Serum urate (sUA) targets guiding urate-lowering therapies (ULT) are poorly evidenced-based and there is a shifting consensus towards a more lenient target to attempt to balance the theoretical harmful effects of hypouricaemia. The aim of this study was two-fold; first, to estimate the risk of dementia among patients with gout, second, to assess the potential impact of ULT.
Methods: Retrospective population-based matched cohort study conducted using the Clinical Practice Research Datalink (CPRD), a large anonymized primary care database. Gout exposure was defined as a first entry of a medical code for gout (previously validated in CPRD with high accuracy (>90%))1 between April 1998-February 2016. Each gout exposed patient was matched to 4 unexposed controls on age (±5 years), gender, general practice and follow-up in CPRD (±3 years). The absolute rate of dementia onset was calculated for gout exposed and unexposed and hazard ratios (HR) were modelled using Cox Proportional Hazards Regression. The analysis was stratified by dementia type (Alzheimers disease (AD), vascular dementia, other dementia types). Finally, among gout cases we assessed the impact of ULT on dementia onset. ULT exposure, defined as at least 6 month prescription, was assessed within 1 and 3 year exposure windows after gout diagnosis.
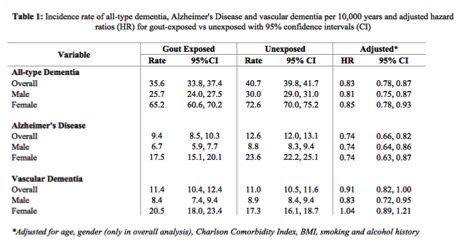
Results: Our cohort of 79,097 gout exposed and 276,808 unexposed had a median follow-up time of 5 years (interquartile range=6.2), mean age of 62 years (standard deviation=15.2) and 73% male. The absolute incidence rate of all-type dementia per 10,000 years was lower in the gout exposed cohort than the unexposed (35.6 (95% Confidence Interval (CI) 33.8 – 37.4) vs 40.7 (95% CI 39.8 – 41.7)) corresponding to a 17% lower risk (HR=0.83 95% CI 0.78 – 0.87) (Table 1). The incidence of AD and other dementia types was lower in the gout cohort, but not vascular dementia (Table 1). Within gout cases, ULT exposure within 1 and 3 years after gout diagnosis did not significantly affect dementia risk after adjustment for potential confounders.
Conclusion: This provides observational evidence supporting the hypothesis that hyperuricaemia has a neuroprotective role, with gout patients having lower dementia risk. This risk was unaffected by ULT, but further studies are required to determine if this differs with longstanding ULT use, dose or magnitude of urate-lowering. This would help devise a more evidence-based sUA target for guiding gout management, which optimally balances a therapeutic target against the possible harmful effect of hypouricaemia.
References: 1. Meier, C. R. & Jick, H. Omeprazole, other antiulcer drugs and newly diagnosed gout. Br. J. Clin. Pharmacol. 44, 175–8 (1997).
To cite this abstract in AMA style:
Crowley L, Abdul Sultan A, Roddy E, Mallen C, Protheroe J, Clarson L. Risk of Dementia in Patients with Gout and the Impact of Urate-Lowering Therapies: A Large Population-Based Cohort Study [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/risk-of-dementia-in-patients-with-gout-and-the-impact-of-urate-lowering-therapies-a-large-population-based-cohort-study/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/risk-of-dementia-in-patients-with-gout-and-the-impact-of-urate-lowering-therapies-a-large-population-based-cohort-study/