Session Information
Date: Sunday, November 7, 2021
Title: Systemic Sclerosis & Related Disorders – Basic Science Poster (0541–0559)
Session Type: Poster Session B
Session Time: 8:30AM-10:30AM
Background/Purpose: The PD-1/PD-L1 pathway has been implicated in Systemic Sclerosis (dSSc). This disease is dominated by increased extracellular matrix deposition initiated by myofibroblasts. We therefore examined the PD-1/PD-L1 pathway in dSSc myofibroblasts and its influence on fibrosis.
Methods: Dermal fibroblasts were isolated from the skin from patients with dSSc (n=9) and compared with dermal fibroblasts from healthy controls (HC)(n=4). Cells were stimulated with TGF β for 48 hours and analyzed by flow cytometry for expression of the surface proteins CD45, Thymocyte differentiation antigen-1 /(CD90 Thy-1), podoplanin (PDPN), Programmed Death Protein Ligand-1(PD-L1), Fibroblast activation Protein (FAP),and Intercellular adhesion molecule-1 (ICAM-1) and alpha smooth muscle actin (α- SMA). Supernatants were analyzed for the production of Type 1 Procollagen and IL-6. Parallel to this, dcSSc fibroblasts, were stimulated with IFNγ (10ng/ml) for 48 hours followed by addition of anti-PD-L1 antibody (atrezolizumab, 5ug/ml) and soluble, recombinant PD-1 (RPD-1;1ug/ml). Supernatants were harvested after 48 hours and analyzed for production of Type 1 Procollagen and Fibronectin.
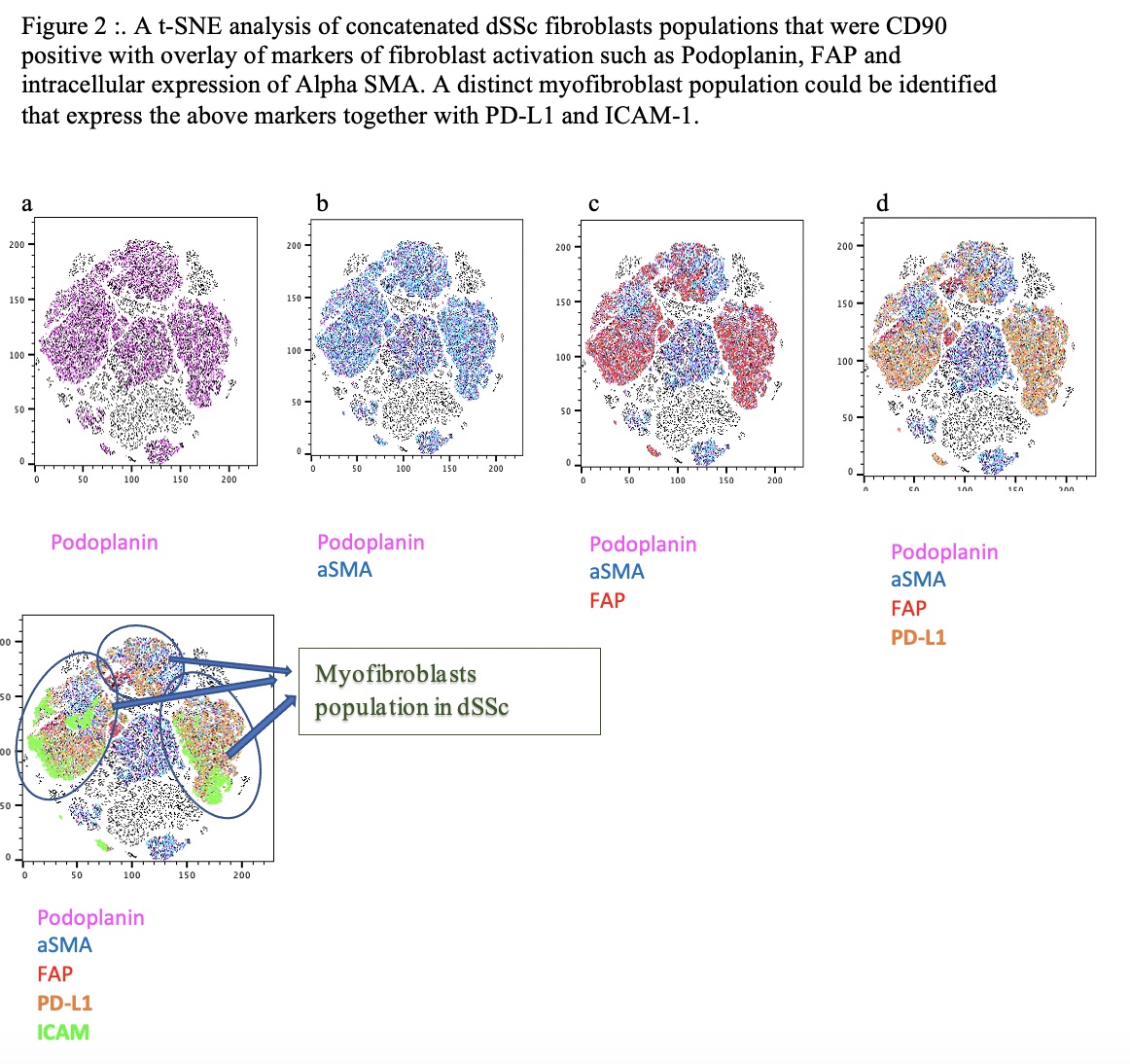
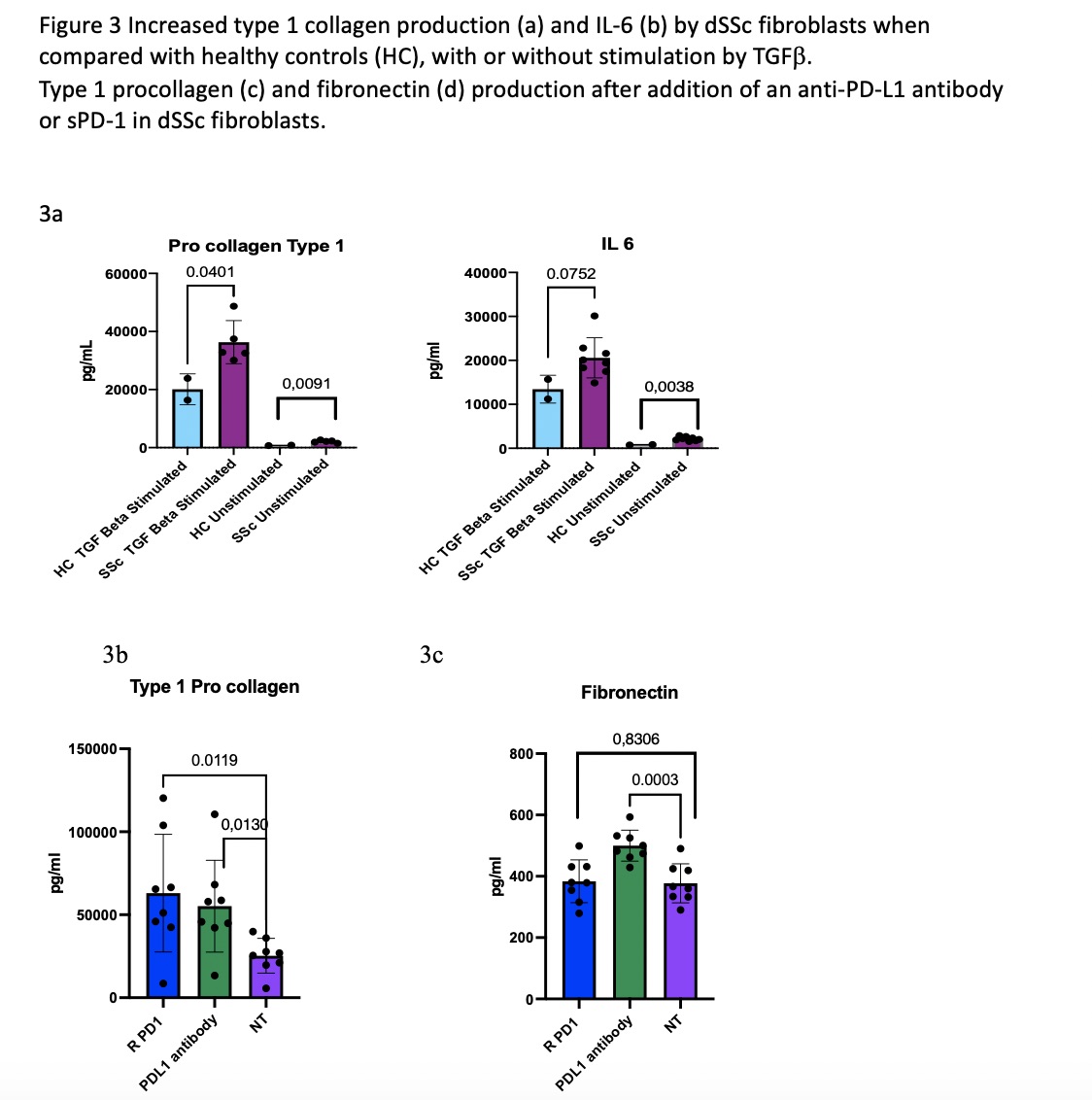
Results: CD45neg fibroblasts, from both dSSc as well as HC could be identified by their expression of Thy-1 and Podoplanin. Upon stimulation with TGFβ, fibroblasts from dSSc patients increased the percentages of myofibroblasts expressing PD-L1, α- SMA, ICAM-1, FAP and Podoplanin when compared to HC fibroblasts.(Figure 1) All p < 0.05, Figure 1. Upon concatenating and analyzing this data by tSNE, we could demarcate a distinct populations of the myofibroblasts that had a high expression of PD-L1 together with ICAM-1 (Figure 2). Compared with HC, dcSSc fibroblasts were characterized by an increased production of Type 1 Procollagen and IL -6, this was highly increased by stimulation with TGFβ, still most pronounced in dSSc (Figure 3a). To explore the role of PD-L1 in fibrosis, we added an anti-PD-L1 monoclonal antibody, or rPD-1 to fibroblasts. Both increased the production of Type 1 Pro-collagen, whereas fibronectin was only increased by adding the anti-PD-L1 antibody(Figure 3b).
Conclusion: dSSc fibroblasts are distinct from dermal fibroblasts from HC, both in their phenotype and functionality. The myofibroblast population can thus be defined as a subset within the dSSc fibroblasts with high and co-expression of PD-L1, FAP, Podoplanin, and ICAM. PD-L1 plays an important role in regulating fibrosis, and inflammation in dSSc and our results supports the notion that PD-L1 does this through reverse signaling.
Type 1 procollagen (c) and fibronectin (d) production after addition of an anti-PD-L1 antibody or sPD_1 in dSSc fibroblasts.
To cite this abstract in AMA style:
Aspari M, Greisen S, Hvid M, Sondergaard K, Ong V, Denton C, Abraham D, Deleuran B. Reverse Signaling Through PD-L1 Plays a Central Role in Extracellular Matrix Protein Secretion from Cutaneous Myofibroblasts in Systemic Sclerosis [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/reverse-signaling-through-pd-l1-plays-a-central-role-in-extracellular-matrix-protein-secretion-from-cutaneous-myofibroblasts-in-systemic-sclerosis/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/reverse-signaling-through-pd-l1-plays-a-central-role-in-extracellular-matrix-protein-secretion-from-cutaneous-myofibroblasts-in-systemic-sclerosis/