Session Information
Session Type: Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Disparities in health care utilization based on sex, race, education, or income affect outcomes in rheumatologic care. We have used ocular inflammatory and infectious disease, which complicates many rheumatic diseases, to study some of these disparities. These eye conditions, significantly increase disease burden, especially in people greater than 65 years of age and disproportionately affect females and racial minorities. However, there is lack of national level data in the US regarding influence of age, sex and race on utilization of medical care for inflammatory and infectious eye disease in people > 65 years. We have conducted an epidemiologic study using the Medicare database to analyze these trends and the influence of age, sex and race.
Methods: We have used Medicare data available through National Vision and Eye Health Surveillance System (VEHSS). Medicare data are collected from research identifiable files obtained through the Center for Medicare and Medicaid Services (CMS) and include all fee for service beneficiaries.
VEHSS uses ICD-10 codes to identify ocular disorders and organizes them into two level categorization, which are category and subgroup. Each code is categorized in one subgroup and multiple subgroups are combined to form a category. Inflammatory and infectious eye disease category includes subgroups of ocular inflammatory conditions, lacrimal system and orbital inflammation, keratitis, conjunctivitis, eyelid inflammation and infection and endophthalmitis.
Utilization for the inflammatory and infectious eye disease caterogory, is stratified by age, sex and race. We have measured trends of utilization for the category and for the individual subgroups for the years 2014-2017. We have identified the effect of stratification on utilization; by race, sex, age alone; combining race and sex; age and sex; and the combination of race, sex and age.
Results: There were 29,971,000, 30,027,208, 30,423,400 and 30,238,300 million Medicare beneficiaries enrolled for the years 2014 to 2017 respectively. There was a decrease in utilization for inflammatory and infectious eye diseases category and subgroups from the year, 2014 to 2015 followed by a steady increase from 2015-2017 (Figure 1). This trend remains, when utilization is stratified by sex, race and age.
Asians and Hispanics have higher utilization for the inflammatory and infectious eye diseases category, and for the individual subgroups, for both males and females (Figure 2). This higher utilization remains, when further stratified by age.
Females have higher utilization across all races. This holds true when utilization is stratified by race; an Asian female has higher utilization than an Asian male (Figure 3). And remains steady when we further stratify by age groups. An Asian female of age group: 65-84 has higher utilization than an Asian male of the same age group; for all the years of the study 2014 to 2017.
Conclusion: Females, Asians and Hispanics have higher Medicare utilization for inflammatory and infectious eye diseases. These results may be due to higher disease prevalence or service utilization in these subgropus. Racial and sex-based disparitiies should be considered when making health care policy decisions
 Figure 1: Trend for Medicare Utilizaiton of Inflammatory and Infectious eye disease category and subgroups: 2014-2017.
Figure 1: Trend for Medicare Utilizaiton of Inflammatory and Infectious eye disease category and subgroups: 2014-2017.
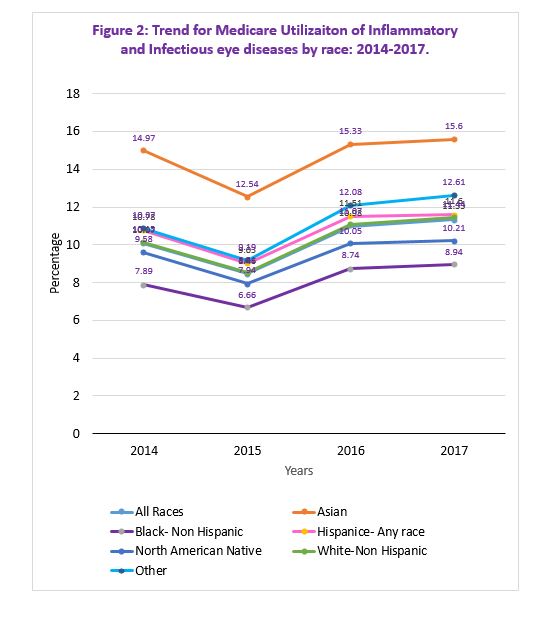 Figure 2: Trend for Medicare Utilizaiton of Inflammatory and Infectious eye diseases by race: 2014-2017.
Figure 2: Trend for Medicare Utilizaiton of Inflammatory and Infectious eye diseases by race: 2014-2017.
 Figure 3: Medicare Utilization of Inflammatory and Infectious eye diseases by sex and race: 2014-2017
Figure 3: Medicare Utilization of Inflammatory and Infectious eye diseases by sex and race: 2014-2017
To cite this abstract in AMA style:
Chauhan K, Rosenbaum J. Racial and Sex-based Disparities in Health Care Utilization: Eye Inflammation as a Paradigm [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/racial-and-sex-based-disparities-in-health-care-utilization-eye-inflammation-as-a-paradigm/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/racial-and-sex-based-disparities-in-health-care-utilization-eye-inflammation-as-a-paradigm/
