Session Information
Title: Rheumatoid Arthritis - Clinical Aspects (ACR): Comorbidities, Treatment Outcomes and Mortality
Session Type: Abstract Submissions (ACR)
Background/Purpose: Rheumatoid arthritis (RA) is associated with higher rates of cardiovascular disease (CVD) and subclinical atherosclerosis as well as psychosocial comorbidities, which themselves are associated with CVD. We explored if psychosocial comorbidities differentially contribute to CVD risk in individuals with RA compared with non-RA controls.
Methods: Data were derived from a longitudinal cohort study of subclinical cardiovascular disease in RA and non-RA controls. Using validated scales, psychosocial comorbidities (depression, chronic life stressors, anxiety/anger, social support, discrimination/hassles) were assessed. Differences in the associations of psychosocial measures with measures of subclinical atherosclerosis [coronary artery calcium (CAC) assessed using computed tomography and carotid intimal-media thickness (IMT)/plaque assessed using ultrasound] were explored using multivariable regression models incorporating RA x psychosocial variable interaction terms. Models were adjusted for relevant unbalanced demographic variables, CVD risk factors, and markers of RA activity/inflammation.
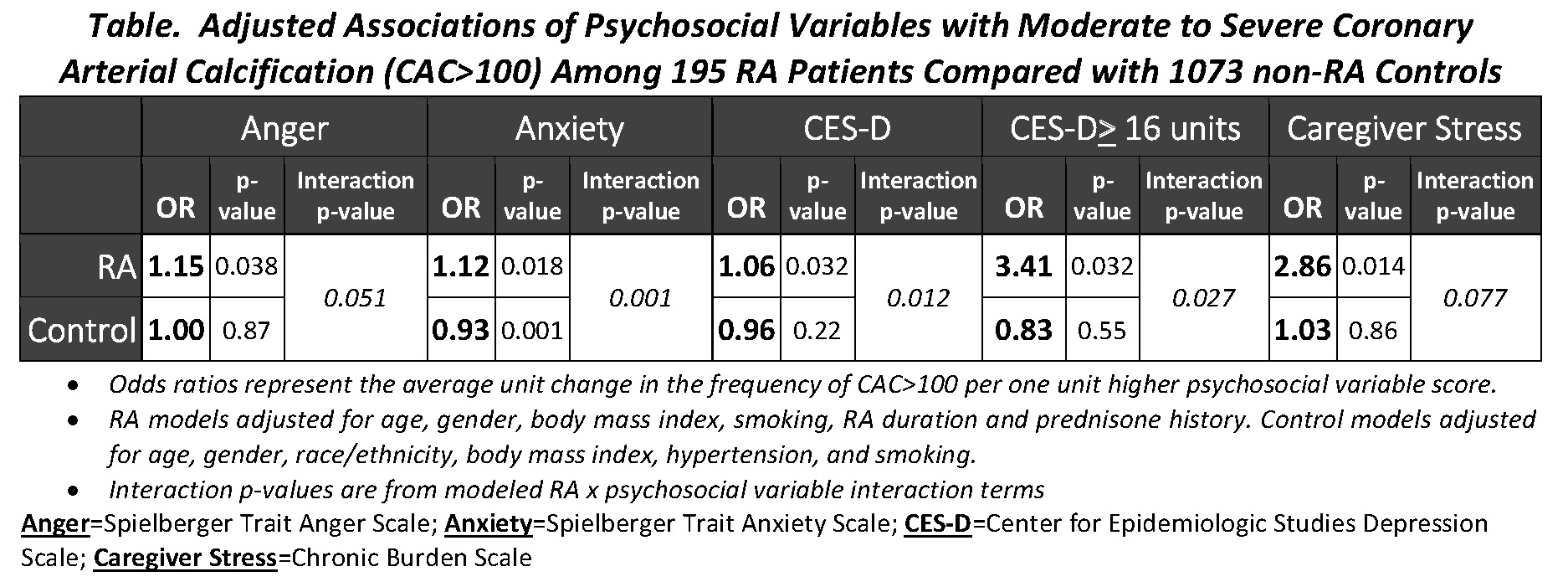
Results: 195 RA patients [mean age=59 ± 9 years, 61% female; 87% Caucasian; median RA=9 years; mean DAS28=3.65 ± 1.1] were compared with 1073 controls. RA participants had a higher prevalence of psychosocial comorbidities (depression and personal health, job, and total stress) compared with controls. In RA, per-unit higher Spielberger trait anxiety scores and the presence of caregiver stress were associated with an increased adjusted odds of CAC>100 units (Table). Per-unit higher Spielberger trait anger scores and Center for Epidemiologic Studies Depression scores were also associated with an increased odds of CAC>100 after adjustment (Table), although these effects were diminished with adjustment for anxiety. All associations were preserved after adjusting for markers of inflammation (IL-6 and CRP) and were only observed in RA patients, but not controls (adjusted interaction term p-values 0.001-0.077). Having job stress was associated with an increased frequency of carotid plaque [adjusted OR=3.21 (p=0.019)], and increasing social support was associated with lower internal carotid IMT (adjusted p=0.024) in RA participants, but not in controls.
Conclusion: Depression, stress, anger/anxiety and social support may affect CVD risk, specifically in RA patients, by promoting atherosclerosis. Because the impact of these factors on atherogenesis may be accentuated in RA compared with the non-RA population, screening and treatment of psychosocial comorbidities may help reduce the known increased burden of CVD in RA.
Disclosure:
Y. Liu,
None;
M. Szklo,
None;
K. Davidson,
None;
J. Bathon,
None;
J. Giles,
None.
« Back to 2014 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/psychosocial-comorbidities-are-independently-associated-with-subclinical-atherosclerosis-in-rheumatoid-arthritis/