Session Information
Date: Tuesday, November 12, 2019
Title: Orthopedics, Low Back Pain, & Rehabilitation Poster – ACR/ARP
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Total knee arthroplasty (TKA) is a valuable option for improving function and pain control in patients with end-stage arthritis, especially those with inflammatory arthritis like Rheumatoid arthritis (RA) or Psoriatic arthritis (PsA). RA and PsA have been associated with an overall increased risk of peri-operative complications, including infections and cardiovascular mortality. There is limited information comparing short-term inpatient complications like post-operative anemia and wound dehiscence in patients with RA or PsA. Anemia has been associated with delayed functional recovery for patients undergoing arthroplasty as well as higher postoperative morbidity and mortality. We aim to assess the prevalence of short term inpatient complications like post-operative anemia and wound dehiscence in patients undergoing TKA with RA and PsA
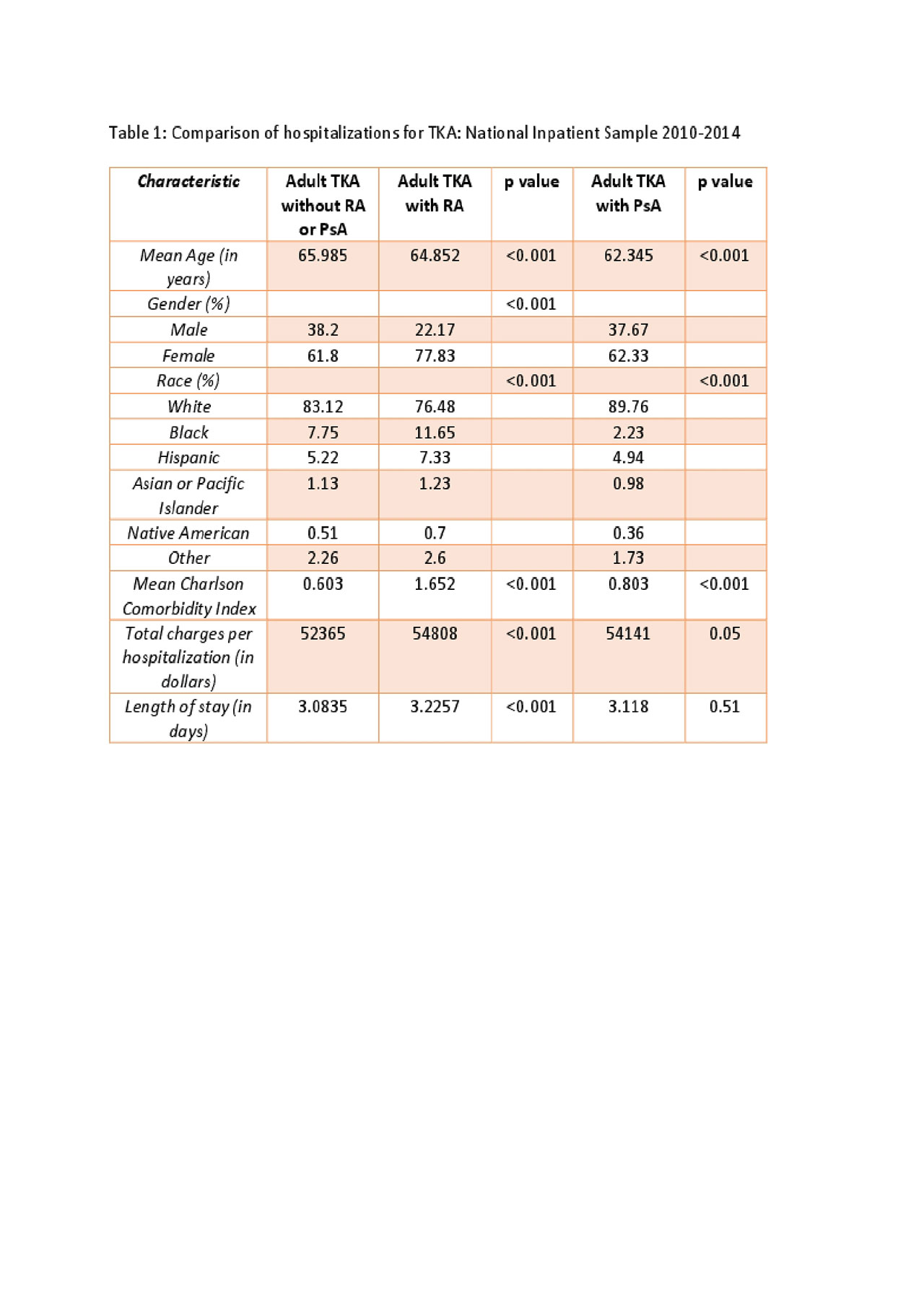
Methods: National Inpatient Sample (NIS)is the largest all-payer inpatient care database in the United States, with approximately 8 million hospitalizations each year. We extracted data for all the adult admissions for TKA from NIS database from 2010-2014 and stratified it into groups based on the status of RA and PsA; using ICD-9 CM diagnostic codes. The baseline characteristics, mortality, the prevalence of post-operative infections, wound dehiscence, and postoperative acute hemorrhagic anemia were compared, using appropriate statistical tools. Stata version 15 (College Station, TX) was used to perform the statistical analysis.
Results: An estimated total of 3172824 hospitalizations for TKA were identified, with around 3157706 TKA and 15117 revision TKA. Amongst these hospitalizations 108101 had an underlying diagnosis of RA and 7421 had an underlying diagnosis of PsA. No difference in postoperative mortality, postoperative infections, or risk of wound dehiscence was noted in these subgroups. But these subgroups were found to have significantly higher rates (p< 0.05)of postoperative acute hemorrhagic anemia. The Odds Ratio for patients admitted for TKA with an underlying diagnosis of RA was estimated as 1.295(95% confidence interval=1.249-1.342). 27.92% hospitalizations for TKA with underlying RA were found to have post-operative anemia (p-value < 0.001). The admissions for TKA with psoriatic arthritis also had significantly higher odds of post-operative acute hemorrhagic anemia (Odds Ratio 1.13, 95% confidence interval 1.012-1.282).
Conclusion: The study estimates that admissions for TKA with underlying RA or PsA have significantly higher rates of postoperative anemia. It may represent pre-existing anemia worsening with surgery, as RA and PsA are associated with anemia of chronic disease. Another explanation can be concomitant use of medications like NSAIDs, DMARDs, or steroids for treatment of RA and PsA. We suggest that besides pre-operative cardiovascular and infection risk assessment, patients with RA and PsA should also be screened for anemia, to avoid postoperative morbidity and mortality.
To cite this abstract in AMA style:
Jatwani K, Chugh K, Bindra B, Jatwani S. Prevalence of Postoperative Anemia in Patients with Rheumatoid Arthritis and Psoriatic Arthritis Undergoing Total Knee Arthroplasty: A Study of National Inpatient Sample 2010-2014 [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/prevalence-of-postoperative-anemia-in-patients-with-rheumatoid-arthritis-and-psoriatic-arthritis-undergoing-total-knee-arthroplasty-a-study-of-national-inpatient-sample-2010-2014/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/prevalence-of-postoperative-anemia-in-patients-with-rheumatoid-arthritis-and-psoriatic-arthritis-undergoing-total-knee-arthroplasty-a-study-of-national-inpatient-sample-2010-2014/