Session Information
Session Type: Poster Session (Monday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Peripheral neuropathy (PN), one of the neuropsychiatric syndromes of SLE, occurs in 2% to 36% of patients. It has been associated with high disease activity indices and poor quality of life scores. The aim of this study was to determine the prevalence of peripheral neuropathy using clinical evaluation and Nerve Conduction Studies (NCS), to describe its electrophysiological types using NCS; and to correlate quality of life with presence of peripheral neuropathy among SLE patients
Methods: This was a crossectional study of SLE patients attending Rheumatology outpatient clinic. Fourty eight patients with a diagnosis of SLE as per the 2012 Systemic Lupus International Collaborating Clinics (SLICC) criteria who were 18 years and above were consecutively selected for the study. Patients were excluded if they were Amputees, had history of traumatic involvement affecting the nerves, had foot ulcerations, those with other known causes of peripheral neuropathy such as mixed connective tissues disease, diabetes mellitus, and history of heavy alcohol consumption, chronic renal failure and pernicious anemia. Socio-demographic data and clinical information were obtained from the patient’s medical records. Structured history and clinical examination was performed on all patients. All patients had NCS carried out and at least 5 nerves were tested: the median, the ulnar, the peroneal, the sural and the Tibial. Lupus quality of life questionnaire was administered to all patients.
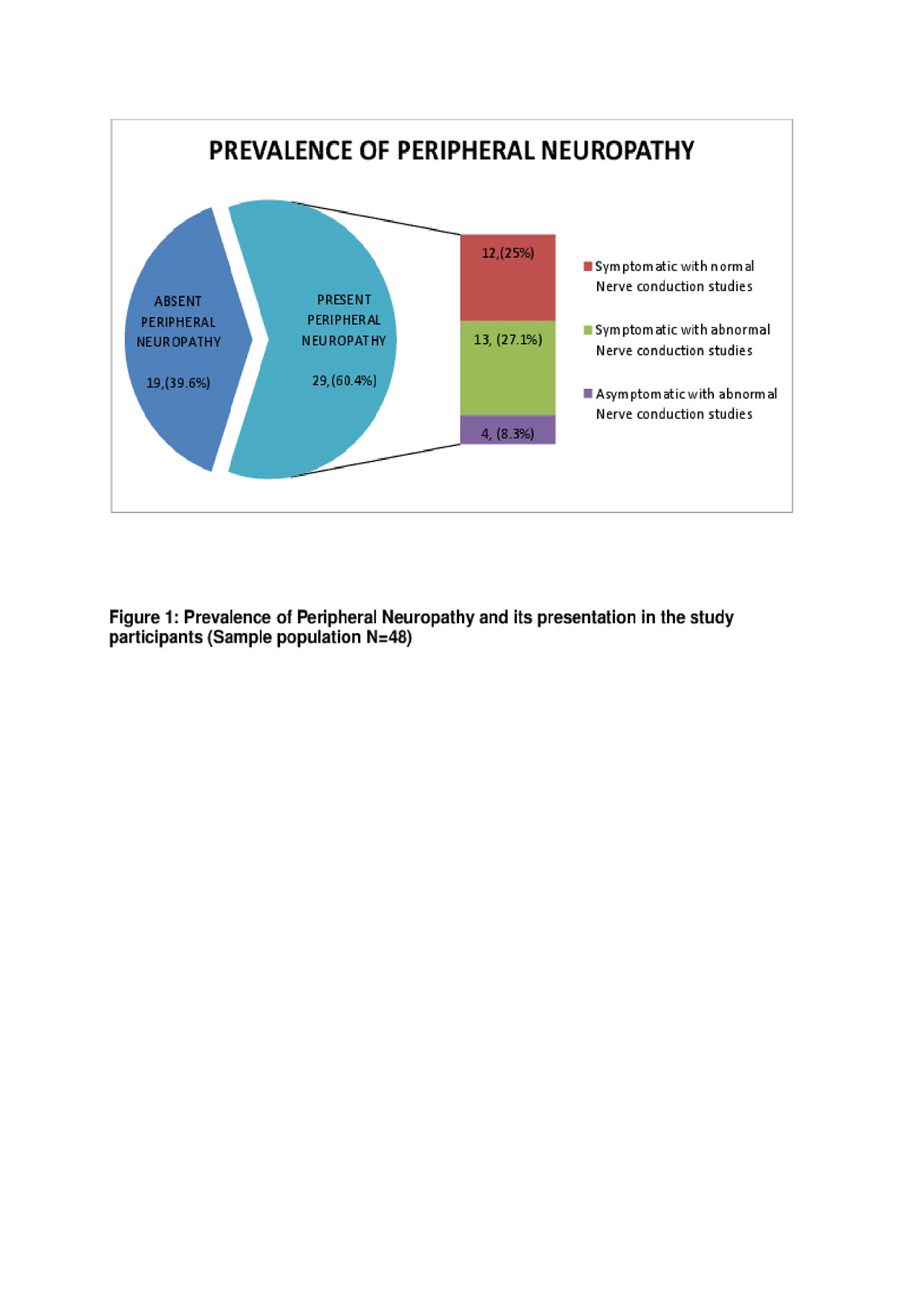
Results: Prevalence of PN was suggestive in 29 out of 48 patients (60.4%). Of these 27.1% were symptomatic for peripheral neuropathy and had abnormal nerve conduction studies while 25 % were symptomatic for peripheral neuropathy and had normal nerve conduction studies. The other 8.3 % had abnormal nerve conduction studies despite being asymptomatic (figure 1). Numbness was the most common symptom complaint in 41.7% of patients. The most common nerve conduction abnormality was demyelination 9(52.94%). However excluding 5 patients found to have carpal tunnel syndrome, then demyelination was 4(23.52%), While axonopathy was found in 5(29.41%) of the patients. Motor neuropathy was the most prevalent nerve conduction syndromes in 9(52.94%) patients. There was a significant correlation between the presence of peripheral neuropathy with lower quality of life scores involving the domains of physical health (p=< 0.001), pain (p=0.012), planning (p=0.003), and fatigue (p=0.005).
Conclusion: There is a high prevalence of peripheral neuropathy among SLE patients, with variable clinical and electrophysiologic presentation. Quality of life is scores are lower in affected patients
To cite this abstract in AMA style:
Wendo C, Oyoo G, Otieno Kwasa T, Maritim M, Nakitare S, Kwasa J. Prevalence of Peripheral Neuropathy and Its Electrophysiological Types in Patients with Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/prevalence-of-peripheral-neuropathy-and-its-electrophysiological-types-in-patients-with-systemic-lupus-erythematosus/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/prevalence-of-peripheral-neuropathy-and-its-electrophysiological-types-in-patients-with-systemic-lupus-erythematosus/