Session Information
Date: Sunday, November 8, 2020
Title: SLE – Diagnosis, Manifestations, & Outcomes Poster II: Comorbidities
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Frailty, defined as a generalized vulnerability to stressors, has emerged as a relevant concept in SLE1, although its origins are in geriatrics. As defined by the Fried Frailty Phenotype (FFP)2, frailty is an aggregate of 5 constructs: weight loss, exhaustion, low physical activity, slowness, and weakness. Other means of identifying frailty have been suggested that may be easier to implement in clinical settings, including a shorter performance-based method, the Short Physical Performance Battery (SPPB)3. We examined the prevalence of frailty using the SPPB in a well-characterized SLE cohort.
Methods: Data are from the California Lupus Epidemiology Study (CLUES), a longitudinal cohort of individuals with rheumatologist-confirmed SLE. Data are collected annually through in-person research visits and structured interviews. At one visit, the SPPB was administered to a subset of the cohort. SPPB consists of balance tests, time to complete 5 chair stands, and gait speed over 4 meters. Scores range from 0 – 12; a score of < 10 identifies frailty. Differences in participant characteristics for frail/not frail were examined using t-tests or chi-square analyses. Multivariate logistic regression analyses identified independent predictors of frailty, including age, sex, race/ethnicity, l, obesity, SLE duration, SLE disease activity, and steroid use. Separate models were constructed to include either physician-assessed (SLE Disease Activity Index, SLEDAI) or patient-reported disease activity (Systemic Lupus Activity Questionnaire). The impact of frailty on patient-reported outcomes (PROs) was examined with multiple regression analyses.
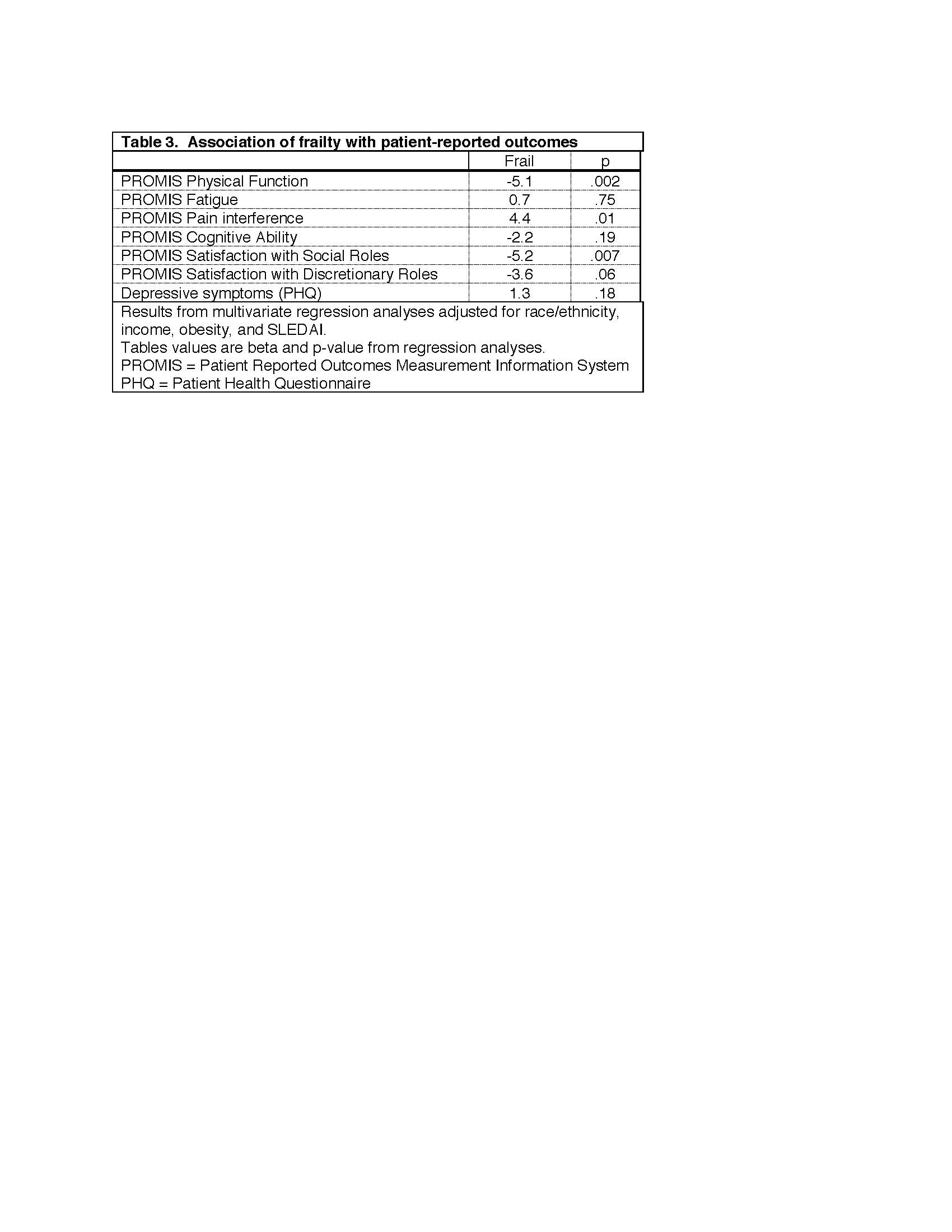
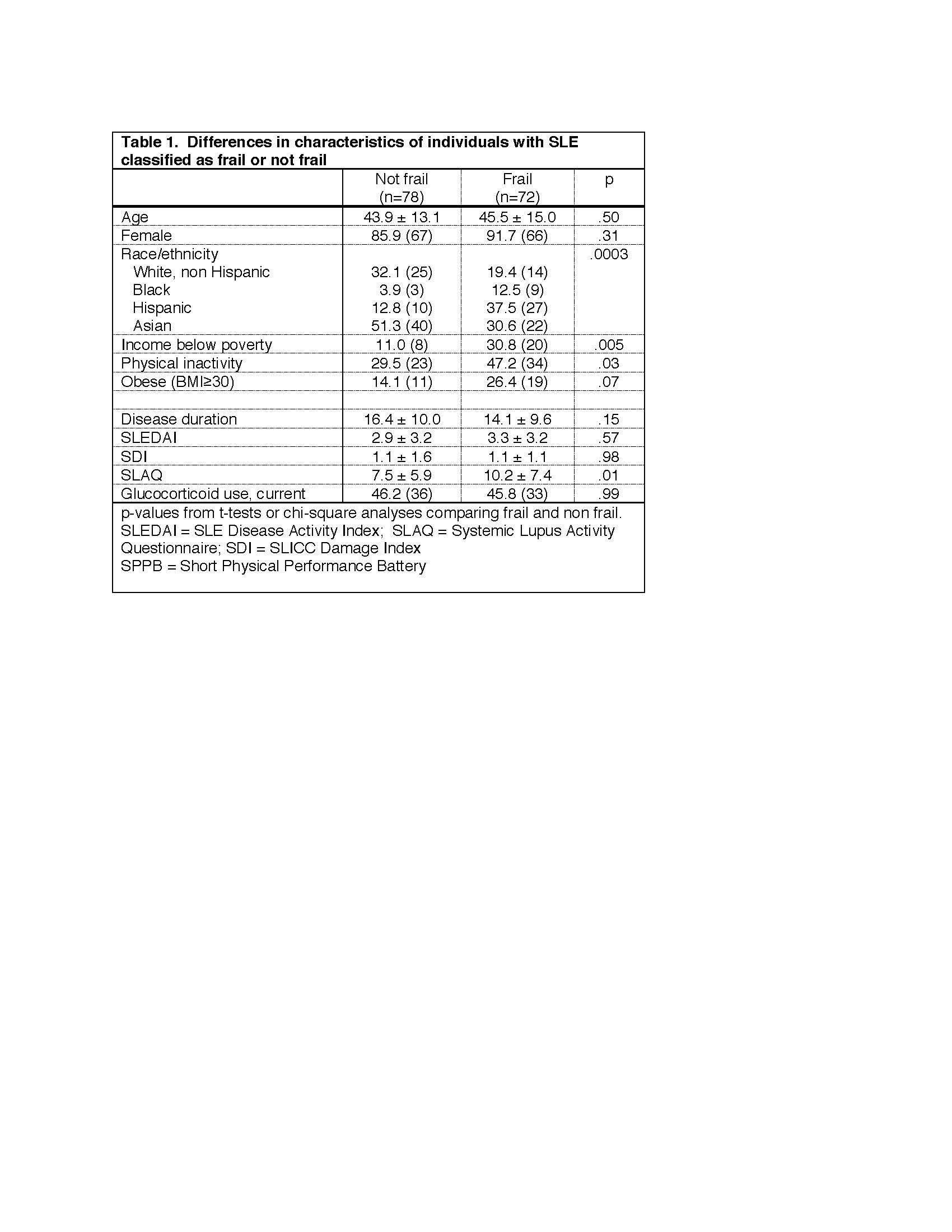
Results: Among the 150 individual who completed the SPPB, mean age was 45 ± 14 years, disease duration 15 ± 10 years, 89% were female, 41% Asian, 25% Hispanic, 26% white non-Hispanic, and 8% African American. The proportion of individuals classified as frail was 48% (Table 1). Factors associated with frailty in bivariate analyses were low income, obesity, physical inactivity, and patient-reported disease activity (Table 1). In multivariate analysis, only race/ethnicity remained a significant independent predictor of frailty (Hispanic only when adjusting for SLEDAI, Hispanic and African America when adjusting for SLAQ). In post-hoc analyses, obesity and inactivity were found to be significantly more common among Hispanics and African Americans (p< .01, not shown). Frailty was associated with worse scores on most PROs, even after adjusting for race/ethnicity, income, obesity, and physician-assessed disease activity (Table 3).
Conclusion: Using the SPPB, nearly half of this sample was identified as frail. A previous study using the FFP found 20% prevalence of frailty and 50% pre-frailty. Racial/ethnic differences were noted, but may be due to greater prevalence of obesity and inactivity among Hispanics and African Americans. Patient-reported outcomes were consistently worse among individuals classified as frail, even after adjusting for covariates. Interventions aimed at reducing inactivity may reduce frailty among individuals with SLE.
1 Katz P. Lupus Sci Med 2017;4:e000186
2 Fried L. J Gerontol 2001; 56:M146
3 Guralnik J. J Gerontol 1994; 49:M85
To cite this abstract in AMA style:
Katz P, Yazdany J, Trupin L, Rush S, Lanata C, Criswell L, Dall'Era M. Predictors of Frailty Identified by the Short Physical Performance Battery and Associations with Patient-reported Outcomes [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/predictors-of-frailty-identified-by-the-short-physical-performance-battery-and-associations-with-patient-reported-outcomes/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/predictors-of-frailty-identified-by-the-short-physical-performance-battery-and-associations-with-patient-reported-outcomes/