Session Information
Session Type: Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Oestrogen exposure leads to an increase in peak bone mass whereas menopause is associated with rapid bone loss. Numerous studies have linked rheumatoid arthritis (RA), systemic lupus erythematosus (SLE) and osteoarthritis to an earlier menopause; however, there are paucity of data in polymyalgia rheumatica (PMR). This study aims to establish whether PMR is associated with a later self-reported age of menopause.
Methods: Post menopausal patients who were referred for bone mineral density (BMD) estimation in a scanner in the North West of England between June 2004 and October 2015 were included in the analysis. All patients had their baseline demographics recorded at time of scan as well as risk factors for fracture including presence of PMR, RA, SLE and coeliac disease, excess alcohol intake, corticosteroid use, smoking history and parental family history of hip fracture. Bone mineral density (BMD) was measured at the left neck of femur and the lumbar spine. Patients were grouped into those with a clinician made diagnosis of PMR and those without; and initially compared using student’s T-test. Univariate and multivariate linear regression models were then fitted to examine associations with age of menopause in this group. All statistical analysis was performed using STATA v13, with results expressed as coefficients with 95% confidence intervals (95%CI).
Results: We recruited 14481 post-menopausal patients with a mean (SD) age of menopause of 65.5 years (10.8). 407 patients (2.8%) had a diagnosis of PMR, 63 (0.44%) patients with SLE, 832 (5.8%) with RA and 272 (1.9%) with coeliac disease. In this cohort, 4742 (32.8%) patient had a smoking history, 810 (5.6%) drank an excess of alcohol, 3157 (21.8%) were taking corticosteroids and 2428 (16.8%) had a parental family history of hip fracture. The mean age (SD) of patients was 65.5 (10.8) years. Mean age of menopause was later in patients with PMR (49.3 vs 48.2 years, mean difference 1.1 years, p=< 0.001). Results of the univariate analysis are shown in table 1. This analysis showed that PMR, increasing age and increased BMD in the lumbar spine are associated with a later age of menopause. Smoking and SLE, however, were associated with an earlier age of menopause. In the multivariable model when adjusting for all of the above, delayed menopause was still significantly associated with PMR (beta co-efficient 1.34 95% CI 0.72, 1.96, p< 0.001).
Conclusion: In this large observational study, women with PMR have a later onset of self reported menopause. This is the first study to establish this association between the age of menopause and PMR. Further studies will be required to confirm this association and review whether the age of menopause is a risk factor for PMR.
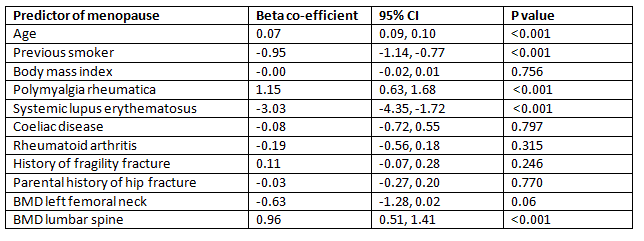 Table 1: Linear regression analysis of patient’s parameters with 95% confidence interval (CI). BMD, bone mineral density.
Table 1: Linear regression analysis of patient’s parameters with 95% confidence interval (CI). BMD, bone mineral density.
To cite this abstract in AMA style:
Dyball S, Saleh C, Bukhari M. Polymyalgia Rheumatica Is Associated with Later Menopause: An Observational Study [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/polymyalgia-rheumatica-is-associated-with-later-menopause-an-observational-study/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/polymyalgia-rheumatica-is-associated-with-later-menopause-an-observational-study/
