Session Information
Session Type: ACR Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose: Anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV) is an autoimmune disease that affects small- to medium-sized blood vessels and causes vascular inflammation and multiple organ damage. The pathogenesis of AAV is still unclear. However, neutrophil extracellular traps (NETs) is thought to be one of important triggers of vascular endothelial dysfunction in the disease process of AAV, and it is recently reported that platelets stimulated via toll-like receptor (TLR) pathways can induce NETs formation. Thus, platelets may be alternative key players in AAV pathogenesis. In this study, we investigated the role of platelets and involvement of TLR signaling in the process of NETs formation in patients with AAV.
Methods: Twenty-one patients with AAV (granulomatosis with polyangiitis [GPA]: n=12, microscopic polyangiitis [MPA]: n=9) who visited Keio University Hospital between August 2017 and October 2018 were consecutively enrolled. Ten SLE, 12 RA, and 20 healthy controls (HCs) were included as controls. All AAV patients fulfilled the 2012 Revised International Chapel Hill Consensus Conference Nomenclature. Expression of platelet-associated TLRs were examined using flow cytometry. Clinical information was obtained from patients’ record and association with expression of TLR was also examined. In order to examine functional involvement of platelets in NETs formation, platelets from AAV patients or HCs were co-cultured with peripheral neutrophils. In some experiments, platelets were stimulated with TLR agonist in advance. NETs formation visualized by Picogreen was detected and quantified using confocal fluorescent microscopy.
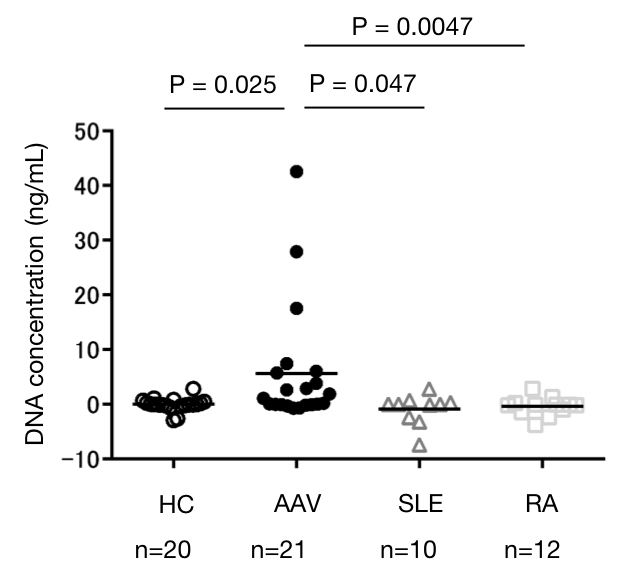
Results: As shown in the figure, platelets from AAV patients increased NETs formation compared with those from RA (p=0.0047), SLE (p=0.047) or HC (p=0.025). Flow cytometric analysis revealed that the expression of TLR9 (p=0.0011) but not other TLRs, such as TLR2 (p=0.71) and TLR4 (p=0.93), in platelets was elevated in platelets from AAV patients compared with HCs. In particular, the proportion of TLR9+platelets was elevated in patients with pulmonary involvement compared with those without (p=0.012), and was correlated with patients’ serum Krebs Von Den Lungen-6 level (r2=0.31, p=0.049). Interestingly, we found that TLR9 agonist (CpG oligodeoxynucleotides)-stimulated platelets from AAV patients induced NETs formation compared with control oligodeoxynucleotides-stimulated platelets.
Conclusion: These results suggest that platelets play a key role in NETs formation in the pathogenesis of AAV and TLR9 signaling is involved in this process.
To cite this abstract in AMA style:
Matsumoto K, Yasuoka H, Suzuki K, Takeuchi T. Platelet Mediates Neutrophil Extracellular Traps Formation via TLR Signaling in ANCA-associated Vasculitis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/platelet-mediates-neutrophil-extracellular-traps-formation-via-tlr-signaling-in-anca-associated-vasculitis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/platelet-mediates-neutrophil-extracellular-traps-formation-via-tlr-signaling-in-anca-associated-vasculitis/