Session Information
The 2020 Pediatric Rheumatology Symposium, originally scheduled for April 29 – May 2, was postponed due to COVID-19; therefore, abstracts were not presented as scheduled.
Session Type: Poster Breakout Session
Session Time: 4:30PM-5:00PM
Background/Purpose: Adverse Childhood Experiences (ACEs) have been recognized for more than two decades as risk factors for poor health outcomes in adults. Nevertheless, the impact of patient exposure to ACEs on outcomes in pediatric chronic disease has yet to be fully explored. To date, there have been no studies examining the impact of parental ACE burden on disease control in pediatric chronic disease. This study assessed parental ACE burden and disease activity in youth ages 12-17 with pediatric systemic lupus erythematosus (pSLE).
Methods: Patients were eligible for inclusion if English speaking, 12-17 years old, met ACR or SLICC classification criteria for SLE, had SLE duration of diagnosis ≥ 6 months, and had been seen in our clinic in the past year. Parents were eligible if they spoke English or Spanish. Eligible patient/parent dyads were identified on a weekly basis by reviewing the clinic schedule. Parents completed a demographic survey, CDC-Kaiser Permanente ACE questionnaire, Perceived Stress Scale (PSS), and Brief Resilient Coping Scale (BRCS). Patients were asked to complete the Morisky Medication Adherence Scale (MMAS-4), and their demographic and disease-related data were extracted from the medical record. Univariate analyses were conducted to determine associations between several variables and disease activity (SLEDAI-2K). Multivariate analysis was conducted to determine if an association existed between parental ACE burden and disease activity while controlling for several variables felt to be potential modulators of disease control.
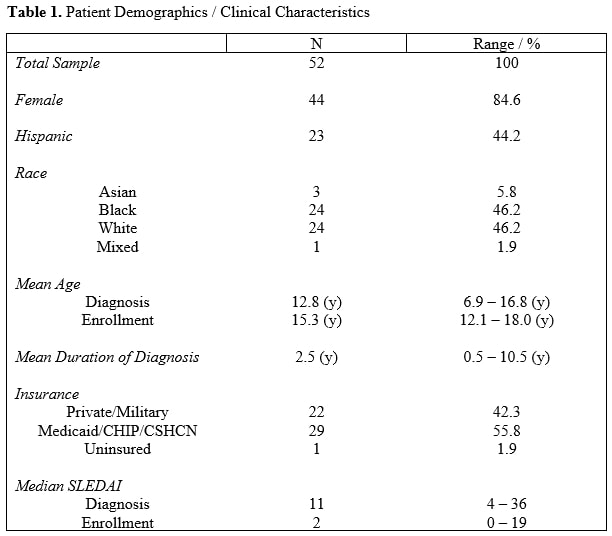
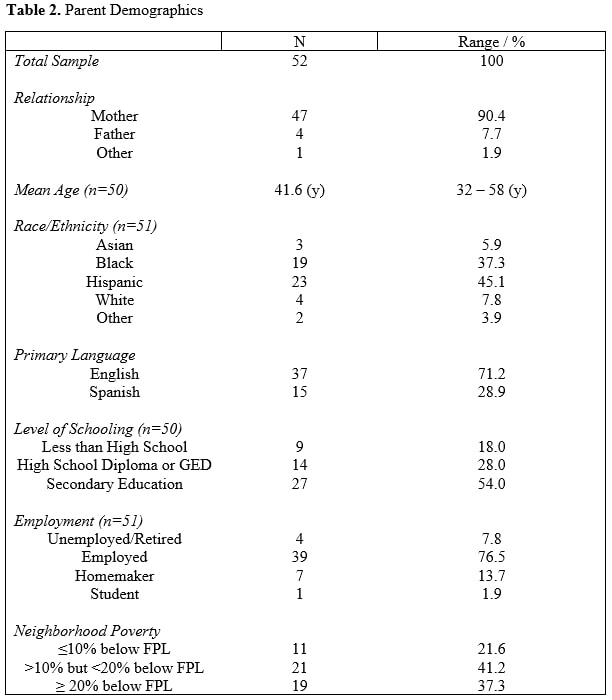
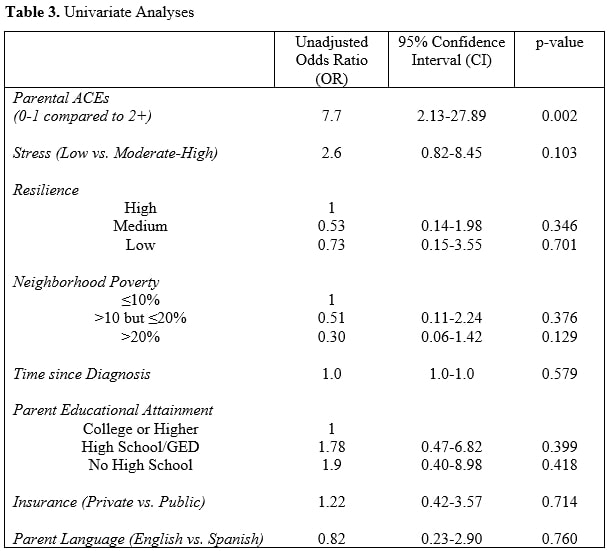
Results: A total of 52 patient/parent dyads were enrolled in the study between May 2019 and January 2020. Patient demographics and clinical characteristics are found in Table 1 and parent demographics in Table 2. Eighteen (34%) parents reported 2 or more ACEs. Twenty-seven (52%) and 25 (48%) parents reported low and moderate-high perceived stress during the past 30 days, respectively. Sixteen (31%), 24 (47%), and 11 (22%) parents were identified as high, medium, and low resilient copers, respectively. In univariate analyses of low vs. moderate-high perceived level of stress over the past 30 days, resilient coping ability, neighborhood poverty, time since diagnosis, parent education, type of insurance (public vs. private/military), and parent primary language, none of these were found to predict active lupus (SLEDAI-2K ≥ 3) at the time of visit (Table 3). However, parental ACE burden of 2 or more was predictive of active lupus (OR = 7.7, 95% CI: 2.13-27.89). MMAS-4 was neither predictive of active disease nor was it affected by parental ACE burden. After controlling for parent reported stress over the past 30 days, insurance type, parent language, and time from diagnosis, parent reported burden of 2 or more ACEs was predictive of active lupus at the time of visit (OR = 6.9, 95% CI: 1.76-27.43).
Conclusion: Our data suggest that parental exposure to 2 or more ACEs is an important risk factor for more active disease in pediatric lupus. As such, screening for parental ACEs may be helpful in identifying youth at higher risk for active lupus. More work needs to be done to determine the manner by which parental ACE burden mediates increased lupus activity and methods to mitigate the harms.
To cite this abstract in AMA style:
Nelson M, Correa N, Butler A, De Guzman M, Van Horne B, Greeley C. Parental Adverse Childhood Experience (ACE) Exposure Is Predictive of Active Lupus in Pediatric Patients [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 4). https://acrabstracts.org/abstract/parental-adverse-childhood-experience-ace-exposure-is-predictive-of-active-lupus-in-pediatric-patients/. Accessed .« Back to 2020 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/parental-adverse-childhood-experience-ace-exposure-is-predictive-of-active-lupus-in-pediatric-patients/