Session Information
Date: Saturday, November 6, 2021
Title: Fibromyalgia & Other Clinical Pain Syndromes Poster (0118–0127)
Session Type: Poster Session A
Session Time: 8:30AM-10:30AM
Background/Purpose: Pain accounts for greater than 40% of all symptom-related outpatient visits totaling over 100 million outpatient encounters worth hundreds of billions of dollars annually in the U.S alone. Face-to-face and internet-delivered web-based cognitive behavioral therapy (CBT) have proven safe and effective in managing chronic musculoskeletal pain (CMP), demonstrating clinically significant improvements in pain-related disability and severity. Nonetheless, the effect size for CBT in CMP has been small partly due to low compliance or engagement by study participants. The purpose of this pilot study was to evaluate the effectiveness of nurse-supported web-based CBT in the outpatient setting for management of CMP.
Methods: Sixty subjects with CMP were recruited from the internal medicine and rheumatology clinics at Wake Forest Baptist Medical Center. Subjects were randomized to web-based self-guided CBT with six phone-based nurse support calls (nurse support group, n=30) vs. web-based self-guided CBT alone (control group, n=30). The purpose of the phone calls was to encourage completion of the eight learning modules within the web-based CBT program. The nurse support calls were made from baseline to week 8. All participants had access to the CBT program from baseline to week 16. Outcome measures were collected at baseline, week 8, and week 16.
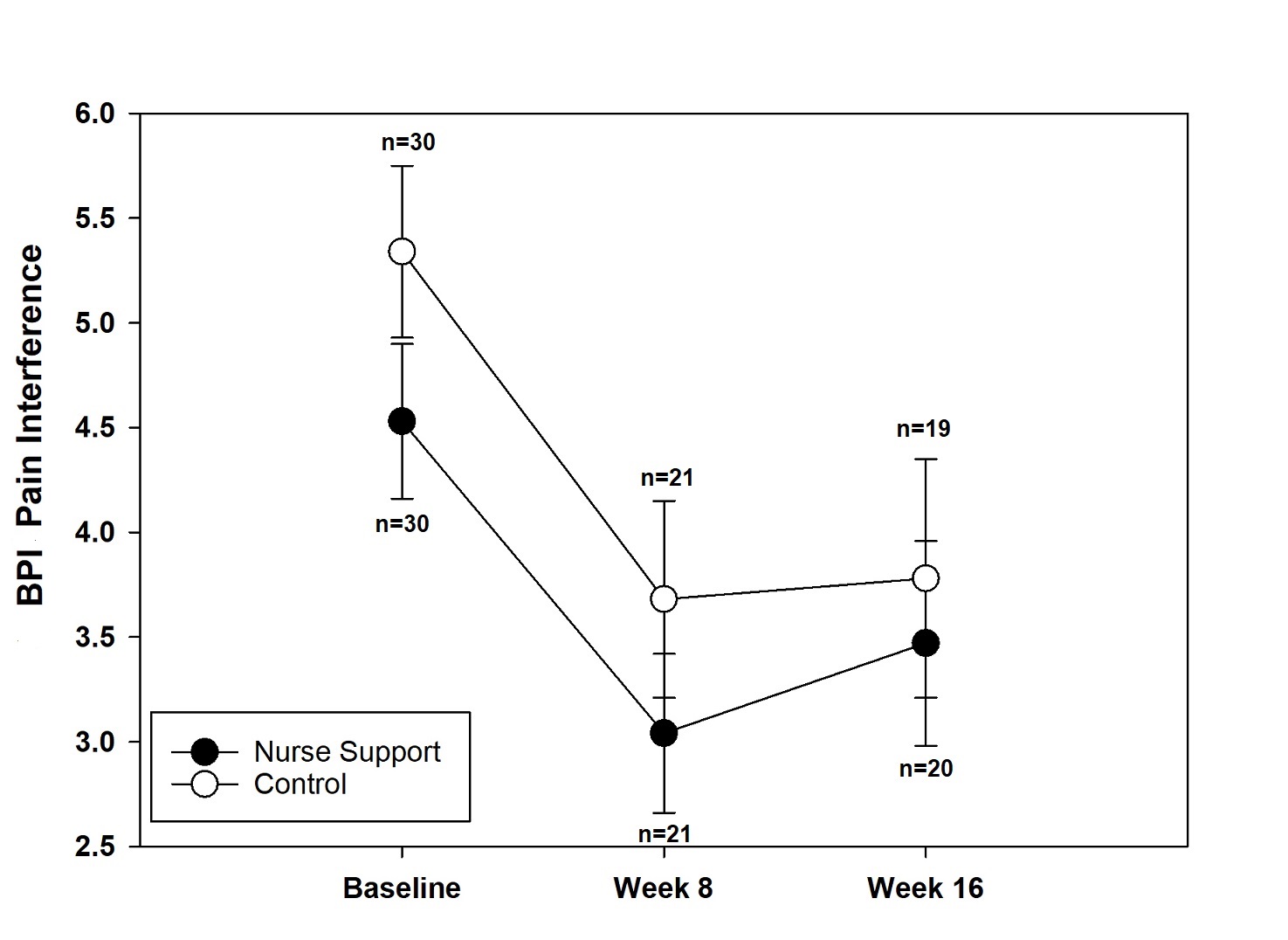
Results: Using analysis of covariance (ANCOVA) of week 8 and 16 outcome measures, both nurse support and control groups showed statistically significant improvements from baseline in BPI pain intensity (-1.2 [-1.7, -0.6], P< 0.05; -1.3 [-1.8, -0.8], P< 0.05), BPI pain interference (-1.3 [-2.0, -0.7], P< 0.05; -1.7 [-2.3, -1.0], P< 0.05), and BPI global pain severity (-1.2 [-1.7, -0.8], P< 0.05; -1.5 [-1.9, -1.0], P< 0.05) scores respectively. Amongst all secondary outcome measures, only the PROMIS sleep disturbance showed significant differences between the two groups and favored the nurse support group over the control group (50.5 [1.3] vs. 54.3 [1.3]; P=0.039). All subjects had comparable baseline characteristics including duration of pain ≥ 1 year, number of painful body sites (≥3 vs. < 3), Brief Pain Inventory (BPI) pain intensity, interference, and global pain severity scores (range 0-10), Patient-Reported Outcomes Measurement Information System (PROMIS) measures, Patient Health Questionnaire (PHQ-8) depression scale scores (≥ 10), and pain catastrophizing scores. Twenty (66.7%) of patients in the nurse support group vs. 19 (63.3%) of patients in the control group completed the study. The proportion of subjects who completed ≥ 6 learning modules were 17 (56.7%) in the treatment group vs. 18 (62.1%) in the control group. From baseline to week 8, the median number of completed phone calls made by the nurses were 3.5 calls (Interquartile Range [IQR]: 2, 5) and the median duration of each phone call was about 7 minutes (IQR: 5, 10).
Conclusion: Web-based CBT alone showed similar benefits in pain relief and pain-related disability in comparison to web-based CBT with phone-based nurse support over the short term. If confirmed in a larger study, web-based CBT without phone-based nurse support should be routinely included in any treatment algorithm for CMP.
To cite this abstract in AMA style:
Diab R, Bomar R, Rinaldi C, Campos C, Kaplan S, Ang D. Nurse-supported Web-based Cognitive Behavioral Therapy for Chronic Musculoskeletal Pain: An Effectiveness Trial [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/nurse-supported-web-based-cognitive-behavioral-therapy-for-chronic-musculoskeletal-pain-an-effectiveness-trial/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/nurse-supported-web-based-cognitive-behavioral-therapy-for-chronic-musculoskeletal-pain-an-effectiveness-trial/