Session Information
Session Type: Poster Session C
Session Time: 8:30AM-10:30AM
Background/Purpose: The rheumatology workforce faces a shortage in the decade ahead. Internal Medicine (IM) residents comprise the pipeline of physicians who will care for rheumatology patients in general medicine, rheumatology, and other specialties. However, many IM residencies lack formal training on rheumatologic diseases. This needs assessment investigated IM residents’ interest, competence, and preferred format of learning rheumatology topics. Results will guide the development of a curriculum to enhance rheumatology teaching for medicine trainees.
Methods: The study population consisted of IM residents at a university hospital (Program A, n=116) and a community hospital (Program B, n= 23). Residents’ objective knowledge of rheumatology was assessed via In-Training Exam (ITE) scores from 2020. Their confidence and interest in clinical rheumatology was assessed through an anonymous survey. The survey queried residents’ confidence in and interest in learning about six skills: conducting a rheumatology review of systems, performing a large joint exam, performing a small joint exam, ordering appropriate labs for autoimmune diseases, interpreting labs for autoimmune diseases, and deciding when to consult rheumatology. It also assessed residents’ confidence in diagnosing and managing, and interest in learning about, eight rheumatologic disease categories: crystal-induced arthropathies, infectious arthritis, osteoarthritis, rheumatoid arthritis, spondyloarthropathies, lupus, systemic sclerosis, and vasculitis. Survey questions were presented on five-point Likert scales.
Results: On the 2020 ITE, rheumatology was the subspecialty with the lowest average score for residents nationwide (59%), at Program A (60%), and tied for lowest at Program B (48%). Surveys were completed by 53/116 (46%) of residents at Program A and 20/23 (87%) of residents at Program B. Responses were similar between Program A and B across all questions, and are presented as aggregate scores. Average interest in learning about rheumatology was 3.8/5, between “neutral” and “somewhat interested.” Average rating of the amount of rheumatology training received in residency was 2.3/5, between “somewhat inadequate” and “neutral.” Confidence in rheumatology skills is presented in Figure 1. Confidence in diagnosing and managing specific rheumatologic conditions is presented in Figure 2. Interest in learning about rheumatology topics is presented in Figure 3. Topics for which residents expressed lowest confidence and highest interest included: ordering and interpreting labs for autoimmune diseases, lupus, vasculitis, and systemic sclerosis. Residents identified noon conference and online self-paced modules as the preferred curriculum formats.
Conclusion: IM residents at both programs demonstrated objective deficits in rheumatology knowledge on the ITE, as well as self-reported need and interest in more rheumatology training. ITE scores and our survey results highlight the urgent need to better address rheumatology training for IM residents nationwide. The study team is developing a series of noon conference sessions for IM residents on the topics identified above, to be recorded and archived for future use.
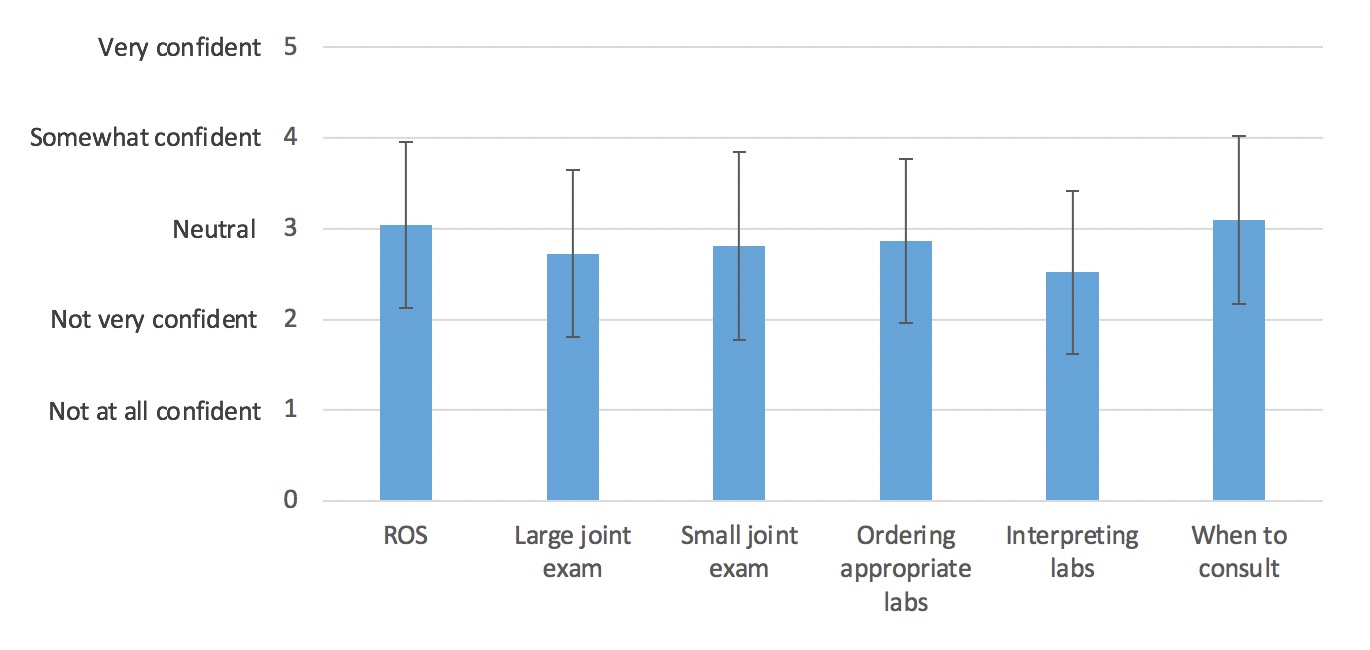 Figure 1: Residents’ confidence in rheumatology skills (n=73). Average scores on a 5-point Likert scale are presented, with error bars indicating one standard deviation.
Figure 1: Residents’ confidence in rheumatology skills (n=73). Average scores on a 5-point Likert scale are presented, with error bars indicating one standard deviation.
 Figure 2: Residents’ confidence in diagnosing (left bar) and managing (right bar) rheumatologic conditions (n=73). Average scores on a 5-point Likert scale are presented, with error bars indicating one standard deviation.
Figure 2: Residents’ confidence in diagnosing (left bar) and managing (right bar) rheumatologic conditions (n=73). Average scores on a 5-point Likert scale are presented, with error bars indicating one standard deviation.
 Figure 3: Residents’ interest in learning about rheumatology topics (n=72). Average scores on a 5-point Likert scale are presented, with error bars indicating one standard deviation.
Figure 3: Residents’ interest in learning about rheumatology topics (n=72). Average scores on a 5-point Likert scale are presented, with error bars indicating one standard deviation.
To cite this abstract in AMA style:
Arneson L, Modilevsky B, Lima K, Fantus S, Dua A. Needs Assessment of a Rheumatology Curriculum for Internal Medicine Residents [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/needs-assessment-of-a-rheumatology-curriculum-for-internal-medicine-residents/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/needs-assessment-of-a-rheumatology-curriculum-for-internal-medicine-residents/
