Session Information
Session Type: Abstract Session
Session Time: 11:00AM-11:50AM
Background/Purpose: Nasal bacteria have been linked to disease activity in granulomatosis with polyangiitis (GPA) with most studies focused on Staphylococcus aureus. Our previous study identified dynamic changes in the ratio of nasal Corynebacterium to Staphylococcus (at the genus level) prior to and during a relapse. Corynebacteria are a common commensal that inhabits the skin and nose and is known to directly interact with S. aureus. The objective of this study was to evaluate species-level identity of nasal bacteria and their association with disease activity and ANCA levels in GPA.
Methods: Nasal bacterial composition was examined using 16S rRNA gene sequencing of nasal swabs of 19 patients with GPA followed longitudinally approximately every 3 months (N = 76 visits, median time between visits 4 months). Nine patients had at least 1 visit with active disease and 10 patients remained in remission during follow-up. Disease activity was determined by BVAS/WG. Only PR3-ANCA results obtained by ELISA at the study site were included for ANCA analyses (11 patients with 29 visits). We evaluated the relative abundance of the 10 most abundant bacterial species across all visits as well as the ratios between these 10 species. Generalized estimating equations evaluated the association between bacteria and i) visit type (stable remission [n=41], pre-pre-relapse [n=4], pre-relapse [n=10], relapse [n=10], post-relapse [n=9]), and ii) ANCA levels, accounting for repeated measures within an individual. Test for trend examined linear trends in bacterial abundance across visit types. Models were adjusted for use of antibiotics, immunosuppressive medications, nasal irrigation, and, when analyzing Corynebacteria, presence of S. aureus.
Results: Corynebacterium tuberculostearicum featured prominently in our analyses. Specifically, we found the abundance of C. tuberculostearicum significantly increased across visit types in GPA when evaluating any relapse (adjusted P = 0.04; Figure 1) and relapse involving the sinonasal area (adjusted P < 0.01). The presence of S. aureus (32/76 visits [42%]) was independently associated with a higher C. tuberculostearicum abundance (adjusted P = 0.02). C. tuberculostearicum abundance was associated with higher levels of PR3-ANCA (adjusted P = 0.02; Figure 2). Analysis of bacterial ratios identified significantly increasing ratios of C. tuberculostearicum to S. caprae abundance and C. pseudodiphtheriticum to S. caprae abundance across visit types (both adjusted P < 0.01; Figure 3).
Conclusion: Our species-level analysis has uncovered a novel finding between C. tuberculostearicum and both disease relapse and ANCA levels in GPA. Our results also detected associations between C. tuberculostearicum and Staphylococcus species, including S. aureus. Prior studies demonstrated a pathogenic role for C. tuberculostearicum in chronic rhinosinusitis and direct interactions between Corynebacterium spp. and S. aureus. We propose that competitive interactions between Corynebacteria and Staphylococci induce nasal mucosal immune responses which, in susceptible hosts predisposed to autoimmunity and ANCA formation, lead to systemic relapse in GPA.
 Figure 1. Increasing abundance of nasal Corynebacterium tuberculostearicum is associated with relapse in granulomatosis with polyangiitis (GPA). Longitudinal study visits categorized by visit type: stable remission (n=41), pre-pre-relapse remission (n=4), pre-relapse remission (n=10), relapse (n=12), and post-relapse remission (n=9). Test for trend detected a significant linear increase in nasal C. tuberculostearicum abundance across visits even after adjusting for antibiotics, immunosuppressives, nasal irrigation, and presence of S. aureus (adjusted P = 0.04). Similar results found when analyzing only relapses involving sinonasal area.
Figure 1. Increasing abundance of nasal Corynebacterium tuberculostearicum is associated with relapse in granulomatosis with polyangiitis (GPA). Longitudinal study visits categorized by visit type: stable remission (n=41), pre-pre-relapse remission (n=4), pre-relapse remission (n=10), relapse (n=12), and post-relapse remission (n=9). Test for trend detected a significant linear increase in nasal C. tuberculostearicum abundance across visits even after adjusting for antibiotics, immunosuppressives, nasal irrigation, and presence of S. aureus (adjusted P = 0.04). Similar results found when analyzing only relapses involving sinonasal area.
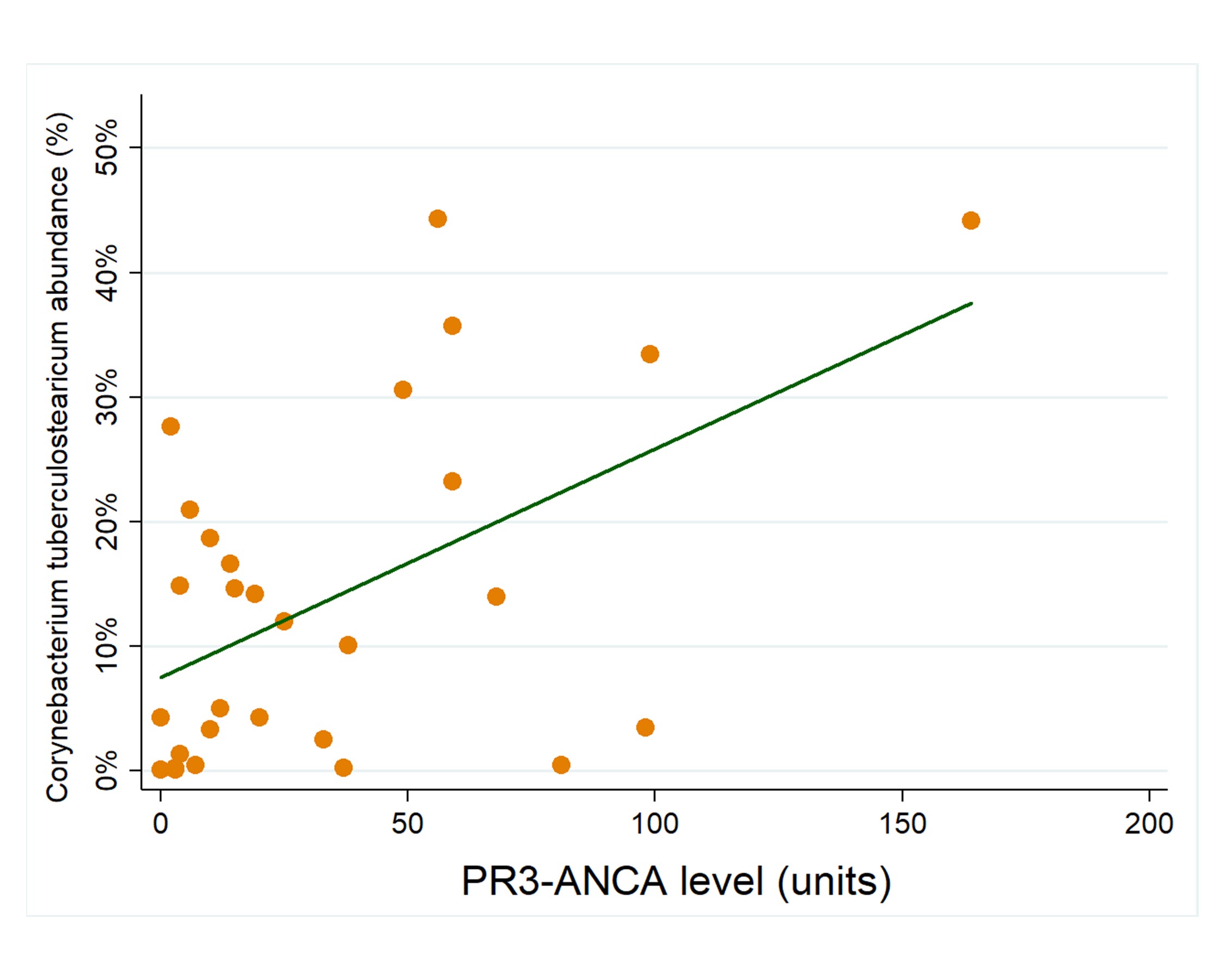 Figure 2. Relative abundance of nasal Corynebacterium tuberculostearicum is associated with PR3-ANCA level in granulomatosis with polyangiitis (GPA). Scatterplot demonstrates association between abundance of nasal C. tuberculostearicum and serum PR3-ANCA levels in 11 patients with total of 29 visits (unadjusted P < 0.01). Association remained significant even after adjusting for use of antibiotics, immunosuppressives, and nasal irrigation (adjusted P = 0.02). Reference range for normal PR3-ANCA < 20 units.
Figure 2. Relative abundance of nasal Corynebacterium tuberculostearicum is associated with PR3-ANCA level in granulomatosis with polyangiitis (GPA). Scatterplot demonstrates association between abundance of nasal C. tuberculostearicum and serum PR3-ANCA levels in 11 patients with total of 29 visits (unadjusted P < 0.01). Association remained significant even after adjusting for use of antibiotics, immunosuppressives, and nasal irrigation (adjusted P = 0.02). Reference range for normal PR3-ANCA < 20 units.
 Figure 3. Ratio of bacteria associated with relapse in granulomatosis with polyangiitis (GPA). Ratio of bacterial abundance were log-transformed and test for trend evaluated for changes across visit types. An increasing ratio of Corynebacterium tuberculostearicum to Staphylococcus caprae and C. pseudodiphtheriticum to S. caprae were both associated with visit type, even after adjusting for antibiotics, immunosuppressives, and nasal irrigation (both adjusted P < 0.01).
Figure 3. Ratio of bacteria associated with relapse in granulomatosis with polyangiitis (GPA). Ratio of bacterial abundance were log-transformed and test for trend evaluated for changes across visit types. An increasing ratio of Corynebacterium tuberculostearicum to Staphylococcus caprae and C. pseudodiphtheriticum to S. caprae were both associated with visit type, even after adjusting for antibiotics, immunosuppressives, and nasal irrigation (both adjusted P < 0.01).
To cite this abstract in AMA style:
Rhee R, Lu J, Bittinger K, Sreih A, Lee J, Mattei L, Kelly B, Grayson P, Lee H, Collman R, Merkel P. Nasal Bacteria Associated with Disease Activity and ANCA Levels in Granulomatosis with Polyangiitis [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/nasal-bacteria-associated-with-disease-activity-and-anca-levels-in-granulomatosis-with-polyangiitis/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/nasal-bacteria-associated-with-disease-activity-and-anca-levels-in-granulomatosis-with-polyangiitis/
