Session Information
Date: Saturday, November 6, 2021
Title: RA – Diagnosis, Manifestations, & Outcomes Poster I: Cardiovascular Pulmonary Disease (0268–0295)
Session Type: Poster Session A
Session Time: 8:30AM-10:30AM
Background/Purpose: In Rheumatoid arthritis (RA), immune dysregulation, excess inflammation and oxidative stress may alter lipoprotein level and function and promote LDL oxidation and its uptake by vessel wall macrophages. The cell cholesterol loading capacity of serum (CLC)- as a reflection of both lipoprotein quantity and quality- may be an essential step in foam cell formation, the establishment and progression of atherosclerosis. RA therapies may modify atherosclerosis trajectory by intercepting several of those processes. We evaluated the relationship of inflammation, LDL particle structure, oxidation and immune system recognition of oxidized epitopes with CLC. We next evaluated interactions between RA treatments and these processes on macrophage cholesterol loading.
Methods: 107 RA patients from our previously described PROTECT-RA cohort with coronary atherosclerosis evaluation were studied. Lipoprotein classes and subclasses and their cholesterol content were directly measured using single vertical spin density gradient ultracentrifugation. Oxidized LDL (oxLDL) was measured with monoclonal antibody E06. IgM and IgG antibodies to oxLDL (anti-oxLDL) were assessed with chemiluminescence Elisa. Proinflammatory cytokines were measured with microparticle immunoassay and singe molecule counting (Erenna, Singulex). CLC was measured by fluorometric assay- as macrophage cholesterol content- after a 24-hour incubation with whole serum. Robust, multivariable generalized linear models evaluated associations between inflammation, LDL particle content, LDL oxidation and antibodies against oxLDL with CLC. Similar models explored interactions between RA treatments and markers of inflammation on CLC.
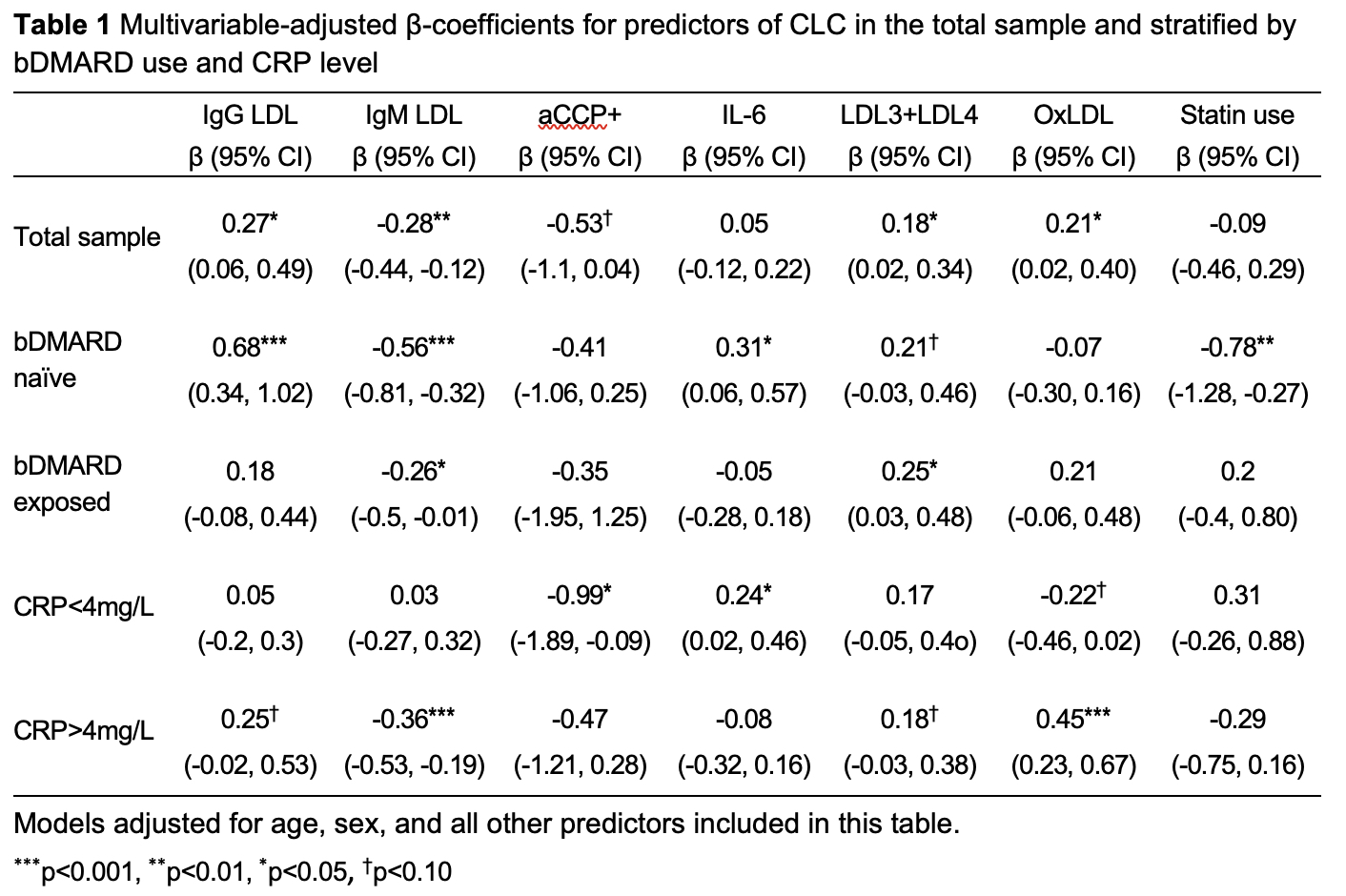
Results: Patients were middle aged (53.9 10.7), mostly female (86%) with seropositive (92%), erosive (66.4%) and well controlled disease (DAS28= 2.49 0.96). Smaller-sized LDL3 and LDL4 levels, oxLDL and anti-oxLDL IgG levels positively associated with CLC (all p < 0.032, Table 1); in contrast, anti-oxLDL IgM levels negatively associated with CLC (adjusted β= -0.28 [95% CI -0.44,-0.12], p=0.001). Inflammation modified the effect of LDL oxidation on CLC (p for interaction= 0.001); oxLDL significantly associated with CLC (adjusted β= 0.45 [95% CI 0.23-0.67], p< 0.001) in patients with CRP > 4mg/L (median split), but not those with CRP < 4mg/L. Significant interactions between bDMARD use and Interleukin-6 levels (p= 0.031) and between bDMARD and statin use (p= 0.038) on CLC were also observed. In bDMARD-naïve patients, interleukin-6 positively associated with CLC (adjusted β= 0.31 [95% CI 0.06-0.57], p=0.017) whereas statin use negatively associated with CLC (adjusted β= -0.78 [95% CI -1.28, -0.27], p= 0.003). Neither interleukin-6 nor statin use related to CLC in bDMARD-exposed patients.
Conclusion: Higher content of smaller-sized, readily oxidizable LDL subclasses, greater oxLDL levels -especially in the context of higher inflammation- and greater anti-oxLDL IgG serum concentration associated with greater cholesterol macrophage loading in RA. bDMARD therapies modified the impact of inflammation, lipid particle structure and statin use on CLC.
To cite this abstract in AMA style:
Karpouzas G, Papotti B, ormseth s, Palumbo M, Hernandez E, Marchi C, Zimetti F, Bernini F, Ronda N. Macrophage Cholesterol Loading Associates with Low-density Lipoprotein Structure, Oxidation, Antibodies Against Oxidized Epitopes and Is Modified by Immunomodulatory Treatments in Patients with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/macrophage-cholesterol-loading-associates-with-low-density-lipoprotein-structure-oxidation-antibodies-against-oxidized-epitopes-and-is-modified-by-immunomodulatory-treatments-in-patients-with-rheuma/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/macrophage-cholesterol-loading-associates-with-low-density-lipoprotein-structure-oxidation-antibodies-against-oxidized-epitopes-and-is-modified-by-immunomodulatory-treatments-in-patients-with-rheuma/