Session Information
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Intestinal microbial dysbiosis in patients with rheumatoid arthritis (RA) has raised the interest in studying the role of intestinal microbes in the pathogenesis of RA. Animals studies indicate that intestinal microbiota changes prior to the onset of visible inflammatory arthritis. Here, we undertook this study to clarify the intestinal microbiota changes in individuals at high risk for RA with the aim to identify bacteria biomarkers associated with the progression of RA.
Methods: High-risk for RA individuals were defined as having a positive serum antibody for anti-cyclic citrullinated peptide (CCP), without reported arthritis symptoms at the time of enrollment. RA patients were diagnosed according to the American College of Rheumatology (ACR) 2010 classification for RA. Age and gender matched anti-CCP negative healthy individuals were recruited as controls. Individuals having a history of antibiotics treatment in the last six months or other conditions that may affect the study were excluded. The 16S ribosomal RNA of fecal samples from 31 RA patients, 42 high-risk individuals and 38 healthy controls (HC) were sequenced and analyzed.
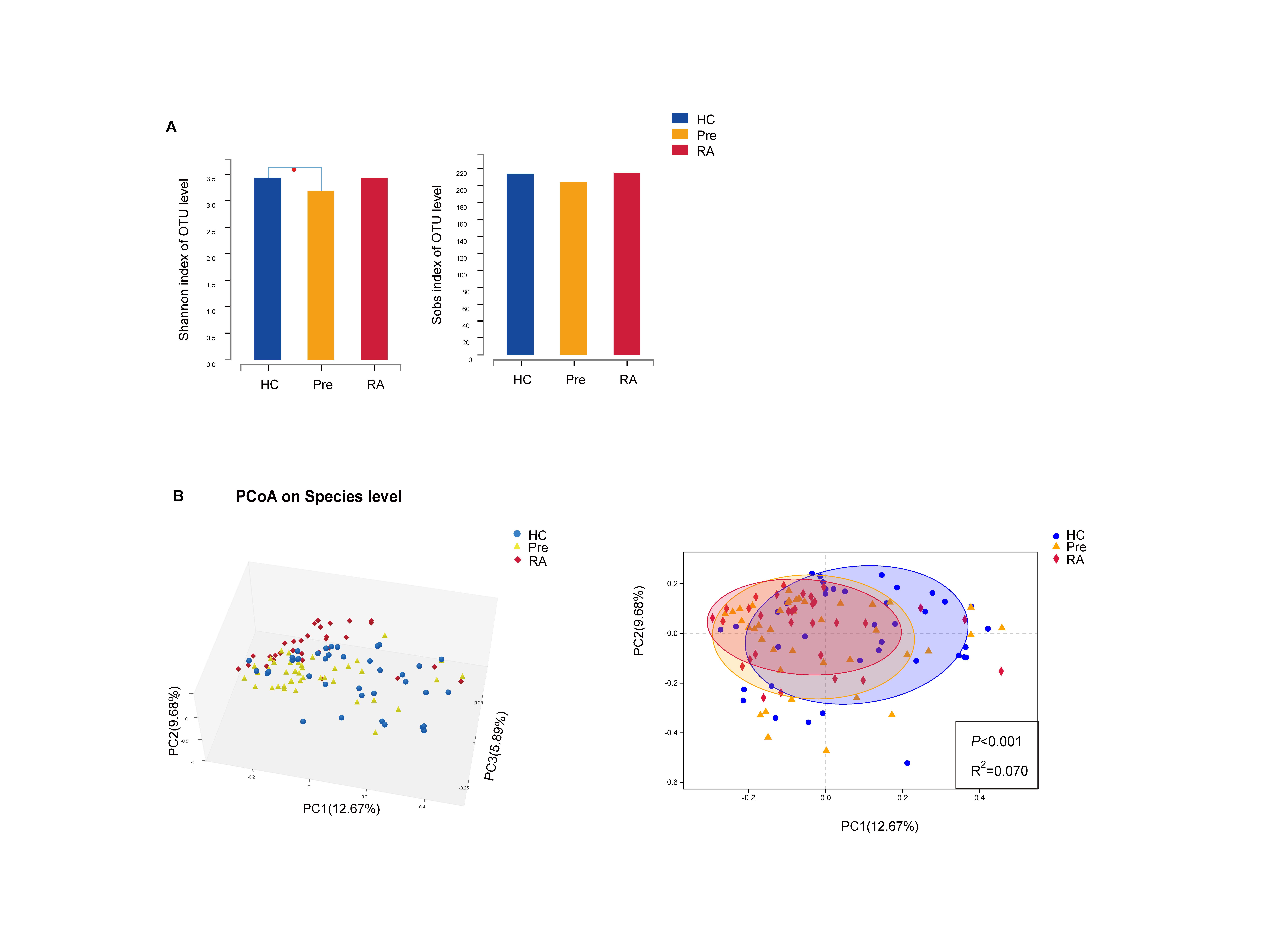
Results: Alpha diversity analysis showed that the intestinal microbiota communities in high-risk group (“pre” group) had a lower community diversity (Shannon index) than the healthy controls (Fig.1A). Beta diversity using principal coordinate analysis (PCoA) revealed that the intestinal microbiota was significantly different between groups (Fig.1B). Interestingly, we observed that the intestinal microbiota communities dynamically shifted from HCs to high-risk individuals (Pre) to RA patients.
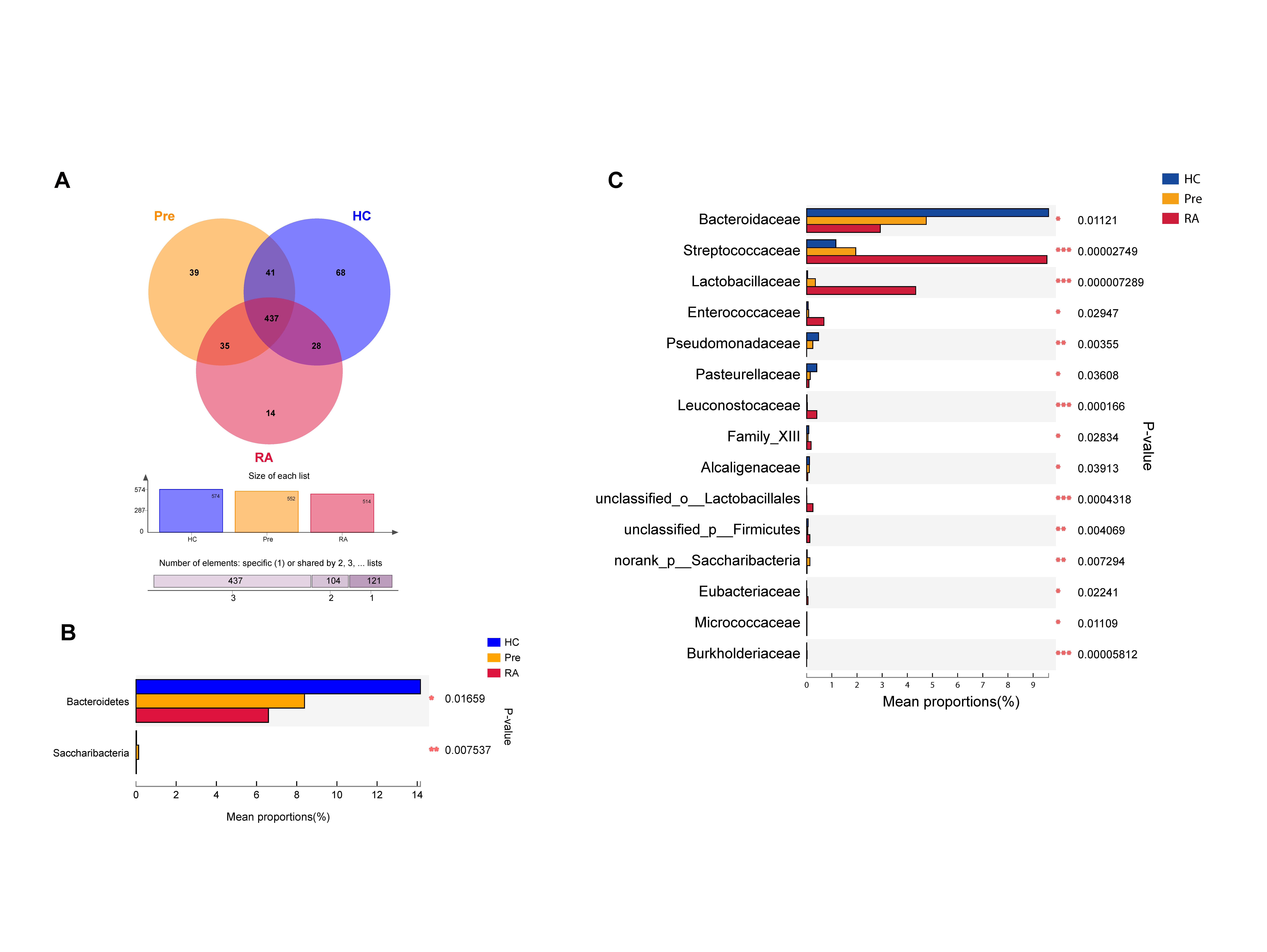
The majority of species (437) were shared by all groups. 35 species were found only in high-risk individuals and RA patients (Fig. 2A). Besides, the abundance of the microflora variant between groups. At the phylum level, the abundance of Bacteroidetes gradually decreased from HCs to high-risk individuals to RA patients. The abundance of Saccharibacteria were particularly higher in high-risk individuals than in both RA patients and HCs (Fig. 2B). Further to the family level, Bacteroidaceae, Pseudomonadaceae and Pasteurellaceae showed the same trend of gradual reduction from the HCs to high-risk individuals and to RA patients. On the contrary, an enriched abundance of Streptococcaceae, Lactobacillaceae, Enterococcaceae and Leuconostocaceae were seen in RA patients (Fig. 2C).
To determine taxonomic biomarkers that characterize the differences in the progression of RA, linear discriminant analysis (LDA) analysis was performed (Fig. 3A). We identified potential disease stage specific bacteria. A marker panel of six bacteria species was selected, which had an AUC of 0.78 (95%CI=0.66-0.9) in discriminating RA patients from HCs (Fig. 3B and 3C).
Conclusion: The intestinal microbiota changed gradually during disease progression of human RA. Intestinal dysbiosis occurs prior to the onset of arthritis symptoms in individuals with positive anti-CCP antibody. Identifying the specific microbes characterize individuals at preclinical stage would provide a useful tool for early detection and intervention of RA.
To cite this abstract in AMA style:
Tong Y, Bai Y, Zhao Y, Liu Y, Luo Y. Intestinal Microbiota Dynamics in the Progression of Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/intestinal-microbiota-dynamics-in-the-progression-of-rheumatoid-arthritis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/intestinal-microbiota-dynamics-in-the-progression-of-rheumatoid-arthritis/