Session Information
Date: Monday, November 9, 2020
Title: Pediatric Rheumatology – Clinical Poster III: SLE, Vasculitis, & JDM
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: Many children with rheumatic disease have active disease as adults, and health care gaps often occur in the transition from pediatric to adult care. We evaluated health care utilization during the adult to pediatric transition.
Methods: This IRB-approved, retrospective study evaluated individuals with rheumatic disease transferring from a pediatric to an adult health system (1/1/2006 -12/31/2016). Subjects age ≥ 8 yrs by 1/1/2010 with ≥ 1 visit before age 20 y, ≥ 2 visits with same rheumatology-related ICD-9 and 10 diagnostic codes (RDC), initial visit with RDC in the children’s health system , ≥1 visit with RDC in adult system, and ≥ 1 rheumatology specialty provider visit were included. Pre-transition period was defined as time between first and last rheumatology visits in the children’s health system. Transition period was time from last pediatric rheumatology visit to second adult rheumatology visit, and post-transition period was time between second and last adult rheumatology visits. Gender, self-reported race/ethnicity, medication (disease modifying anti-rheumatic drugs or biologic) use, diagnosis and household income [estimated by post-transition zip code using US Census Bureau American Community Survey (2014-2018)] were analyzed. Mixed effects binomial modeling of the dichotomous variable of ≥ 1 emergency department (ED) visit or hospitalization was performed examining variables denoted in Table 1. Poisson modeling of the continuous outcomes of number of rheumatology and non-rheumatology office visits was performed including predictors in Table 1 except period duration.
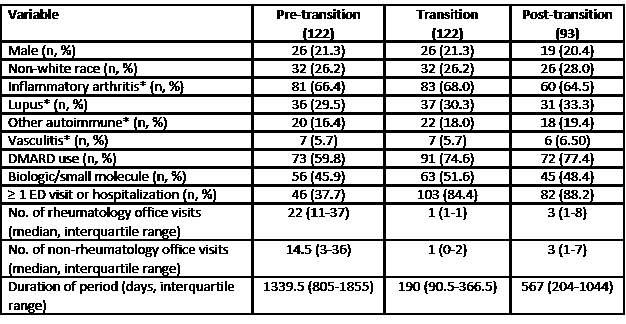
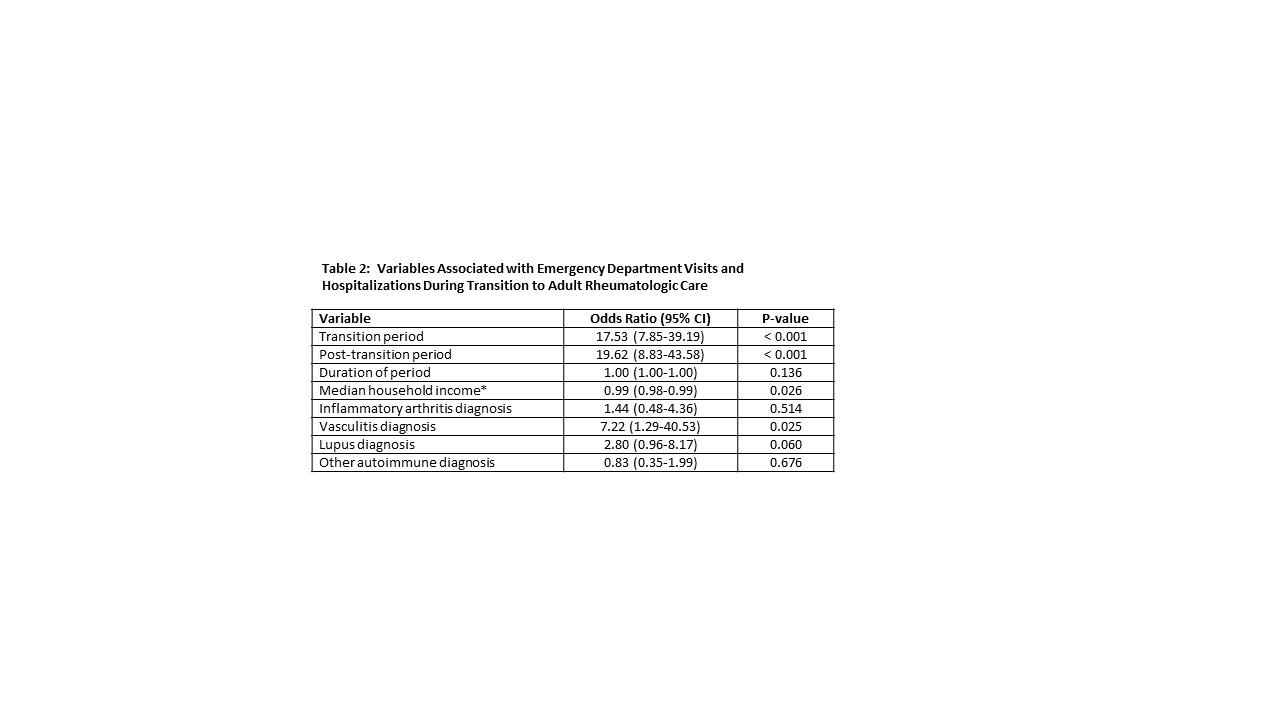
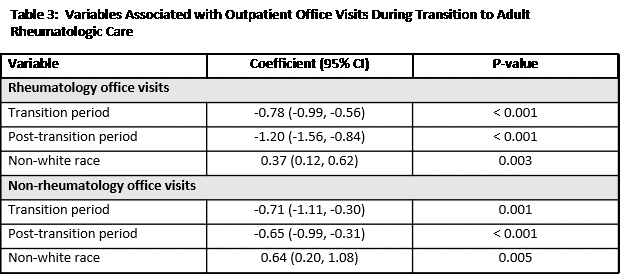
Results: 122 subjects met inclusion criteria for analysis. Of these, 93 (76%) reached post-transition period; 96 (79%) were female and were 32 (26%) non-white. Median household income was $67,872 (IQR $46,013 – $81,813). Patient characteristics during the transition periods are summarized in Table 1. Median transition time was 190 days (IQR 90.5 – 366.5). As noted in Table 2, risk of ≥ 1 ED visit or hospitalization significantly increased during transition period (OR 17.5; 95% CI 7.8 – 39.2), post-transition period (OR 19.6; 95% CI 8.8 – 43.6) and with diagnosis of vasculitis (OR 7.2; 95% CI 1.3 – 40.5). As shown in Table 3, the number of rheumatology and non-rheumatology office visits, corrected for period duration and other co-variates, decreased during transition and post-transition periods and was lower in non-white subjects.
Conclusion: In this retrospective analysis of health care transition over a 10 yr period between large pediatric and adult medical facilities, the rate of transition to adult care was 76%, higher than in most reported studies, and the median time between last pediatric and second adult rheumatology visits was ≥ 6 months. ED use and hospitalization significantly increased in the transition and post-transition periods and in individuals with vasculitis. Both rheumatology and non-rheumatology office visits decreased in the transition and post-transition periods. Non-white individuals had fewer office visits. These results suggest that efforts to increase post-transition outpatient care have the potential to reduce ED visits and hospitalizations.
To cite this abstract in AMA style:
Jensen P, Greco J, Jackson K, Ardoin S. Increase in Emergency Department Visits and Hospitalizations, Decrease in Outpatient Visits Following Transition to Adult Rheumatologic Care [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/increase-in-emergency-department-visits-and-hospitalizations-decrease-in-outpatient-visits-following-transition-to-adult-rheumatologic-care/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/increase-in-emergency-department-visits-and-hospitalizations-decrease-in-outpatient-visits-following-transition-to-adult-rheumatologic-care/