Session Information
Date: Sunday, November 10, 2019
Title: 3S108: RA – Diagnosis, Manifestations, & Outcomes II: Cardiovascular Comorbidities (921–926)
Session Type: ACR Abstract Session
Session Time: 4:30PM-6:00PM
Background/Purpose: Inflammation has been thought to be a risk factor for cognitive impairment and dementia. RA, an autoimmune inflammatory disorder is associated with a high risk of cardiovascular disease (CVD) as a result of underlying inflammation, However, it is unknown if RA patients at risk of CVD are similarly at higher risk of developing dementia. The objective of this study was to describe the incidence of dementia among patients with RA older than 40 years, and to compare the risk of incident dementia between those with known CVD and those without CVD, with and without traditional CVD risk factors.
Methods: We conducted a longitudinal analysis, using Centers for Medicare and Medicaid claims (CMS) data from 2006-2014. To be included, patients had to be continuously enrolled throughout 2006 (12 months calendar year of fee for service), > 40 years old, eligible for Medicare parts A, B and D, and without a diagnosis of dementia in 2006. RA was defined as: two RA diagnoses (ICD-9-CM 714.xx) by a rheumatologist > 7 and < 365 days apart and or at least one diagnosis of RA and least 1 prescription for a DMARD. Incident dementia was defined as: 2 outpatient claims for dementia (ICD-9-CM codes for 290.xx, 294.1x, or 331.xx) at least 40 days apart in 2007 or later. Prevalent CVD was defined by ICD-9-CM codes for myocardial infarction, heart failure, stroke, or CVD procedures (coronary artery bypass grafting, percutaneous coronary intervention, or carotid endarterectomy) in 2006. CVD risk factors were defined by ICD-9-CM codes for diabetes, hyperlipidemia, hypertension, and obesity in 2006. Age-adjusted incidence rates (IR) were estimated using Poisson models. Age- and sex-adjusted Cox proportional hazard models (HR) were used to compare risk of incident dementia in 3 groups of RA patients; 1) with prevalent CVD 2) without CVD but with CVD risk factors, and 3) no prevalent CVD events nor CVD risk factors.
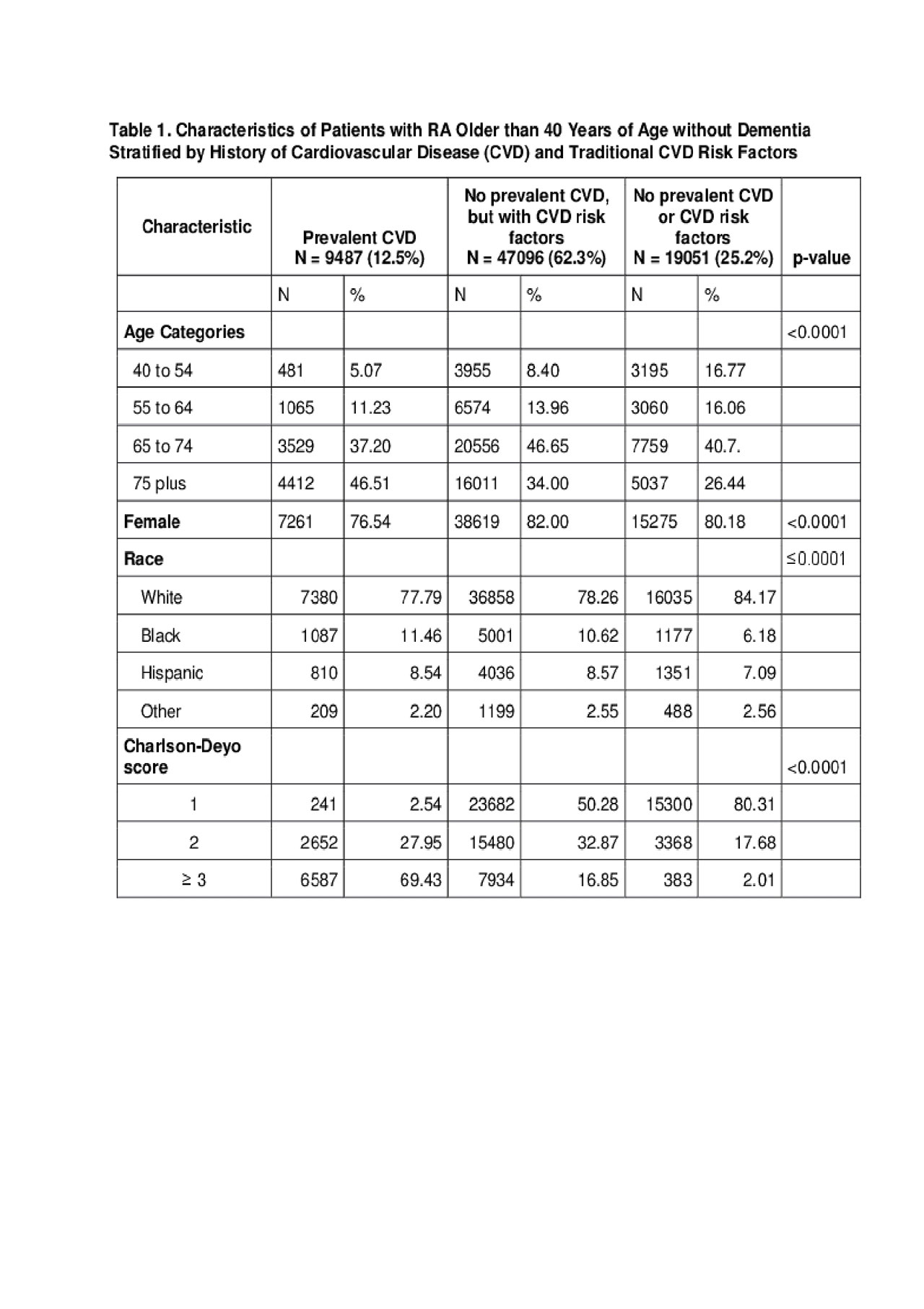
Results: There were 79,957 RA patients in the study sample; 80.8% were female, and 79.6% were white (Table 1). The prevalence of dementia was 2.36% (n = 1,887). After removing RA patients with prevalent dementia in 2006, 75,634 remained. Between 2007-2014, there were 9,835 (13%) cases of incident dementia (Table 1). The age-adjusted IR of dementia was 25.6 (95% CI 24.3 – 26.9) per 1000 person-years for those with prevalent CVD, 17.5 (95% CI 17.1 – 18.1) per 1000 person-years for those with CVD risk factors, and 15.2 (95% CI 14.59-16.00) in patients with neither (Table 2). The age- and sex-adjusted HR for incident dementia was 2.1 (95% CI 1.9 – 2.2) in those with prevalent CVD and 1.2 (95% CI 1.1 – 1.2) in those without prevalent CVD with presence of any CVD risk factor compared to those without CVD and or CVD risk factors.
Conclusion: The incidence of dementia in patients with RA was as high or higher than previous reports from the general population. The presence of CVD in patients with RA increases the risk for incident dementia 2-fold when compared to patients with RA without CVD or CVD risk factors. Our study suggests that in patients with RA, increasing risk for CVD may also be associated with an increased risk for dementia. Further studies comparing patients with and without RA are needed to clarify this association.
To cite this abstract in AMA style:
Sattui S, Rajan M, Lieber S, Lui G, Curtis J, Mandl L, Navarro-Millan I. Incidence of Dementia and Association with Cardiovascular Disease and Risk Factors in Rheumatoid Arthritis – Analysis of a National Claims Database [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/incidence-of-dementia-and-association-with-cardiovascular-disease-and-risk-factors-in-rheumatoid-arthritis-analysis-of-a-national-claims-database/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/incidence-of-dementia-and-association-with-cardiovascular-disease-and-risk-factors-in-rheumatoid-arthritis-analysis-of-a-national-claims-database/