Session Information
Session Type: Poster Session D
Session Time: 9:00AM-11:00AM
Background/Purpose: It is not known whether cancer patients being treated with immune checkpoint inhibitors (ICI) and/or immunosuppression are more vulnerable to SARS-CoV-2 or more apt to have severe manifestations of the disease. We aimed to describe oncology and rheumatology treatment practices in ICI-treated patients with a history of rheumatic immune-related adverse events (irAE) during the March-April 2020 “surge” in SARS-CoV-2 infections in the New York Tri-State area, and to determine the frequency of SARS-CoV-2 infection in these patients.
Methods: A 23-question email survey was administered via RedCap on April, 16 2020 to all living patients enrolled in our institutional ICI rheumatic irAE registry, who had consented to future studies. Participants who did not fill out the form electronically were contacted via telephone and if they agreed, completed the survey verbally. The survey included questions about current cancer status, ICI and immunosuppressant medication use, irAE status, history of SARS-CoV-2 symptoms or diagnosed infection, as well as a free text question asking, “Is there anything else you would like to tell us about how coronavirus has affected you personally?”
Results: The survey was sent to 92 registry patients. Thirty-nine completed the survey electronically and 26 by telephone (response rate 71%). After excluding 2 patients who never received ICI, 63 patients were analyzed (Table 1). Patients who had been on ICI within the last 6 months (n=25) and those who discontinued ICI because of the pandemic (n=7) were identified as patient subsets. There were no significant differences between the groups, although there was a trend toward ICI therapy more often being held in female patients, those on ICI monotherapy and those with a good cancer response. None of the patients who had their ICI held had active arthritis or other irAE requiring immunosuppression. In patients on immunosuppression for irAE, none had changes made in these medications pre-emptively as a result of the pandemic. Table 2 highlights characteristics of patients with proven or presumed SARS-CoV-2 infection. Four of 5 were men, and 3 had renal cell carcinoma (RCC), proportionally higher than the overall cohort both for gender and cancer type. The 2 patients still on active ICI were on combination therapy and prednisone at the time of infection. The other 3 were no longer on either ICI or immunosuppression. 37/63 (59%) responded to the free-text question and, of those, 30 (81%) expressed depression, anxiety/fear, frustration and economic hardship while 7 (19 %) remained optimistic and positive (Table 3).
Conclusion: Oncologists held ICI in a quarter of registry cancer patients in the context of the SARS-CoV-2 pandemic, particularly women on ICI monotherapy who had had a good cancer response. Five patients (8%) developed SARS-CoV-2 infection during the NY Tri-state “surge” of March-April 2020, but all were able to recover uneventfully despite their advanced age. Four of 5 with SARS-CoV-2 infection were male, 3 had RCC and 2 were on combination ICI. Larger studies are needed to determine whether RCC and/or combination ICI are risk factors for SARS-CoV-2 infection.
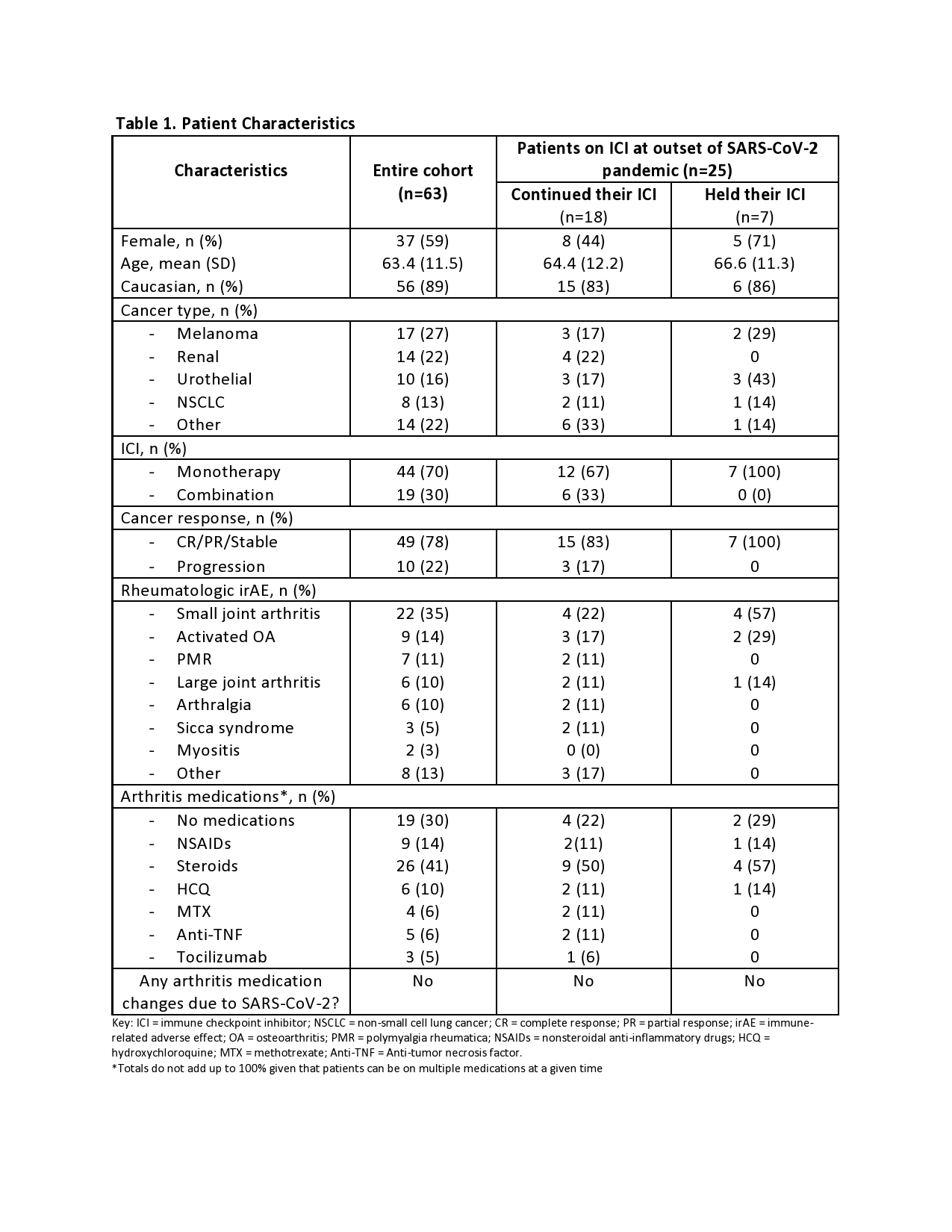 Table 1. Patient Characteristics
Table 1. Patient Characteristics
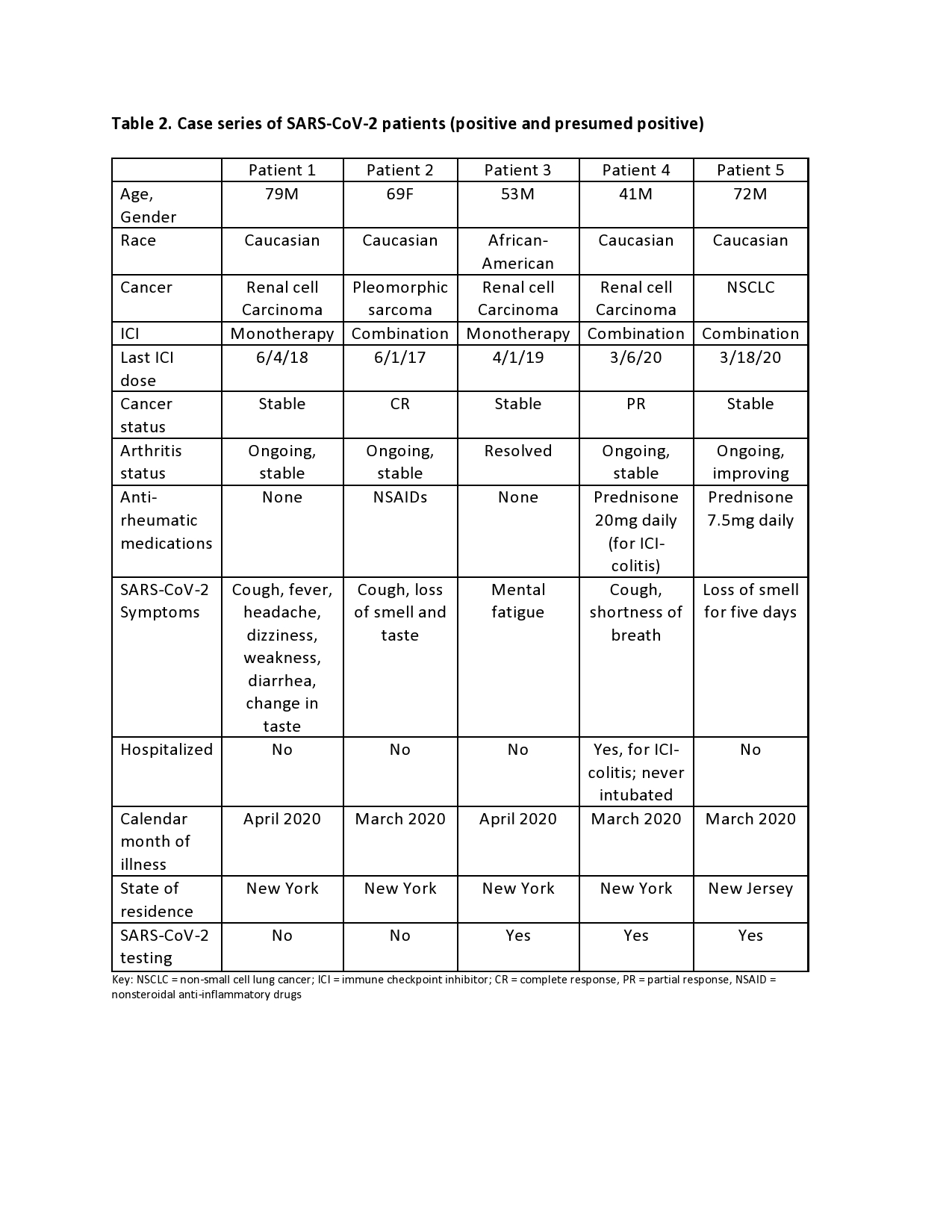 Table 2. Case series of SARS-CoV-2 patients
Table 2. Case series of SARS-CoV-2 patients
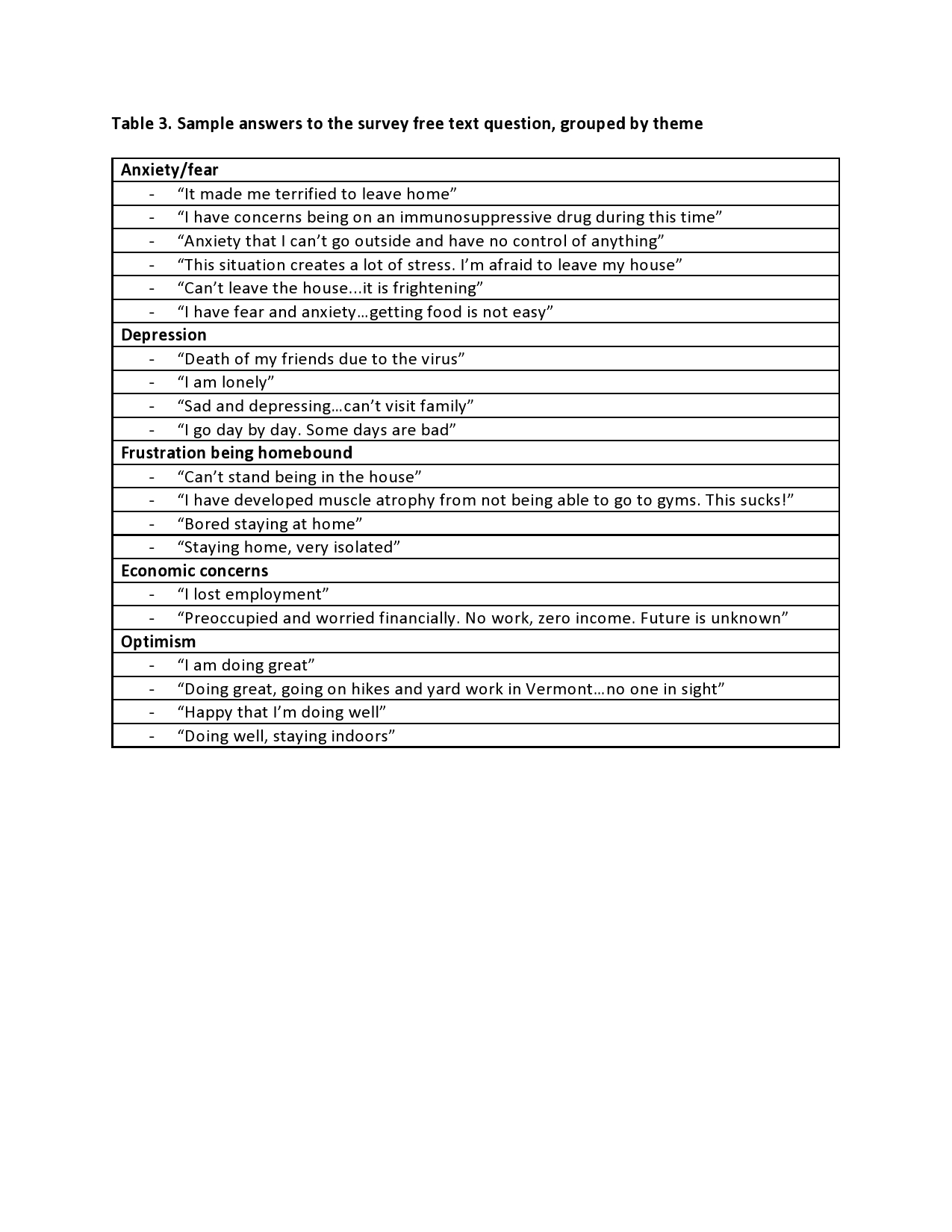 Sample answers to free text question regarding SARS-CoV-2 pandemic, grouped by theme
Sample answers to free text question regarding SARS-CoV-2 pandemic, grouped by theme
To cite this abstract in AMA style:
Ghosh N, Tirpack A, Benson C, Vitone G, Chan K, Bass A. Impact of the SARS-CoV-2 Pandemic on a Cohort of Patients with Rheumatic Complications of Immune Checkpoint Inhibitors: A Registry Survey Study [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/impact-of-the-sars-cov-2-pandemic-on-a-cohort-of-patients-with-rheumatic-complications-of-immune-checkpoint-inhibitors-a-registry-survey-study/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/impact-of-the-sars-cov-2-pandemic-on-a-cohort-of-patients-with-rheumatic-complications-of-immune-checkpoint-inhibitors-a-registry-survey-study/
