Session Information
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Clinical evaluation of synovitis in rheumatoid arthritis (RA) is difficult in obese (O) and overweight patients, due to the fat pad located around the joint, that can over- or under estimate the number of joints regarded as swollen by clinical examination.
Objectives: To compare the level of agreement between the number of joints considered abnormal by Power Doppler ultrasound (PDUS) and clinical examination (swollen joint count (SJC) as component of SDAI) in O (i.e. Body Mass Index (BMI) >30) versus non-obese (NO) (BMI≤30) RA patients.
Methods: RA patients ≥18 years fulfilling 2010 ACR-EULAR criteria, treated with conventional synthetic (cs) or biologic (b) DMARDs were included in the cross-sectional multicenter (13 centers) French observational RABODI study (ClinicalTrials.gov Identifier: NCT03004651). Clinical synovitis was evaluated on 44 joints. ESR and CRP were collected and several composite scores were calculated: SDAI, DAS28, DAS. A standard US examination on 44 joints for the presence of synovial hypertrophy (SH) and PD signal according to the EULAR-OMERACT scoring system was performed in each center by an independent investigator blinded to clinical data. Presence of US synovitis was defined by a SH≥1 and PD signal≥1 on a semi-quantitative scale. Levels of agreement between number of synovitis defined by PDUS and clinical examination were compared in O versus NO patients using Chi2 test, and Kappas (k) and ORs were calculated. A patient was considered “discordant” if ≥1 joint was discordantly classified by PDUS and clinical examination. SDAI was calculated and compared, with SJC defined either by clinical examination or PDUS.
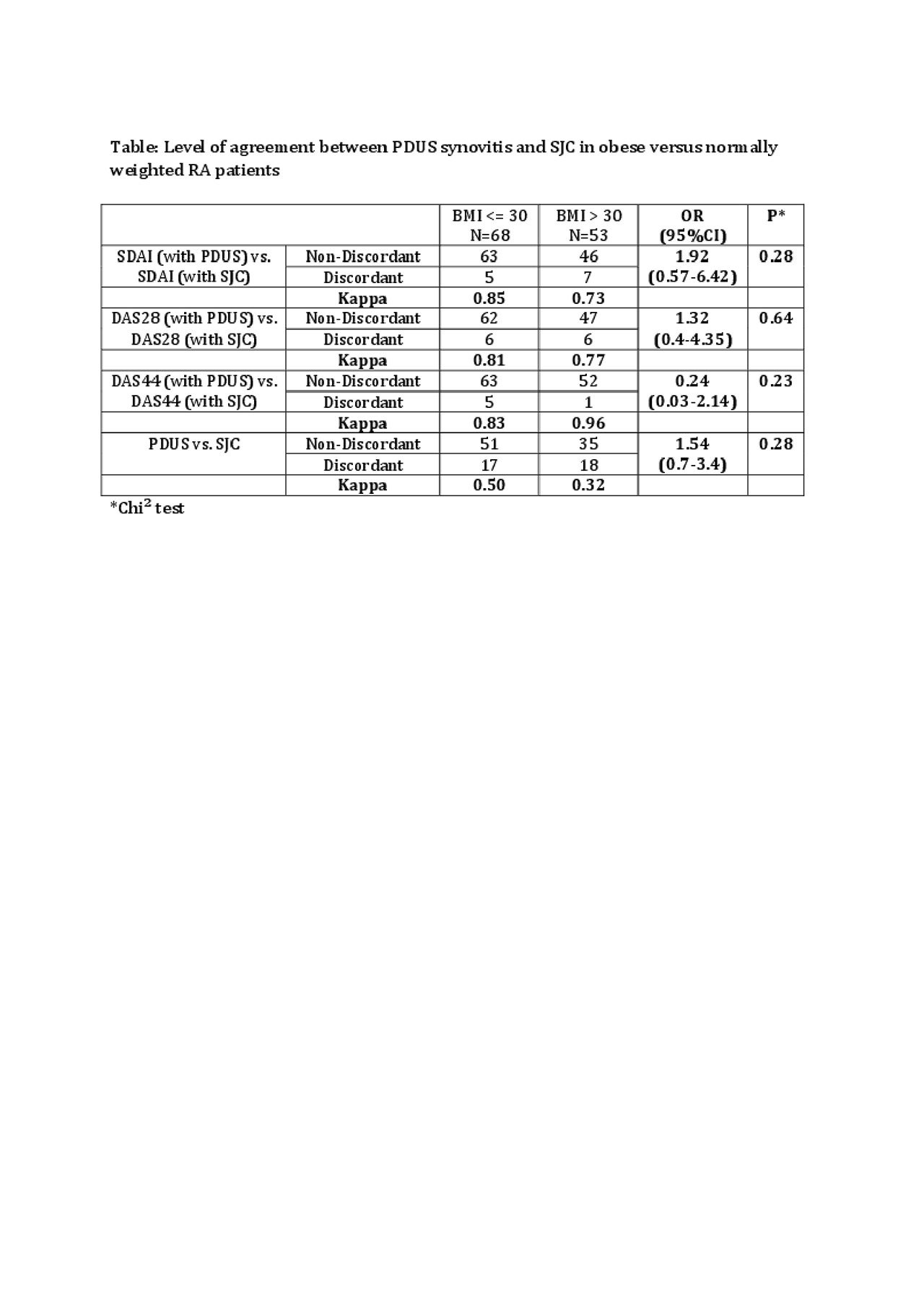
Results: 121 patients were included: mean (SD) age of 58.5 (12.7) years, mean disease duration of 11.1 (9.7) years. 81% were female, 84.3% anti-CCP positive, 63.6% had erosive disease. Mean SDAI was 12,6 (±10,2). 53 (43.8%) had a BMI >30 and 68 (56.2%) ≤30. 59 (48.7%) and 62 (51.2%) had a SDAI≤11 and >11, respectively. 78.5% received csDMARD, 58.7% bDMARD and 40.5% glucocorticoids. The 2 groups were comparable, except for weight (mean (SD) 65.4 (13.5) vs 96.7 (14.7) kg, p< 0.001), some comorbidities (diabetes, asthma and fibromyalgia more frequent in O patients, anemia less frequent), tender joint count (mean 4.04 (±5.23) in NO vs 7.38 (±8.64) in O, p=0.021). Mean number of clinical synovitis was 2.4 (3.3), and 6.7 (±6.3) by PDUS. Levels of agreement between clinical and PDUS findings were comparable in O vs. NO patients regarding SDAI and other scores (Table). Patients with ≥3 discordant joints was numerically higher in O patients compared to NO (26/53 (49.1%) vs 22/68 (32.4%), p=0.062). Results were similar when overweighted patients (BMI >25) were compared with normally weighted patients (BMI≤25) or when SH≥1 was considered in place of PDUS synovitis. At the joint level, discordance was higher in O patients in some specific joints: MCP4 (p=0.057), wrist (p=0.089).
Conclusion: In RA patients, despite a perceived higher difficulty to clinically detect synovitis (SJ) in O patients, the discrepancy between clinically- and PDUS defined synovitis was not significantly higher than in NO patients, and did not impact the extend of the definition of disease activity level.
To cite this abstract in AMA style:
Mouterde G, Manna F, Le Goff B, Albert J, Jousse-Joulin S, Gandjbakhch F, Loeuille D, Gaudin P, Piperno M, Banal F, Jamard B, Salliot C, Molinari N, Combe B, D'Agostino M, Lukas C. Impact of Body Mass Index on the Agreement Between Ultrasound- and Clinical Assessments of Disease Activity in Rheumatoid Arthritis : Multicenter and Cross-sectional Study [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/impact-of-body-mass-index-on-the-agreement-between-ultrasound-and-clinical-assessments-of-disease-activity-in-rheumatoid-arthritis-multicenter-and-cross-sectional-study/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/impact-of-body-mass-index-on-the-agreement-between-ultrasound-and-clinical-assessments-of-disease-activity-in-rheumatoid-arthritis-multicenter-and-cross-sectional-study/