Session Information
Date: Saturday, November 6, 2021
Title: Fibromyalgia & Other Clinical Pain Syndromes Poster (0118–0127)
Session Type: Poster Session A
Session Time: 8:30AM-10:30AM
Background/Purpose: Over one-third of patients with rheumatoid arthritis (RA) exhibit evidence of fibromyalgianess, a cluster of somatic symptoms associated with increased sensitivity to painful stimuli. Fibromyalgianess is associated with higher rates of disability among RA patients and inadequate responsiveness to disease-modifying antirheumatic drugs (DMARDs). Up to half of patients with RA often remain on oral glucocorticoids (GCs) for prolonged periods, despite the well-described risk of dose-dependent morbidity and mortality. We know little about how fibromyalgianess might influence GC use in RA. In this study, we examined the longitudinal association between fibromyalgianess and oral GC persistence among RA patients.
Methods: We used data from the Central Pain in Rheumatoid Arthritis (CPIRA) cohort to follow participants with active RA on oral prednisone after they initiated a new DMARD. Fibromyalgianess was measured using the Fibromyalgia Survey Questionnaire (FSQ), previously shown to correlate with key fibromyalgia features often superimposed upon RA. Severity of fibromyalgianess was stratified as follows: FSQ< 8 low, 8-10 moderate, and >10 high/very high. GC persistence was defined as GC use at three-month follow-up visit. The association between baseline fibromyalgianess (exposure) and GC persistence at 3-month follow-up (outcome) was assessed using multiple logistic regression. The analysis was adjusted for baseline demographics, RA duration, serologic status, and inflammatory activity as measured by swollen joint count and C-reactive protein.
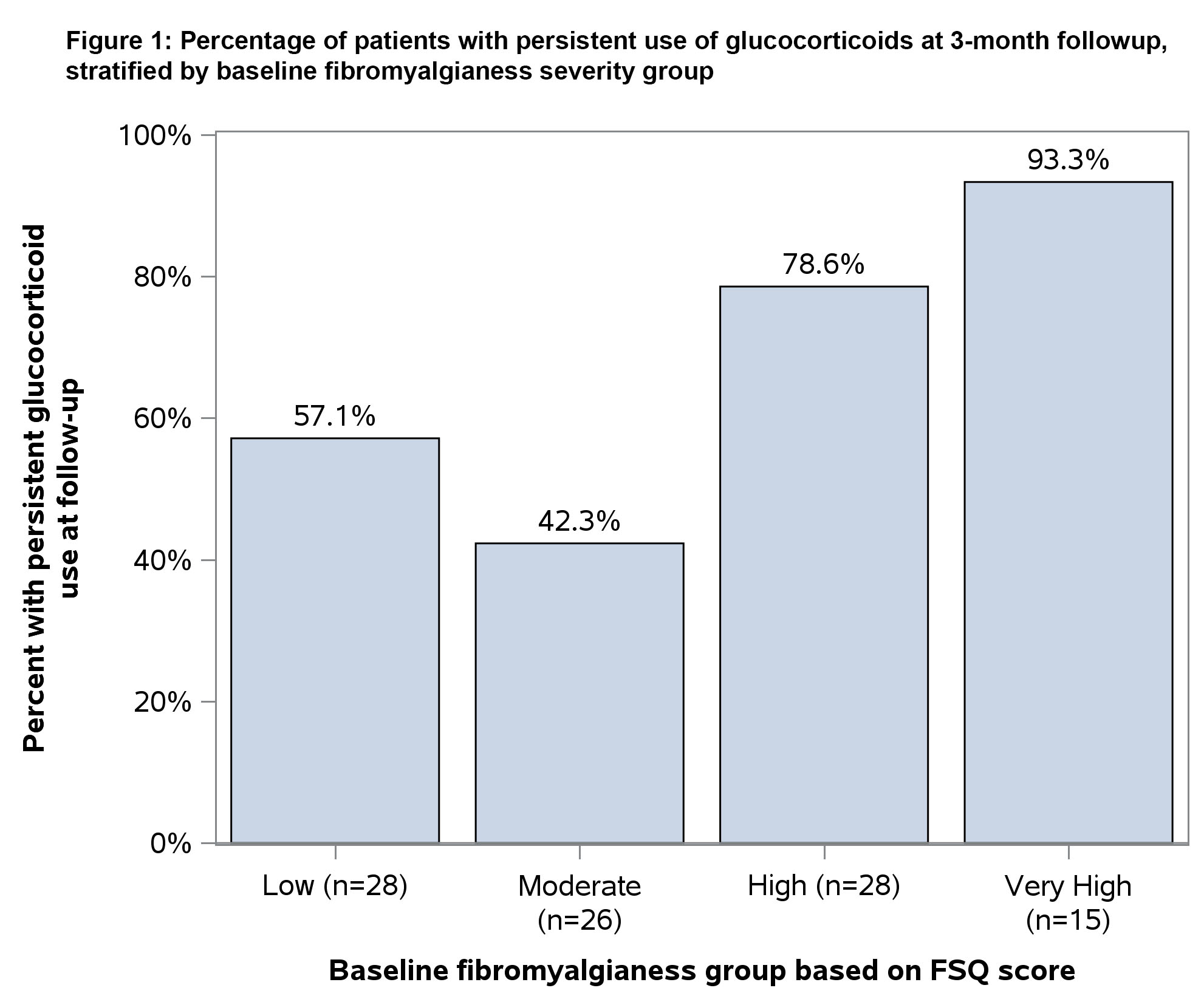
Results: Of 97 participants on prednisone at baseline, 65% were taking prednisone at follow-up. Fifty-seven percent of participants with low baseline fibromyalgianess had persistent GC use, compared to 84% with high or very high fibromyalgianess. After adjustment as outlined above, participants with high/very high baseline fibromyalgianess remained more likely to be on prednisone at follow-up, relative to those with low fibromyalgianess (OR 4.99 [95% CI 1.20 – 20.73]).
Conclusion: In this cohort of patients with active RA, high fibromyalgianess is associated with persistent GC use, independent of inflammatory activity. This finding suggests that non-inflammatory pain related to fibromyalgianess may be misclassified by patients or providers as inflammatory pain related to RA disease activity. Greater insights into clinician and patient perspectives on GC tapering in RA patients with high fibromyalgianess are required to help clinicians distinguish active RA symptoms from manifestations of other chronic pain conditions.
To cite this abstract in AMA style:
Wallace B, Moore M, Heisler A, Muhammad L, Song J, Clauw D, Bingham C, Bolster M, Marder W, Neogi T, Wohlfahrt A, Dunlop D, Lee Y. Fibromyalgianess and Glucocorticoid Persistence Among Patients with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/fibromyalgianess-and-glucocorticoid-persistence-among-patients-with-rheumatoid-arthritis/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/fibromyalgianess-and-glucocorticoid-persistence-among-patients-with-rheumatoid-arthritis/