Session Information
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Giant cell arteritis (GCA) is the most common systemic vasculitis in the elderly. The halo sign is an accepted valid test for the diagnosis of GCA in trained units. However, other conditions can also produce a hypoechoic increase of the arterial wall thickness and mimic the halo sign. Our aim was to describe the frequency and causes of false positives in the diagnosis of GCA by color Doppler ultrasound (CDUS).
Methods: We performed an observational retrospective study of 305 patients with temporal artery CDUS findings compatible with GCA. Their medical records were reviewed to collect demographic, physical examination, clinical and analytical data. The medical diagnosis based on the clinical evolution of the patient during at least 1 year of follow-up was established as the gold standard for definitive diagnosis.
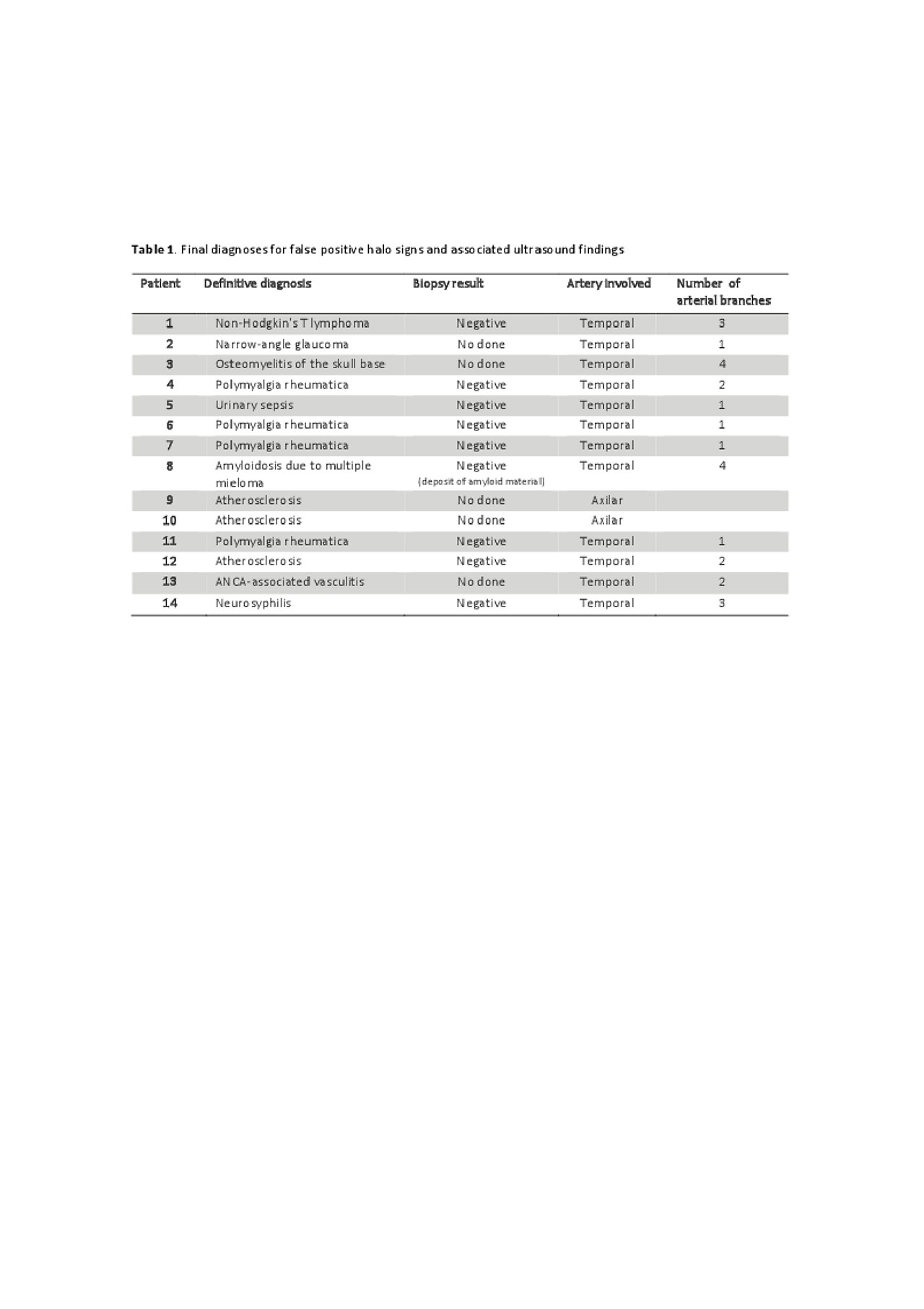
Results: 14 of the 305 included cases (4.6%) were false positives. The characteristics of these 14 patients and their final diagnoses are shown in table 1. 64% were female. The median age was 72 (interquartile range 68-79) years. The median erythrocyte sedimentation rate was 55 (32-110) mm/h, C-reactive protein 15.1 (7.3-100.9) mg/L and hemoglobin 13.3 (11.2-14.1) g/dL. Five patients (36%) fulfilled the 1990 American College of Rheumatology classification criteria. A temporal artery biopsy was performed in 9 patients (64%), with negative results in all of them. Twelve patients (86%) had CDUS involvement of the superficial temporal arteries. Five had 1 branch involved (42%), three 2 branches (25%), two 3 branches (17%) and two 4 branches (17%). In addition, two patients (14%) had an isolated halo sign in the axillary arteries, one unilateral and the other bilateral. Regarding the definitive diagnosis, in four patients it was polymyalgia rheumatica (29%), in three atherosclerosis (21%), and there was one case each of non-Hodgkin’s Lymphoma type T, osteomyelitis of the skull base, primary amyloidosis associated with multiple myeloma, granulomatosis with polyangiitis, neurosyphilis, urinary sepsis and narrow-angle glaucoma.
Conclusion: CDUS diagnosis of GCA yields a low percentage of false positives. These are attributable either to operator-dependent technical mistakes or to the presence of other medical conditions that alter the US signal of the arterial wall, resulting in a halo sign. The clinician must be aware of the existence of these conditions when interpreting this test, in order to improve the diagnostic accuracy of the CDUS.
To cite this abstract in AMA style:
Fernández E, Monjo I, Bonilla G, Plasencia C, Miranda-Carus M, Balsa A, de Miguel E. False Positives in the Ultrasound Diagnosis of Giant Cell Arteritis: Some Diseases Can Also Have Halo Sign [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/false-positives-in-the-ultrasound-diagnosis-of-giant-cell-arteritis-some-diseases-can-also-have-halo-sign/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/false-positives-in-the-ultrasound-diagnosis-of-giant-cell-arteritis-some-diseases-can-also-have-halo-sign/