Session Information
Date: Tuesday, October 23, 2018
Title: Muscle Biology, Myositis and Myopathies Poster III: Treatment and Classification Criteria
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: We examined patients in a large juvenile dermatomyositis (JDM) registry for frequency of and factors associated with final corticosteroid discontinuation (Steroid DC), complete clinical response (CCR, clinically inactive disease for ≥6 continuous months on treatment), and remission (inactive disease for ≥6 continuous months off all treatment).
Methods: A retrospective review of illness outcomes was evaluated in 307 patients with probable or definite JDM with median follow-up duration of 43 months. The probability of achieving steroid DC, CCR, and remission were examined by Weibull time-to-event modeling. Significant univariable predictors were examined in multivariable time-to-event analysis using Markov chain Monte Carlo extension models. The conditional probability of each outcome was also evaluated using Bayesian network models.
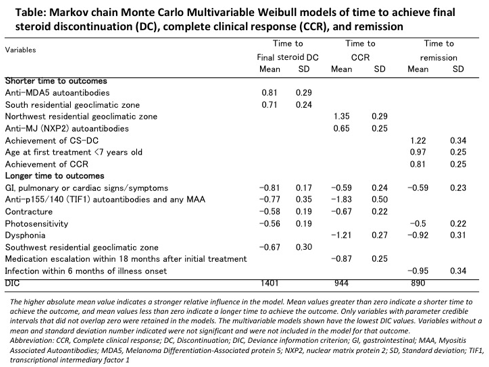
Results: One-hundred-ninety-one of the 307 patients (62.2%) achieved at least one of the outcomes. By 60 months from treatment initiation, 57% of patients achieved steroid DC, 44% achieved CCR, and 31% achieved remission. Time to 50% probability of achieving steroid DC, CCR, and remission were 52, 69, and 92 months, respectively. The probability of CCR and remission were conditional. The probability of attaining CCR given steroid DC was 47%; when steroid DC was not attained, the probability of achieving CCR was 19%. When steroid DC and CCR were achieved, the probability of achieving remission was 66%. When steroid DC and CCR were not achieved, the probability of remission was 3.5%. Several factors were associated with longer times to achieve these outcomes in multivariable models. Gastrointestinal, pulmonary or cardiac symptoms were the only factors associated with longer times to achieve all three outcomes. Anti-p155/140 autoantibodies (Abs) with any myositis associated Abs and contractures were associated with longer times to steroid DC and CCR, photosensitivity with longer times to steroid DC and remission, and dysphonia with longer times to CCR and remission. A Southeast residential geoclimatic zone, medication escalation within 18 months of treatment initiation, and an infection within 6 months of illness onset were associated with longer times to achieve a single outcome. Anti-MDA5 Abs and a Southern residential geoclimatic zone were associated with shorter times to steroid DC. A Northwest residential geoclimatic zone and anti-MJ Abs were associated with shorter times to CCR. The achievement of steroid DC and CCR and younger age at first treatment were associated with shorter times to remission.
Conclusion: A large proportion of JDM patients achieve positive treatment responses, including steroid DC, CCR, and remission, although timelines for these important outcomes are relatively long. Factors associated with times to achieve these outcomes include selected clinical features, autoantibodies, and environmental factors.
To cite this abstract in AMA style:
Kishi T, Warren-Hicks W, Bayat N, Targoff I, Finkel TH, Goldmuntz E, Henrickson M, Lang B, Mammen A, Pachman LM, Passo M, O'Hanlon TP, Miller FW, Ward M, Rider LG. Factors Associated with Corticosteroid Discontinuation, Complete Clinical Response and Remission in Patients with Juvenile Dermatomyositis [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/factors-associated-with-corticosteroid-discontinuation-complete-clinical-response-and-remission-in-patients-with-juvenile-dermatomyositis/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/factors-associated-with-corticosteroid-discontinuation-complete-clinical-response-and-remission-in-patients-with-juvenile-dermatomyositis/