Session Information
Date: Tuesday, November 15, 2016
Title: Spondylarthropathies and Psoriatic Arthritis – Clinical Aspects and Treatment - Poster III
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: The diagnosis and assessment of psoriatic arthritis (PsA) and psoriasis (PsO) lesions are mostly done by visual inspection, and when in doubt, supplemented by a biopsy. Although PsA is primarily assessed by physical examination, the utility of ultrasound is beneficial. Here, we test the performance of advanced ultrasound skin imaging software applications in PsO & PsA assessment.
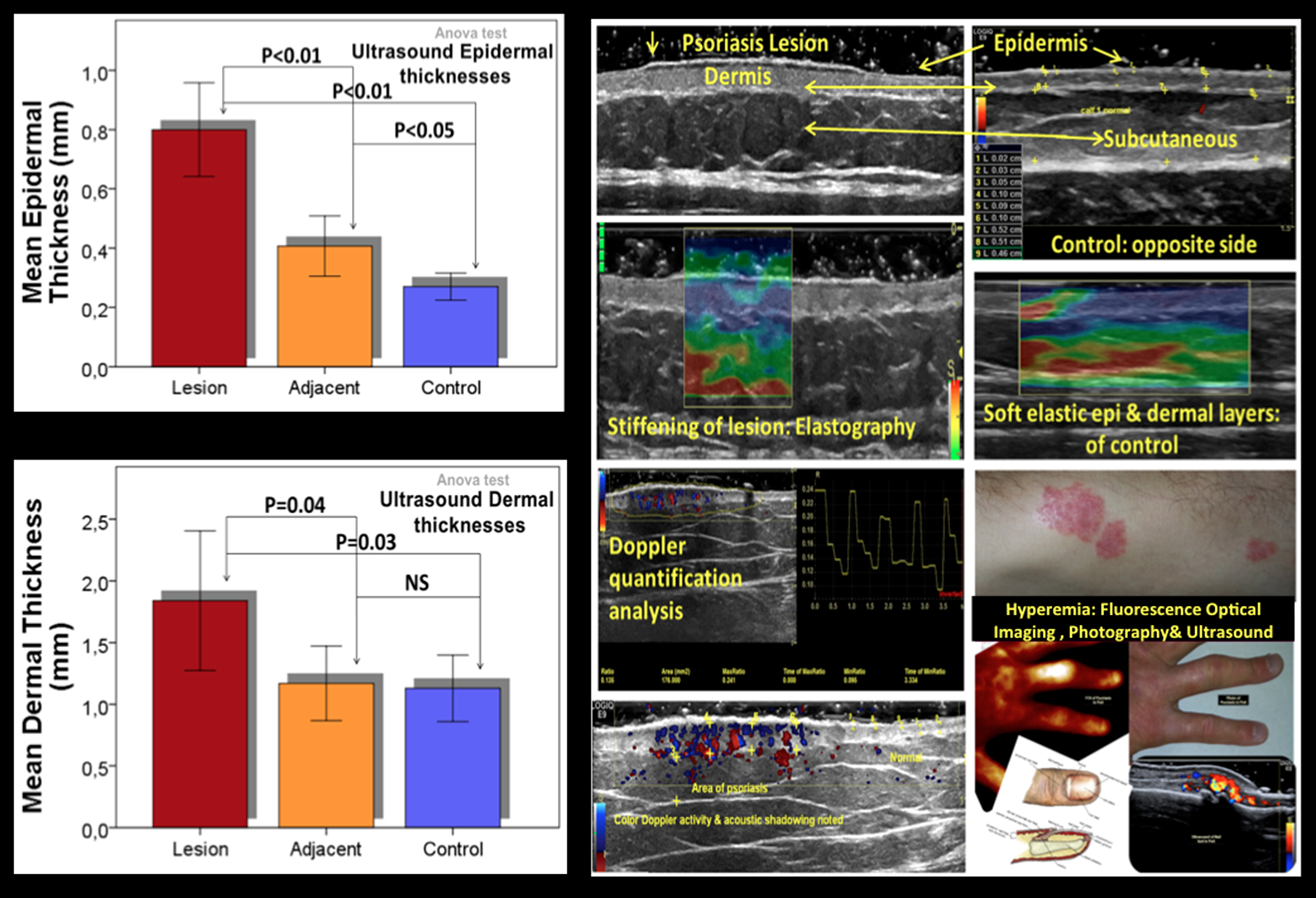
Methods: The rheumatologist and dermatologist performed standard clinical examinations on PsA and PsO patients respectively. Using ultrasound (US), we evaluated the hand, wrist, & symptomatic joints of PsA patients for synovitis & tenosynovitis (nail beds included). Blinded by the clinical results & treatment plans, the epidermal, dermal and subcutaneous tissue thickness of 2 of the most affected lesions were scanned by high frequency B-Mode, automated color Doppler quantification (CDQ) and elastography applications (measuring lesion size, depth, hyperemia and tissue elasticity). The skin tissues adjacent to the psoriatic lesion, and the unaffected skin on the contralateral side (self-control) were measured for comparison.
Results: A total of 270 skin measurements in, around, & opposite to the 10 psoriatic lesions of 5 PsA/PsO patients were analyzed. Epidermal thickness differed significantly between adjacent and control tissue layers [F (2,27) = 30.95, MSE = 0.76, p<0.001]. Similar findings were evident for dermal thickness differences [F (2,27) = 5.05, MSE = 1.59, p=0.014]. Subcutaneous tissue depths were of no significance. Ultrasound CDQ & elastography revealed hyperemia in 80% of lesions (60% with plaque). Contrary, 20% of lesions showed no obvious Doppler activity, displaying reduced tissue stiffening on elastography (suggesting healed lesions). Two of 10 lesions were soft on elastography (no acoustic shadows) but had low-level CDQ activity (minimum 0.016:0.034 & maximum 0.103:0.135 ratios). In PsA patients, the presence of synovitis (intra &extra-articular Doppler) mostly in DIPs & PIPs, and tenosynovitis of flexor tendons were detected. Hyperemic nail beds (altered microcirculation) and hand psoriasis skin perfusion was evident on US, and confirmed by fluorescence optical imaging (FOI).
Conclusion: Several ultrasound parameters clearly distinguish between affected & normal skin and could be used as quantitative and objective measures in assessing psoriasis lesions. Some US parameters appear to distinguish between adjacent (non-involved) skin & self-control skin, while some show striking heterogeneity between different patients, suggesting that US may help subtype psoriasis lesions, but need to be investigated further. Ultrasound metrics of skin tissue (depth, plaque characteristics, elasticity and Doppler quantification) has potential to compliment the clinical assessment of PsO & PsA patients.
To cite this abstract in AMA style:
Kisten Y, Larsson PT, af Klint E, Rezaei H, Györi N, Eidsmo L, Ståhle M, van Vollenhoven RF. Evaluating Psoriatic Arthritis and Psoriasis Skin Lesions: Ultrasound As a Complementary Measure [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/evaluating-psoriatic-arthritis-and-psoriasis-skin-lesions-ultrasound-as-a-complementary-measure/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/evaluating-psoriatic-arthritis-and-psoriasis-skin-lesions-ultrasound-as-a-complementary-measure/