Session Information
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: JIA-associated uveitis (JIA-U) is the most prevalent extra-articular manifestation of JIA and the most common type of uveitis in children. To date, environmental factors such as smoke exposure, early life infection, pets, breast feeding, residential areas, stressful life events and prematurity have been investigated for potential associations with the development of JIA. Prematurity was found to have a possible correlation with JIA; while in adults, cigarette smoke has been reported to have an association with the onset of uveitis. Our objective is to identify environmental factors (pregnancy history, smoking exposure and initial feeding regimen) and disease characteristics (clinical lab values, disease duration and disease subtype) associated with uveitis development in children with JIA.
Methods: We reviewed records for a JIA cohort comprised of 171 children (120 oligoarticular or polyarticular RF- JIA without uveitis [JIA-no-U], and 51 JIA-U) enrolled in a prospective study on uveitis outcomes who are seen at an outpatient clinic at Cincinnati Children’s Hospital. Data collected included JIA and uveitis clinical characteristics, and a baseline ESR at JIA diagnosis. Parents or guardians completed a questionnaire on socio-cultural factors including pregnancy history (fertility treatments, substance use and birth weight), initial feeding regimen and smoke exposure (Figure 1). Means were used to compare JIA-no-U and JIA-U patients using Chi Square (χ2) and T-test.
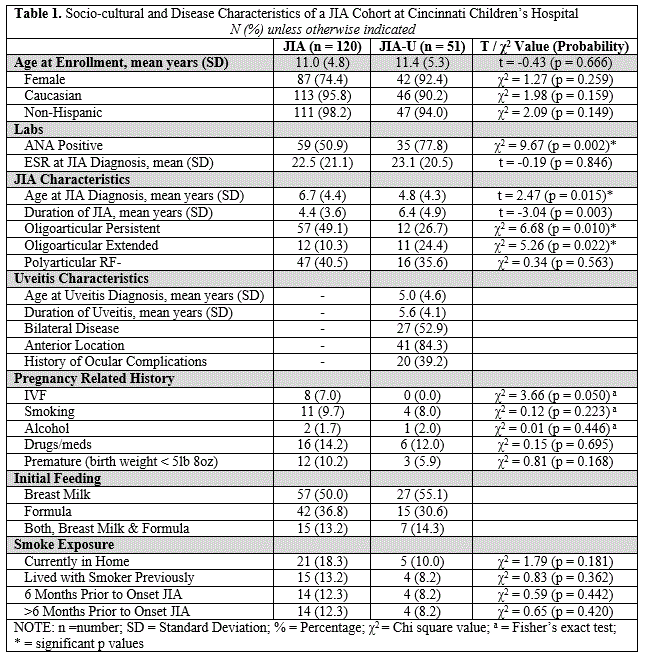
Results: Of 171 children, mean age was 11 (SD, 5 years), 75% female, 93% Caucasian and 93% non-Hispanic (Table 1). Compared to JIA-no-U, those with JIA-U were more likely to be ANA positive (50.9% vs. 77.8%, p = 0.002), diagnosed with JIA at a younger age (6.7 vs. 4.8 years, p = 0.015), and be of the oligoarticular extended JIA category (24.4%, p = 0.022). ESR (nearest JIA diagnosis) of JIA-no-U and JIA-U children at JIA diagnosis was not significantly different (22.5 vs. 23.1, p = 0.846). Environmental factors such as initial feeding regimens, pregnancy history and smoke exposure were also not significantly different. A portion of our JIA population report a history of in-vitro fertilization (JIA-no-U: 8 vs. JIA-U: 0, p = 0.050).
Conclusion: Our results are consistent with previous findings suggesting children with JIA-U more commonly have a positive ANA and are diagnosed with JIA at a younger age. In our Midwest regional cohort, we were not able to identify environmental factors significantly-associated with uveitis development in children with JIA. Further, we were not able to confirm associations with smoking or baseline ESR levels. Future studies are needed in a larger cohort to examine environmental factors in relation to healthy controls and JIA-U children, and other reported environmental factors such as birth order, delivery type or family medical history.
To cite this abstract in AMA style:
Hennard T, Mwase N, Cassedy A, McDonald J, Utz V, Angeles-Han S. Epidemiology of JIA-Associated Uveitis: Environmental Factors and Disease Characteristics of a JIA-Associated Uveitis Cohort [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/epidemiology-of-jia-associated-uveitis-environmental-factors-and-disease-characteristics-of-a-jia-associated-uveitis-cohort/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/epidemiology-of-jia-associated-uveitis-environmental-factors-and-disease-characteristics-of-a-jia-associated-uveitis-cohort/