Session Information
Date: Tuesday, November 14, 2023
Title: (2257–2325) SLE – Diagnosis, Manifestations, & Outcomes Poster III
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Systemic Lupus Erythematosus (SLE) is associated with epithelial defects and disrupted intestinal barrier, risking bacterial translocation, and promoting systemic inflammation, known as dysbiosis, which is associated with increased disease activity (1). Enterococcus gallinarum has been previously linked to gastrointestinal autoimmune diseases, like autoimmune hepatitis and primary sclerosing cholangitis. (2) However, little is known about E. gallinarum prevalence in SLE. Our objective was to analyze the frequency of E. gallinarum in stool samples from SLE individuals and examine its association with clinical and laboratory characteristics.
Methods: A cross-sectional, descriptive study was conducted at the University Hospital “Dr. José Eleuterio González” in northern Mexico. We included adult patients who met the current criteria for systemic lupus erythematosus (SLE) and had recent (< 3 months) routine paraclinical tests, including acute phase reactants. Patients with other autoimmune diseases, chronic infections, pregnancy, cancer, abdominal surgery, or gastrointestinal bleeding were excluded. Demographic and clinical data, as well as anti-nuclear antibodies and complement levels, were obtained from medical records. No participant had received antibiotics, probiotics, or synbiotics within 3 months prior to the study. DNA was extracted using the DNeasy PowerLyzer PowerSoil DNeasy kit from Qiagen (Hilden, Germany) according to the manufacturer’s specifications. E. gallinarum was detected using endpoint polymerase chain reaction assay in both SLE patients and age- and sex-matched healthy controls.
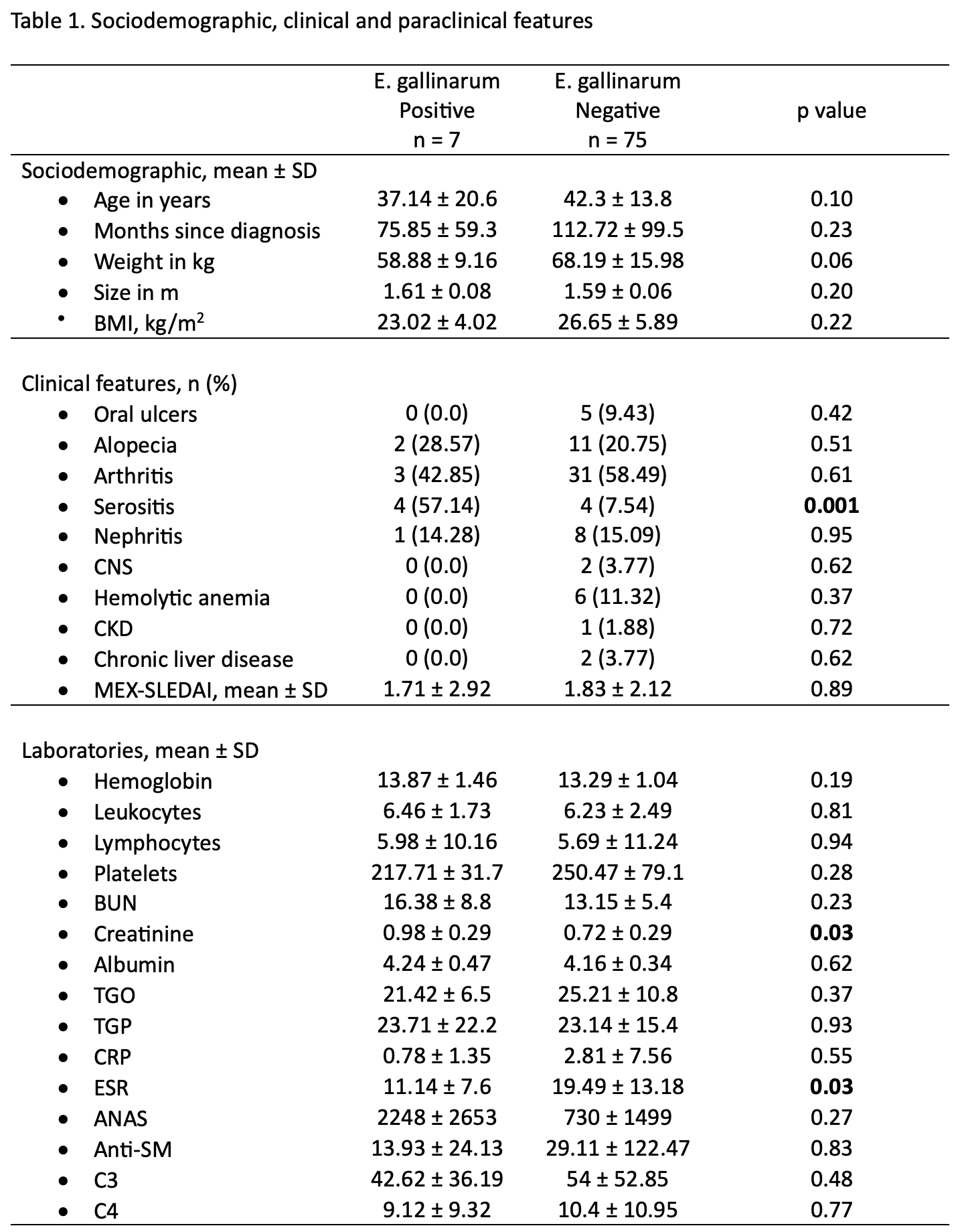
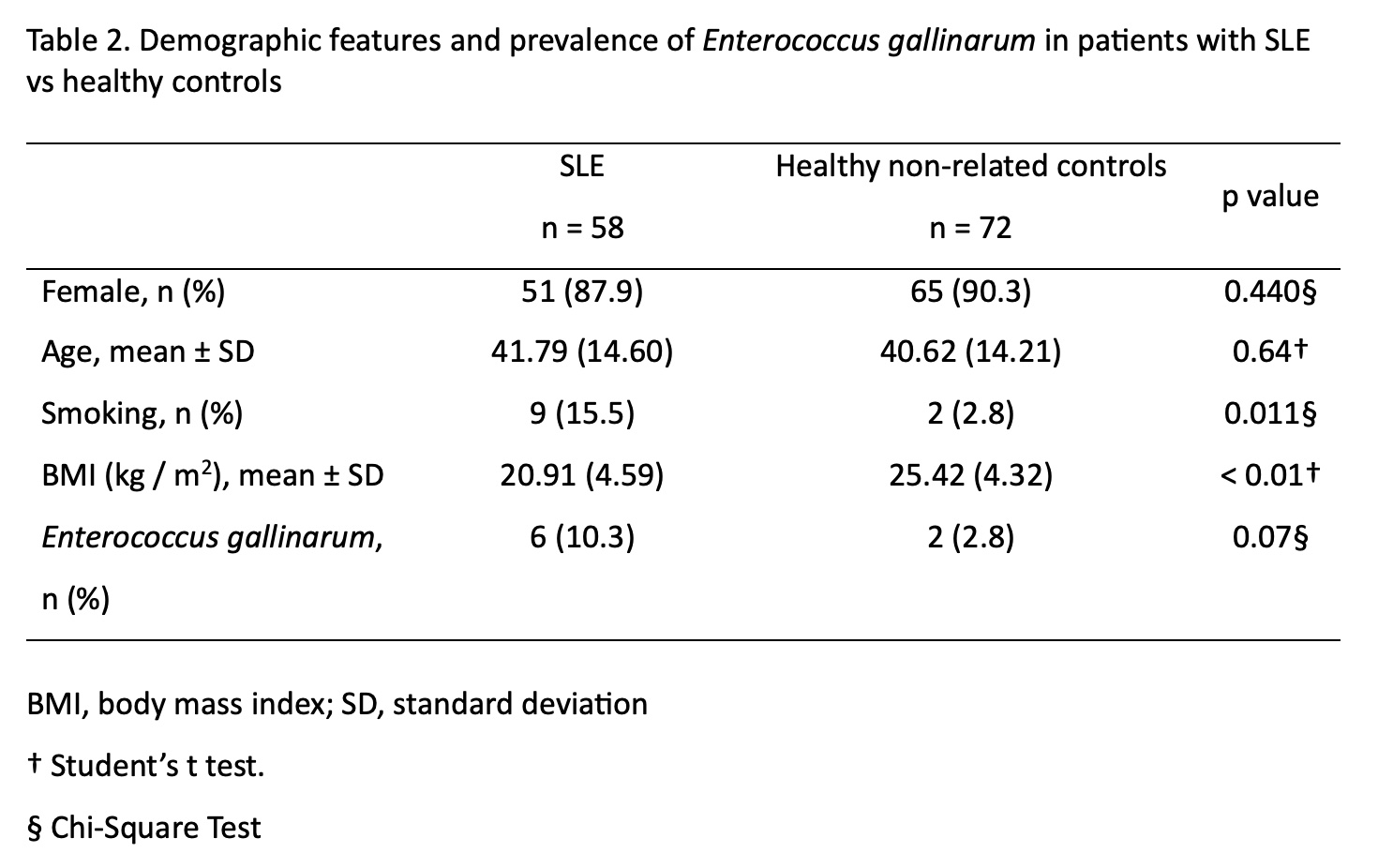
Results: Sixty subjects with systemic lupus erythematosus (SLE) were included in the study, with the majority being women (51, 85%). The mean age was 41.79 (±16.6) years, and the average time since diagnosis was 107.03 months (±95.46). E. gallinarum and Enterococcus spp were detected in 7 (11.6%) cases. The most common MEX-SLEDAI parameter observed was arthritis, present in 34 (56.6%) cases, followed by acute cutaneous lupus in 23 (38.3%) cases. Detailed clinical manifestations and laboratory findings can be found in Table 1. A significant difference was found in E. gallinarum-positive patients regarding creatinine levels (0.98 vs. 0.72, p=0.032), erythrocyte sedimentation rate (11.14 vs. 19.49, p=0.031), and the frequency of serositis (57.14% vs. 7.54%, p=0.001). However, when analyzing erythrocyte sedimentation rate using the age-adjusted upper limit, the significance was no longer present (p=0.4). When comparing the prevalence of E. gallinarum in age and sex matched healthy controls (2.8%) with subjects with systemic lupus erythematosus (SLE) (10.3%), E. gallinarum was found to be slightly higher, approaching statistical significance (Table 2)
Conclusion: E. gallinarum was found to have a slightly higher prevalence in patients with systemic lupus erythematosus (SLE) compared to healthy controls, indicating a potential association with the disease. Significant associations were observed between E. gallinarum-positive SLE patients and certain clinical and laboratory parameters.
To cite this abstract in AMA style:
Vega Sevilla L, Alvarez-González O, Riega-Torres J, Skinner-Taylor C, Rubio Torres D, Vera Cabrera L, Galarza-Delgado D, Cardenas-De la Garza J, Castillo-de la Garza R, Aguilera Valenciano M, Escalante w, Guerra H. Enterococcus Gallinarum Prevalence in Patients with Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2023; 75 (suppl 9). https://acrabstracts.org/abstract/enterococcus-gallinarum-prevalence-in-patients-with-systemic-lupus-erythematosus/. Accessed .« Back to ACR Convergence 2023
ACR Meeting Abstracts - https://acrabstracts.org/abstract/enterococcus-gallinarum-prevalence-in-patients-with-systemic-lupus-erythematosus/