Session Information
Date: Monday, November 11, 2019
Title: 4M115: Pain Mechanisms – Basic & Clinical Science (1878–1883)
Session Type: ACR Abstract Session
Session Time: 4:30PM-6:00PM
Background/Purpose: Despite a broad range of available therapeutics, pain remains poorly treated in many juvenile idiopathic arthritis (JIA) patients1-2. For some patients, the level of pain is not commensurate with the magnitude of detectable joint pathology (i.e., synovitis). In order to elucidate pain mechanisms in JIA, we have investigated the functionality of CNS circuitry in polyarticular JIA (pJIA) individuals ( >5 affected joints) alongside peripheral joint pathology, markers of inflammation, subjective measures related to pain and clinical status. This strategy is projected to facilitate the identification of pain biomarker signatures and define mechanisms that underlie the observed pain-inflammation disconnect in JIA.
Methods: Consented, male and female pJIA patients (8-16 years) with and without pain were assessed using functional magnetic resonance imaging (fMRI), musculoskeletal MRI, Patient Reported Outcomes Measurement Information System (PROMIS) questionnaires, fluid markers informing on inflammation (i.e., CRP and ESR levels) and clinical status. All evaluated patients had either past or ongoing hand joint abnormalities. Patient enrollment is currently active.
FMRI data collected during a hand motor task involved a visually cued, opening and closing of the right or left hand (depending on location of joint pathology or clinical pain) in a 30 second off/10 second on manner for 5 cycles. Evoked stimulation was subsequently performed by applying cold stimuli (10°C) to hand and knee joints also in a 30 second off/10 second on block design (Medoc LTD, Israel). Immediately following fMRI, patients underwent hand MRI (index hand only). All imaging was performed on a Siemens 3T scanner (Siemens, Germany). fMRI data was analyzed using FSL 6.0, while hand MRI was clinically evaluated by a musculoskeletal radiologist (KE). This study was approved by the Institutional Review Board at Boston Children’s Hospital.
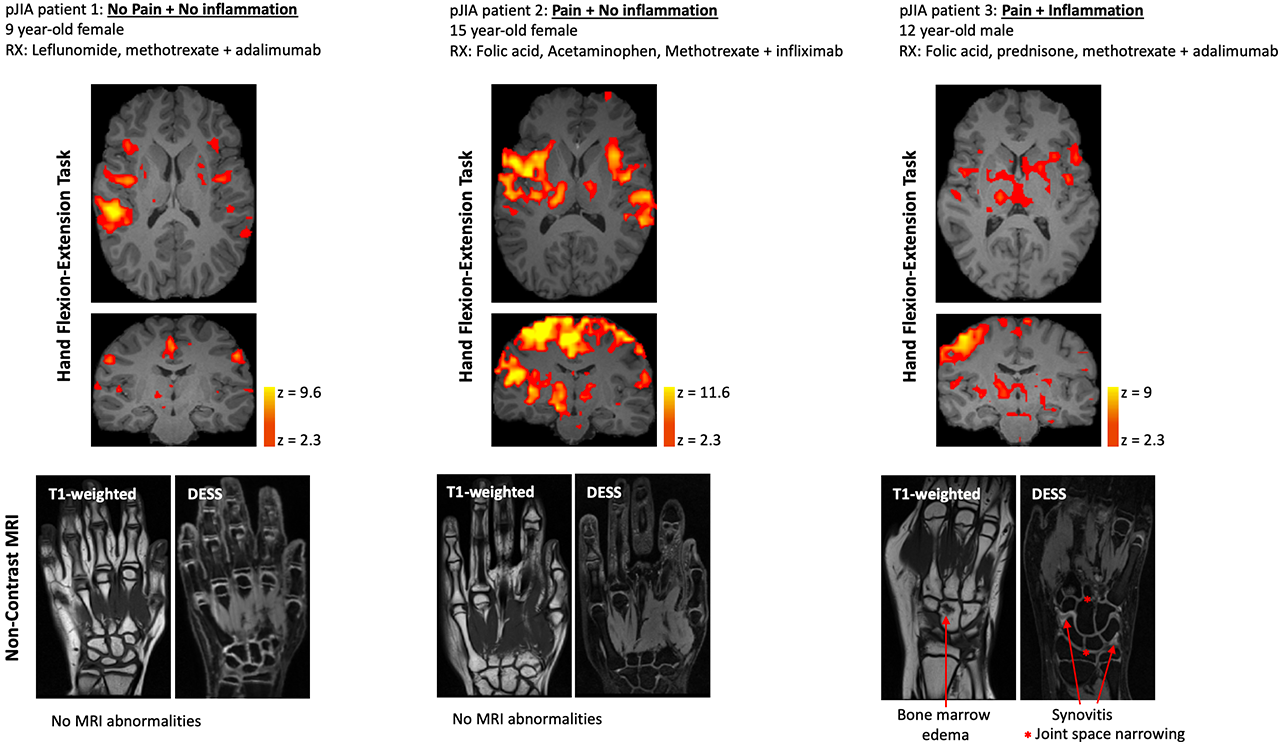
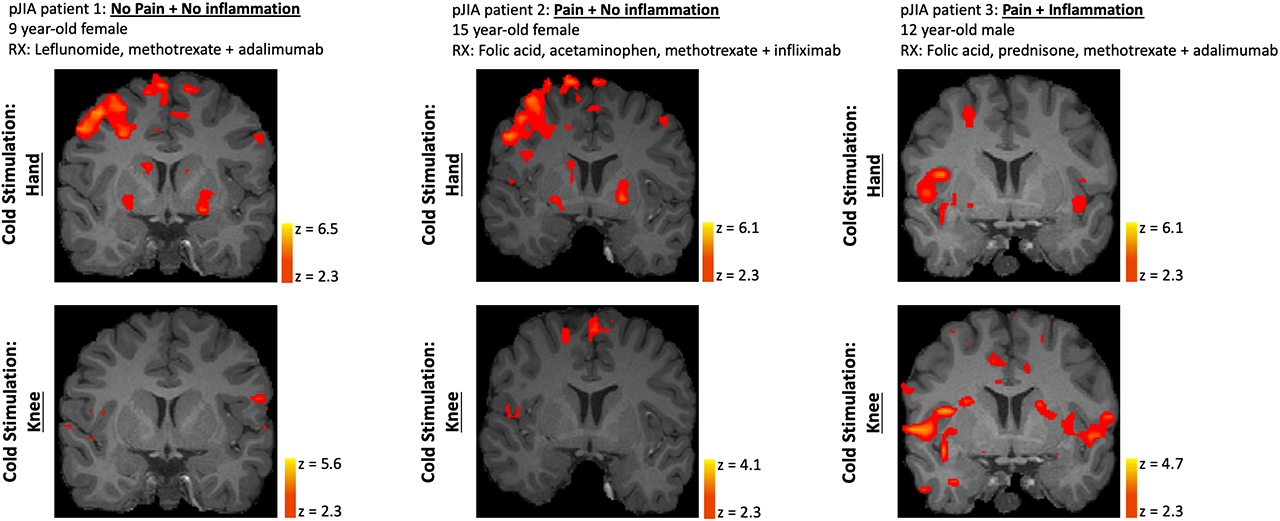
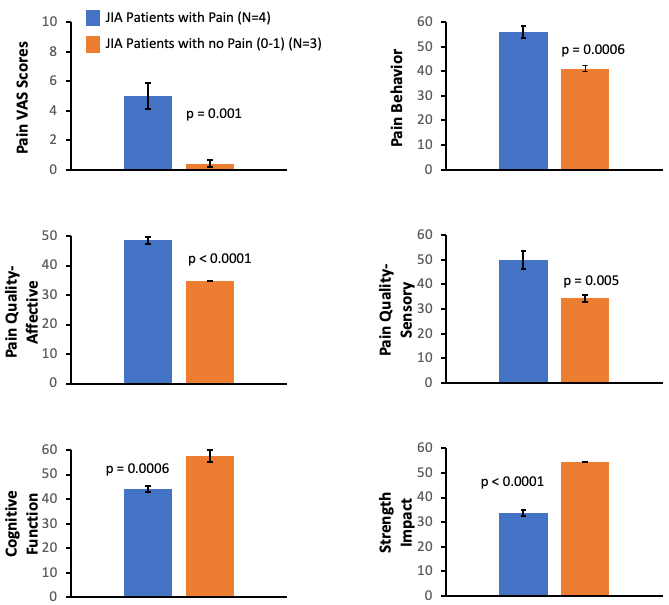
Results: Hand motor task fMRI showed differential CNS activation profiles amongst patients with No Pain + No inflammation, Pain + No Inflammation and Pain + Inflammation (Figure 1). Of these states, the pain without inflammation (or other pathology) sub-type yielded the most robust CNS activation. MRI abnormalities detected in the hand in Patient 3 consisted of (teno-)synovitis, bone marrow lesions and joint space narrowing. Cold stimuli yielded comparable responses across pain and inflammation conditions (Figure 2). Interestingly, in the pJIA patient with current hand/wrist and past knee joint abnormalities, evoked CNS responses and pain scores to cold stimuli were similar at either site. Finally, from PROMIS-based questionnaires (Figure 3), pJIA patients with pain reported a greater extent of loss of functions (cognition) and gain of functions (behaviors altered by pain).
Conclusion: For the first time, a neuroimaging-based assessment of pJIA patients was executed. This allowed for novel insight to be gained regarding potential neurobiological factors driving pain in pJIA. The current multidisciplinary datasets are suggestive of non-inflammatory (centralized or neuropathic) and inflammatory pain mechanisms at play in pJIA.
1. Giancane, Clin Exp Rheumatol. (2017)
2. Shiff, Pain. (2018)
To cite this abstract in AMA style:
Upadhyay J, Sibai D, Labadie R, Lemme J, Sieberg C, Ecklund K, Borsook D, Sundel R. Elucidating Pain Mechanisms in Polyarticular Juvenile Idiopathic Arthritis Patients [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/elucidating-pain-mechanisms-in-polyarticular-juvenile-idiopathic-arthritis-patients/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/elucidating-pain-mechanisms-in-polyarticular-juvenile-idiopathic-arthritis-patients/