Session Information
Date: Monday, November 6, 2017
Title: Plenary Session II
Session Type: ACR Plenary Session
Session Time: 11:00AM-12:30PM
Background/Purpose: Although intra-articular injection of corticosteroids (IAIC) has been one of the modalities of treatment for symptomatic knee OA, the recommendations for its use are inconsistent. Recently, a randomized clinical trial (RCT) reported that IAIC didn¡¯t significantly improve pain, but instead resulted in greater cartilage volume loss compared with saline injections. To examine this unexpected finding in a real-life non-trial setting, we investigated IAIC in relation to knee radiographic osteoarthritis (ROA) progression in a prospective cohort study.
Methods: We conducted a propensity score matched cohort study to examine the effect of IAIC on the risk of knee ROA progression using data collected from the Osteoarthritis Initiative up to 8 years follow-up. Eligible subjects consisted of those who had at least one knee with a K/L grade of 2 or 3 and did not have IAIC at baseline. We identified subjects with incident knee IAIC during the study period. Knee ROA progression was defined as K/L grade worsening or knee replacement therapy during the follow-up. We used logistic regression model to calculate propensity scores for IAIC within each 1-year time block. The predictors for IAIC in the logistic regression model included age, sex, BMI, education, WOMAC pain score, knee injury history, physical activity level, NSAIDs use and K/L grade. Up to four knees without IAIC were propensity score matched to a knee with incident IAIC within each 1-year accrual block. Subjects were followed to the date of ROA progression, lost to follow-up, death or end of the follow-up, whichever came first. We plotted cumulative risk of ROA progression using Kaplan¨CMeier curves for each cohort accounting for competing risk. We fitted a Cox proportional-hazards model to examine the relation of IAIC to the risk of ROA progression.
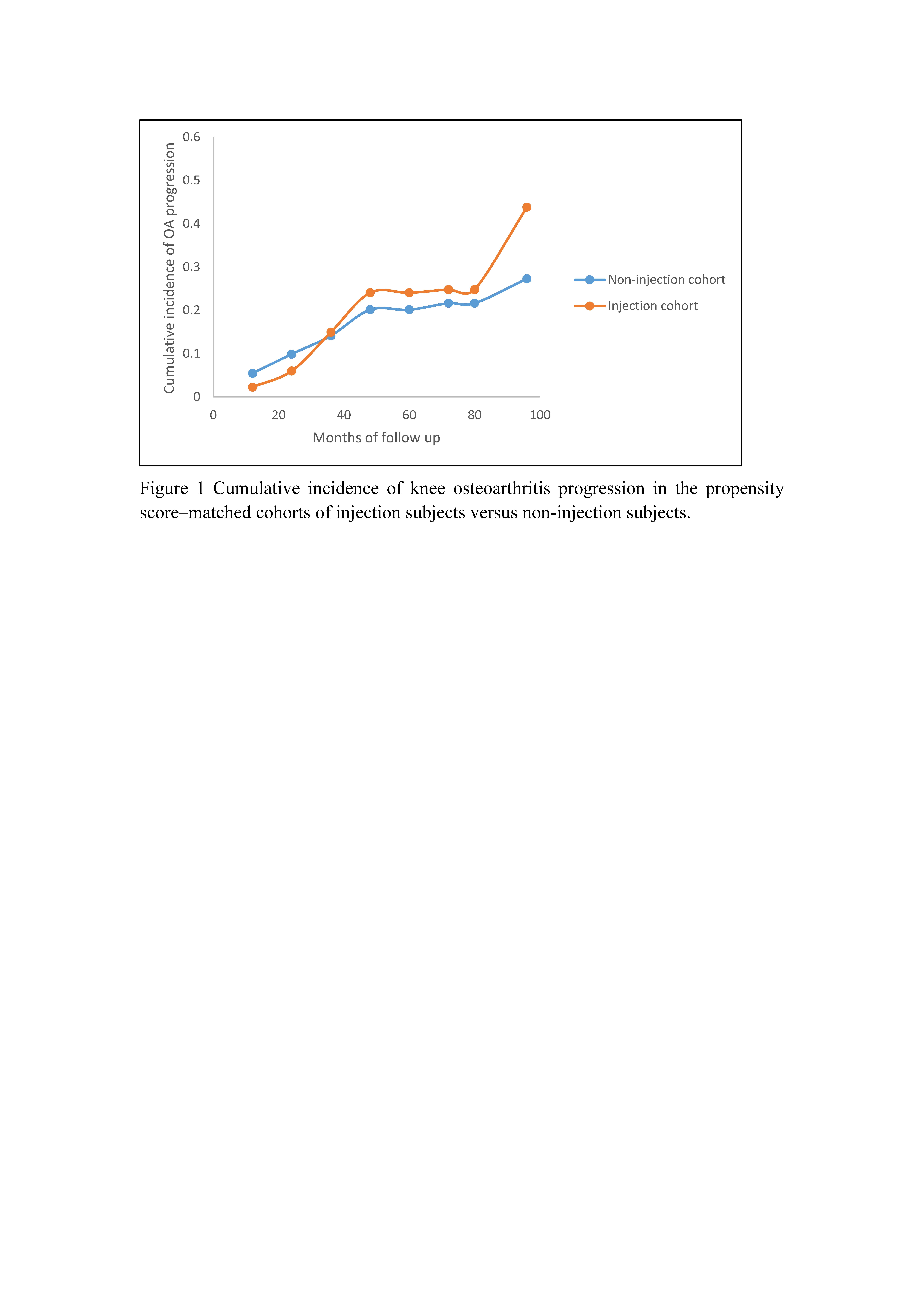
Results: Baseline characteristics were well-balanced between IAIC and non-IAIC cohorts (Table 1). Risk of ROA progression was higher among knees with IAIC (60.86 per 1000 person-years) than those without IAIC (38.02 per 1000 person-years) during the follow-up (Figure 1). Compared with knees without IAIC, the hazard ratio of ROA progression for knees with IAIC was 1.60 (95%CI: 1.21 to 2.12). The associations appeared stronger among women (HR=1.71, 95%CI: 1.22 to 2.40) than men (HR=1.38, 95%CI: 0.84 to 2.28) although the effect estimate in men was not statistically significant owing to relatively small sample size (Table 1).
Conclusion: We found that knees with IAIC experienced higher risk of knee ROA progression than those without IAIC in a real-life setting, consistent with the recent RCT results.
To cite this abstract in AMA style:
Lei GH, Zeng C, Wei J, Wang YL, Xie DX. Dose Intra-Articular Injection of Corticosteroids Increase the Risk of Knee Osteoarthritis Progression? Data from the Osteoarthritis Initiative [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/dose-intra-articular-injection-of-corticosteroids-increase-the-risk-of-knee-osteoarthritis-progression-data-from-the-osteoarthritis-initiative/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/dose-intra-articular-injection-of-corticosteroids-increase-the-risk-of-knee-osteoarthritis-progression-data-from-the-osteoarthritis-initiative/