Session Information
Session Type: ACR Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: To study the relationship between clinically-determined disease activity and vascular inflammation assessed by positron emission tomography (PET) in patients with TakayasuÕs arteritis (TAK).
Methods: Patients with new or relapsing TAK were evaluated at 5 centers. Whole body 18F-flurodeoxyglucose (FDG)PET-CT imaging was performed during a period of clinical disease activity. Clinical assessments were performed blinded to PET scan findings. A single nuclear medicine physician interpreted all of the PET scans, blinded to clinical data, to determine presence of active vasculitis based on degree of arterial FDG uptake. Classification and regression tree analysis (CART) defined predictors of PET scan activity. Elevated acute phase reactants (ESR>30mm/hr, CRP>10mg/L), prednisone dose at time of imaging, ongoing use of other immunosuppressive agents for >1 month at time of clinical assessment, interval between clinical and imaging assessments, and clinical features of disease activity (vascular vs nonspecific) were studied within the CART models. Vascular features included asymptomatic disease progression by angiography. Non-specific features of disease activity were defined as constitutional symptoms accompanied by elevated acute phase reactants in the absence of signs or symptoms of vascular involvement.
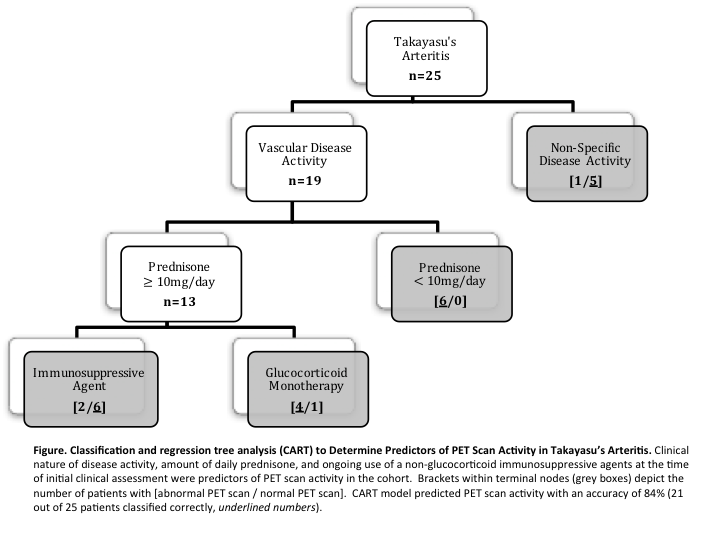
Results: Clinical assessments were performed in 25 patients with TAK, and PET scans were performed a mean of 7 days later. FDG-PET findings were suggestive of active vasculitis in 13 of 25 patients (52%). Interval increase in glucocorticoid therapy between clinical assessment and imaging occurred in 4/13 (31%) patients with an active scan and 5/12 (42%) patients with an inactive scan (p=0.69). CART analysis predicted FDG-PET scan activity with 84% accuracy based upon 3 variables: clinical features of disease activity, prednisone dose at the time of imaging, and use of a non-glucocorticoid immunosuppressive agent (Figure). Acute phase reactants and time interval delay between clinical and imaging assessments were not predictive within the model. Clinical features of disease were the strongest determinant of vascular activity on FDG-PET. Among patients with vascular symptoms of disease activity, use of <10mg daily prednisone at the time of imaging assessment and treatment with glucocorticoid monotherapy were associated with increased probability of active vasculitis on FDG-PET.
Conclusion: Clinical features of disease and treatment status are associated with different findings on vascular FDG-PET scan in TAK. Clinical studies that incorporate imaging-based assessment of disease activity in TAK should ideally obtain baseline imaging studies prior to the initiation of glucocorticoid therapy and should consider exclusion of patients with exclusively non-specific symptoms of disease activity.
To cite this abstract in AMA style:
Grayson PC, Ahlman M, Marinelli K, Borchin R, Carette S, Khalidi NA, Langford CA, McAlear CA, Monach PA, Pagnoux C, Warrington KJ, Ytterberg SR, Merkel PA. Discrepancies between Clinical- and Imaging-Based Assessments of Disease Activity in Takayasu’s Arteritis [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/discrepancies-between-clinical-and-imaging-based-assessments-of-disease-activity-in-takayasus-arteritis/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/discrepancies-between-clinical-and-imaging-based-assessments-of-disease-activity-in-takayasus-arteritis/