Session Information
Date: Monday, October 22, 2018
Title: Patient Outcomes, Preferences, and Attitudes Poster I: Patient-Reported Outcomes
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Most studies evaluating patient-reported outcomes such as the PROMIS Physical Function Short Form 10a (PF10a) in rheumatoid arthritis (RA) have been performed in white and English-speaking populations. We assessed the measurement properties of the PF10a in a racially/ethnically diverse population with RA. We determined the effect of non-English language proficiency, insurance status and race/ethnicity, on the validity and responsiveness of the PF10a.
Methods: Data were derived from electronic health records for all RA patients seen in a university rheumatology clinic between February 2013 and October 2017. We evaluated the PF10a’s floor and ceiling effects across categories of language preference, insurance and race/ethnicity. To assess convergent and discriminant validity, we examined Spearman’s correlation coefficients (r) between the PF10a and other patient-reported outcomes (patient global assessment and pain), clinical outcomes (tender and swollen joint counts) and inflammatory markers (ESR and CRP) across population subgroups. We used linear mixed effects models to evaluate the responsiveness of the PF10a to longitudinal changes in the Clinical Disease Activity Index (CDAI) across population subgroups.
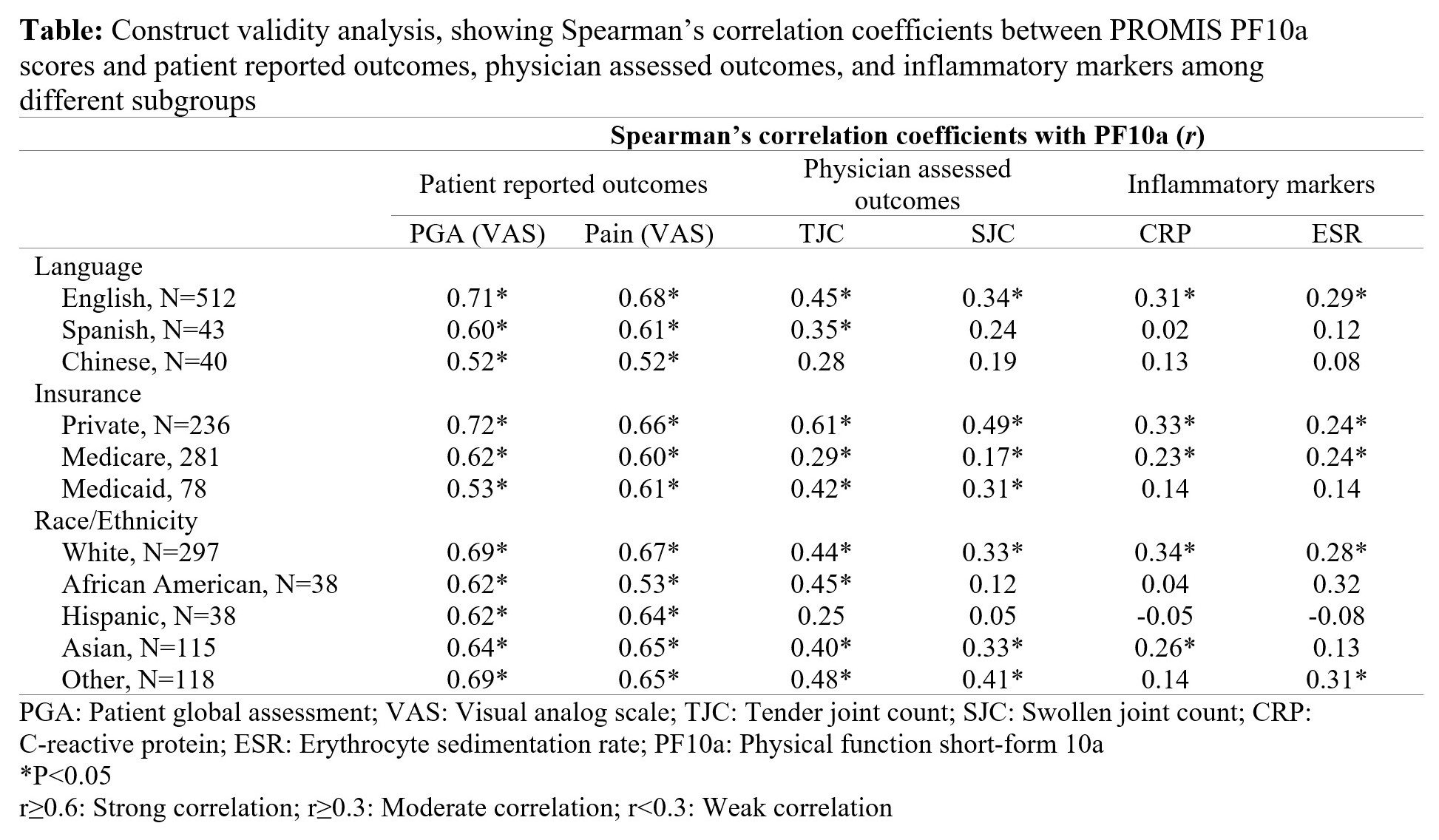
Results: We included 595 patients with complete data in a cross-sectional analysis of validity and 341 patients in longitudinal analyses of responsiveness. The group was racially/ethnically diverse (50% non-white) and 14% preferred a language other than English. Most patients had Medicare (47%) or private (40%) insurance. Mean (SD) PF10a score was 40 (11), nearly a standard deviation lower than the overall US population mean. PF10a had acceptable floor (≤7.5%) and ceiling (≤11%) effects across population subgroups. As expected, we observed strong correlations (r≥0.6) with patient-reported outcomes, and moderate correlations (r≥0.3) with clinical outcomes among whites, English speakers and privately insured patients (Table). However, constructs evaluated by the PF10a were less correlated with clinical outcomes among Chinese speakers and Hispanics (r<0.3 and statistically non-significant), and less sensitive to clinical improvements among Medicaid patients (p=0.005) and Spanish speakers (p=0.029) (Figure).
Conclusion: Consistent with published research, the PF10a had good measurement properties among whites, English speakers and privately insured patients. However, we also found important differences across racial/ethnic groups and those with limited English proficiency that warrant further investigation.
To cite this abstract in AMA style:
Izadi Z, Katz P, Schmajuk G, Gandrup J, Li J, Gianfrancesco M, Yazdany J. Differences in the Measurement Properties of the Patient-Reported Outcomes Measurement Information System Physical Function Short-Form 10a Among Racial/Ethnic Minorities with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2018; 70 (suppl 9). https://acrabstracts.org/abstract/differences-in-the-measurement-properties-of-the-patient-reported-outcomes-measurement-information-system-physical-function-short-form-10a-among-racial-ethnic-minorities-with-rheumatoid-arthritis/. Accessed .« Back to 2018 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/differences-in-the-measurement-properties-of-the-patient-reported-outcomes-measurement-information-system-physical-function-short-form-10a-among-racial-ethnic-minorities-with-rheumatoid-arthritis/