Session Information
Date: Friday, November 6, 2020
Title: RA – Diagnosis, Manifestations, & Outcomes Poster I: Multimorbidity
Session Type: Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: Depression and depressive symptoms are common but under-recognized in rheumatoid arthritis (RA). Few studies have examined depression symptoms in RA patients compared to clinically diagnosed depression, and their role as mortality predictors. The objectives of the present study were to examine the prevalence of depression symptoms compared to clinically diagnosed depression and to examine the association of depression with mortality in RA patients.
Methods: We studied a cohort of RA patients who met the 1987 classification criteria, recruited from 1996 through 2011. All underwent a comprehensive clinical and psychosocial evaluation using standardized instruments. Depressive symptoms were measured with the Center for Epidemiologic Studies Depression Scale (CESD), adjusted for RA (CESD-RA) by eliminating items that may overlap with symptoms of RA. We considered depression as present when the CESD score was ≥ 16. To quantify RA disease activity, we used the DAS28 ESR (DAS28). All deaths were confirmed with a death certificate. Multivariable logistic regression models were fit to examine the combined influence of independent variables on the outcome
Results: We studied 1328 RA patients, 981 of whom were women (74%). A clinical diagnosis of depression was found in the medical records of 220 patients (17%), significantly fewer than the 361 (27%) with significant depression symptoms on the CESD (P < 0.0001). There were 305 deaths during the study period. Of the patients who died, 31 had been diagnosed clinically with depression (10%), but 75 had significant depression symptoms on the CESD (26%). Patients with depression or significant depression symptoms were younger than patients without them, mean age 53 years (95% CI 52, 54) vs. 58 years (95% CI 57, 59), P < 0.0001, and more likely to be women, 82% vs. 69%, OR 1.97, (95% CI 1.48, 2.63), P < 0.0001. Patients with significant depression symptoms had greater disease activity than those without them, mean DAS28ESR 5.1 (95% CI 5.0, 5.3) vs. 4.0 (95% CI 3.9, 4.1), P < 0.001).
Logistic regression analysis adjusted for age and sex revealed that significant depression symptoms predicted all-cause mortality, OR 1.77 (95% CI 1.49, 2.12), P < 0.001, but clinically diagnosed depression did not.
Conclusion: Significant depression symptoms in RA are more frequent than depression diagnosed clinically, suggesting that some patients with depression may go undiagnosed. Depression symptoms predicted mortality in RA patients, while a clinical diagnosis of depression did not. Our findings suggest that strategies to improve the recognition of depression in RA should be studied further.
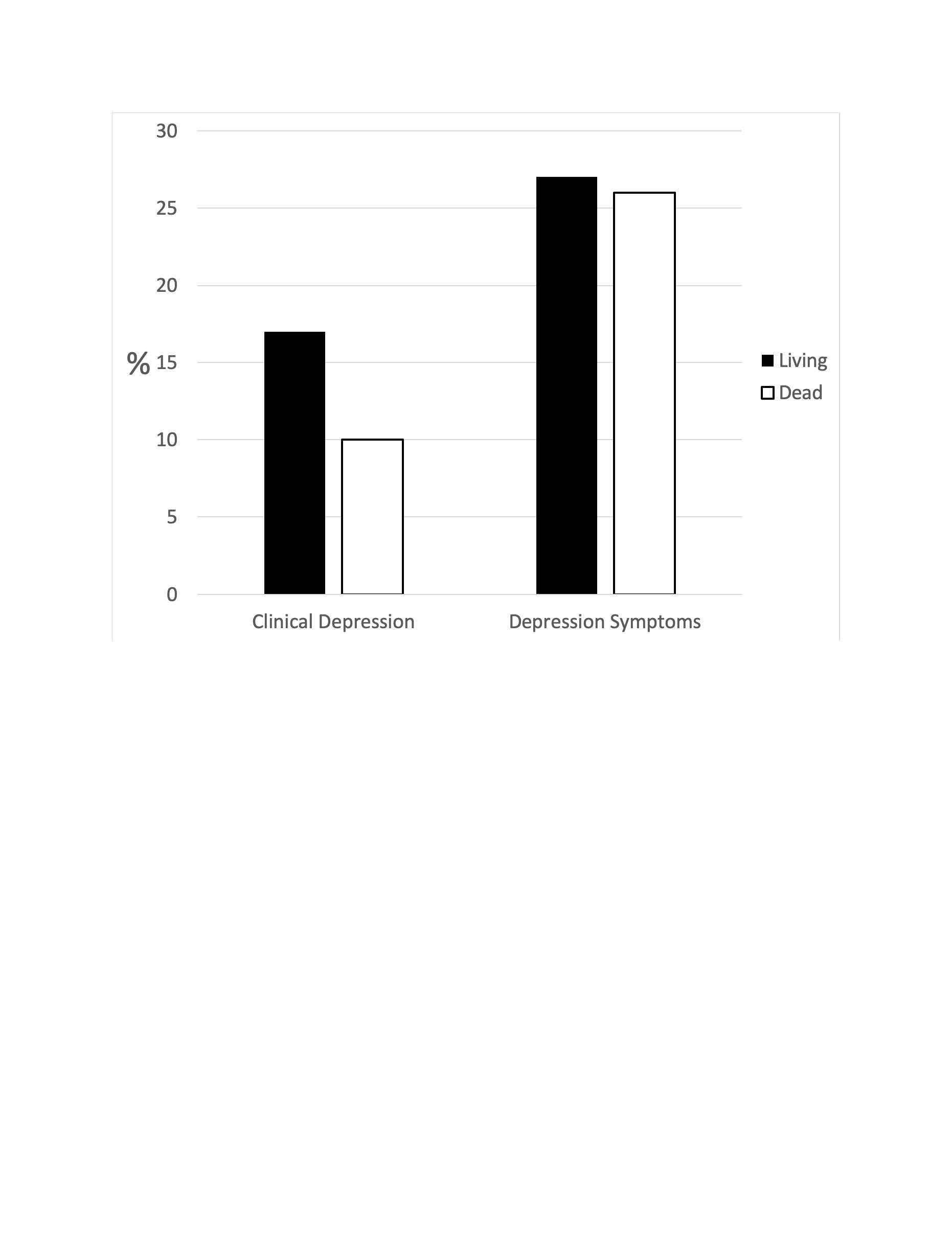 Figure. Significant depression symptoms were more frequent than clinically diagnosed depression in both patients who survived as well as in those who died (P < 0.001)
Figure. Significant depression symptoms were more frequent than clinically diagnosed depression in both patients who survived as well as in those who died (P < 0.001)
To cite this abstract in AMA style:
Restrepo J, Del Rincon I, Escalante A. Depression Symptoms but Not Clinically Diagnosed Depression Predict Mortality in Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/depression-symptoms-but-not-clinically-diagnosed-depression-predict-mortality-in-rheumatoid-arthritis/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/depression-symptoms-but-not-clinically-diagnosed-depression-predict-mortality-in-rheumatoid-arthritis/
