Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: Women with rheumatoid arthritis (RA) often take medications to control disease activity that, should a woman become pregnant, may increase the risk of poor pregnancy outcomes, such as miscarriage and birth defects. The objective of this study was to determine if women with RA are using highly effective contraceptives, and if contraception differs by current medication use.
Methods: Women with RA (2010 ACR/EULAR criteria) aged 20-40 seen in a university clinic without a history of ovarian surgery or prior exposure to possible ovary-toxic medications were invited to participate in a cross-sectional survey. The survey included questions on current medications taken for RA and contraceptive methods used in the previous three months. Contraceptive methods were categorized as highly effective (tubal ligation or vasectomy, IUD, Implanon/Nexplanon), effective (progesterone-only pill, estrogen-containing pill, Depo-Provera injections), and ineffective (abstinence, patient didn’t think she could get pregnant, withdrawal, condoms, diaphragm, and none). Additionally, patients were asked if they had discussed contraceptives with their rheumatologist. Contraceptive methods were reported as counts and frequencies overall and in each medication class, and Fisher’s exact test analyzed differences across medication classes.
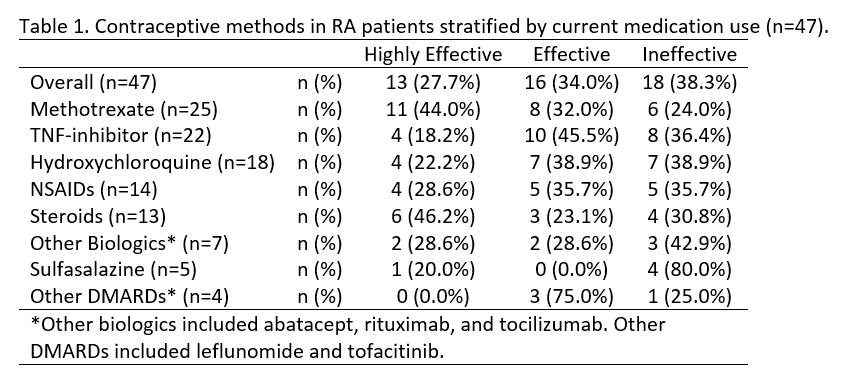
Results: There were 52 RA patients; 79% white with a mean age of 32 and mean RA duration of 9 years. Education beyond high school was completed by 98% of patients, 61% of patients were married, and 56% of patients worked full time. Discussing contraception with their rheumatologist was recalled by 71% of patients. Current medications included TNF-inhibitor (50%), methotrexate (48%), hydroxychloroquine (38%), NSAIDs (31%), corticosteroids (29%), sulfasalazine (15%), other biologics (13%), and other DMARDs (8%). In the 47 patients of reproductive age who were not trying to conceive, 38% were using ineffective, 34% were using effective, and 28% were using highly effective contraceptive methods (Table 1). Among 25 methotrexate users, 44% were using highly effective contraceptives, compared to 9% of patients not taking methotrexate (p=0.02). However, 24% of methotrexate users were using ineffective contraceptives. Among patients taking other DMARDs or biologics, drugs with very limited pregnancy safety information, 18% were using highly effective, 45% were using effective, and 36% were using ineffective contraceptive methods.
Conclusion: In this highly educated group of RA patients, most women were using effective or highly effective methods of contraception. It appears that rheumatologists are targeting highly effective contraceptives to women who are taking methotrexate, a highly teratogenic drug. However, there is room for improvement for women taking newer DMARDs and biologics, for which we have inadequate safety data in pregnancy.
To cite this abstract in AMA style:
Clowse MEB, McDaniel G, Eudy AM. Contraceptive Methods in Women with Rheumatoid Arthritis [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/contraceptive-methods-in-women-with-rheumatoid-arthritis/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/contraceptive-methods-in-women-with-rheumatoid-arthritis/