Session Information
Session Type: ACR Abstract Session
Session Time: 4:30PM-6:00PM
Background/Purpose: Development of new disease-modifying drugs in osteoarthritis (DMOADs) has proven difficult and is complicated by heterogeneous study populations and insensitive endpoints of structural change, symptomatic benefit, and discordances between structural disease severity and reported symptoms. In such trials, counterintuitively, mild structural disease may be associated with severe symptoms and vice versa. The reasons for this discordance are unknown, and research to uncover factors potentially distorting the perceived severity of symptoms is needed to better characterize the clinical relevance of structural improvement, if any, in DMOAD trials. Psychological conditions including anxiety and depressive disorders (ADD) as well as concurrent pain conditions are known to affect pain sensitivity and perception, and as common co-morbidities of osteoarthritis (OA), these conditions may partly explain the observed discordance between structure and symptoms, and if established, exclusion of patients with such co-morbidities in DMOAD trials could potentially improve the understanding of structural benefit in a clinical context.
The purpose of this analysis was to investigate the impact of ADD and back pain (BP) on the association between structural features of OA and the patient-reported pain.
Methods: Baseline data from two phase 3 clinical trials investigating oral salmon calcitonin in OA, NCT00486434 and NCT00704847 (total N=2206), was analyzed in a post-hoc cross-sectional analysis. Patients with self-reported depression, anxiety, post-traumatic stress syndrome (PTSD), either present or previous, were selected and compared with a control group, matched by sex, age, BMI and Kellgren Lawrence (KL) grade. The correlations between Joint-Space Width (JSW), and the WOMAC Pain Score were plotted for the ADD group and ADD controls, and Spearman’s correlation analysis was performed for both ADD and BP groups.
Results: In the ADD group, 149 patients had AD in medical history of which 123 were ongoing at baseline. In the BP group, 333 patients had BP in medical history of which 322 were ongoing at baseline. The study groups of ADD, BP and respective matched controls (MC) were highly similar in terms of age, sex, BMI, JSW, KL-grade and WOMAC pain.
Associations between pain and JSW
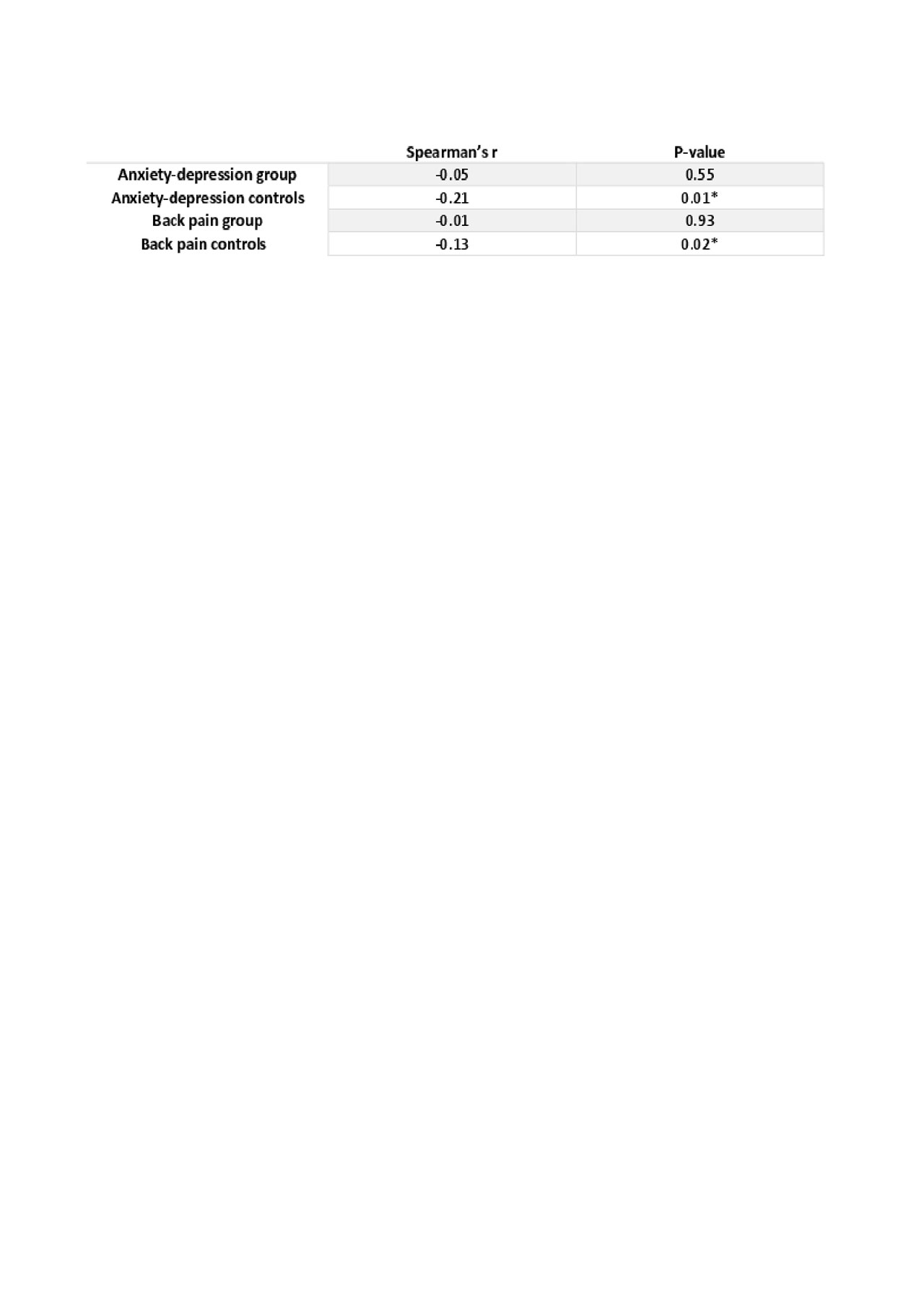
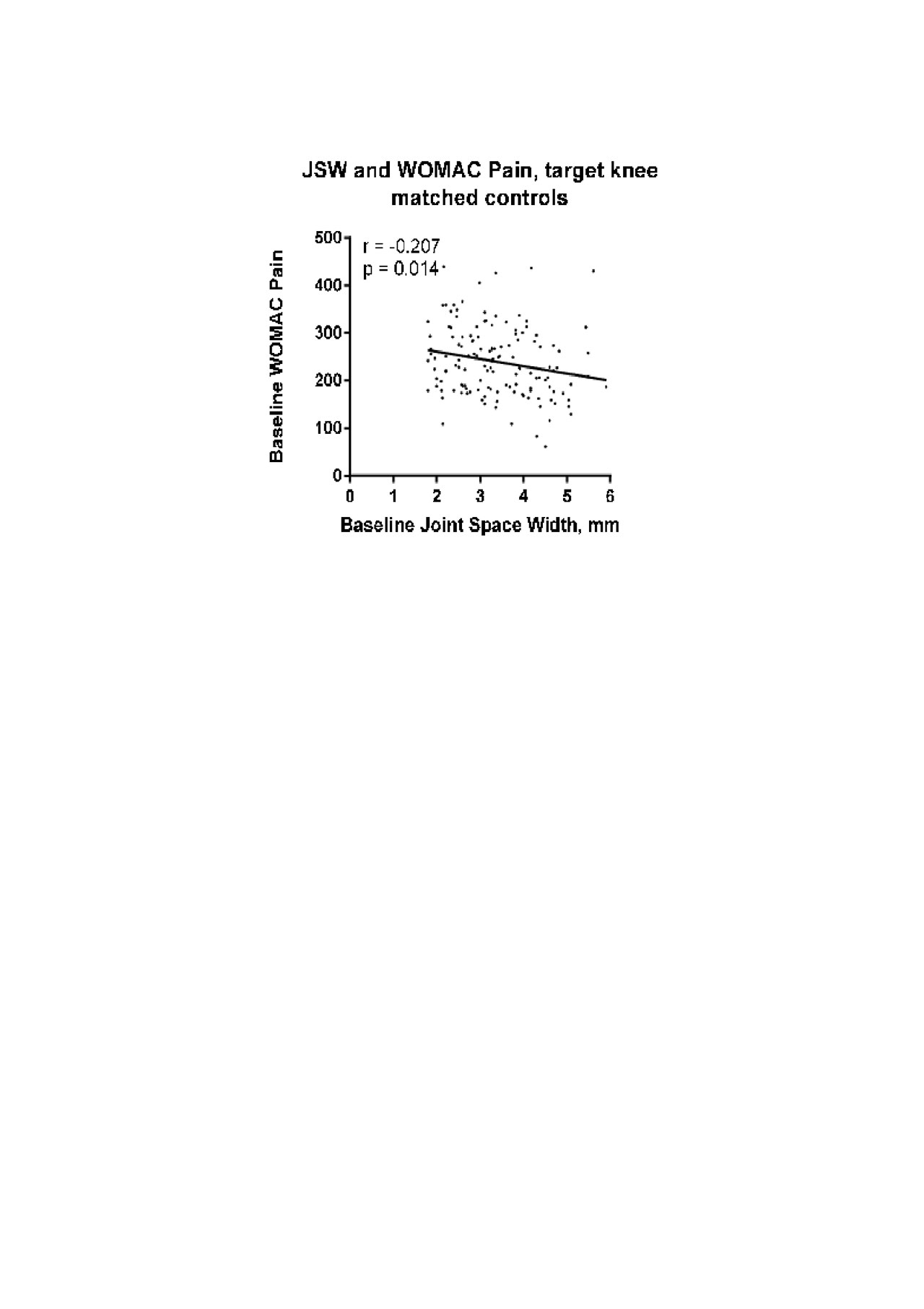
Referring to table 1, no correlation was found in the ADD and BP group between JSW and WOMAC pain. In the respective MC groups, statistically significant correlations (MC for ADD: R= -0.21, p = 0.01, and MC for BP: R=-0.13, p=0.02) was found between JSW and pain indicating that lower JSW was associated with higher pain in the control groups but not in the ADD or BP groups. The univariate linear relationship between JSW and pain in the ADD and MC groups are illustrated in Figure 1 and 2.
Conclusion: A marked structure-symptoms discordance was found in OA patients with ADD and BP, while a statistically significant correlation was seen in matched controls without ADD or BP. The results suggest that exclusion of trial patients with anxiety and depression and/or back pain in medical history may improve the accuracy of pain reporting in clinical OA trials.
To cite this abstract in AMA style:
Bjerre-Bastos J, Byrjalsen I, Karsdal M, Andersen J, Bihlet A. Co-morbidities Associated with Discordance Between Structural Severity and Pain in Osteoarthritis: Implications for Clinical Trial Design in OA – a Post-Hoc Analysis of Data from Two Randomized Controlled Trials [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/co-morbidities-associated-with-discordance-between-structural-severity-and-pain-in-osteoarthritis-implications-for-clinical-trial-design-in-oa-a-post-hoc-analysis-of-data-from-two-randomize/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/co-morbidities-associated-with-discordance-between-structural-severity-and-pain-in-osteoarthritis-implications-for-clinical-trial-design-in-oa-a-post-hoc-analysis-of-data-from-two-randomize/