Session Information
Date: Sunday, November 10, 2019
Title: RA – Diagnosis, Manifestations, & Outcomes Poster I: Risk Factors, Predictors, & Prognosis
Session Type: Poster Session (Sunday)
Session Time: 9:00AM-11:00AM
Background/Purpose: The Targeting Immune Responses for Prevention of RA (TIP-RA) Collaborative prospectively studies individuals at high risk for developing RA because of serum ACPA positivity in absence of inflammatory arthritis (IA) at baseline. The objectives of the analyses presented herein are to evaluate ACPA+ ACPA- individuals to identify factors associated with each of these states, and to identify factors associated with incident inflammatory arthritis and classifiable RA.
Methods: 87 ACPA+ subjects were identified who at their baseline study visit did not have historical or examination (66/68 count) evidence of IA, and 160 ACPA- matched controls. ACPA+ was defined as a serum elevation of anti-CCP3 (IgG, Inova) on ≥2 occasions above the manufacturer’s suggested cut-off (≥20 units). Subjects were recruited through screening of health-fair particiants, first-degree relatives of patients with RA and individuals referred to rheumatology clinics. Subjects were followed annually or sooner if they had changes in joint symptoms. Clinical and biomarker factors, including RF IgA and M (Inova) and C-reactive protein (CRP), were assessed. Comparisons between ACPA+/- subjects were performed, and factors associated with incident IA/RA within the ACPA+ subjects were evaluated.
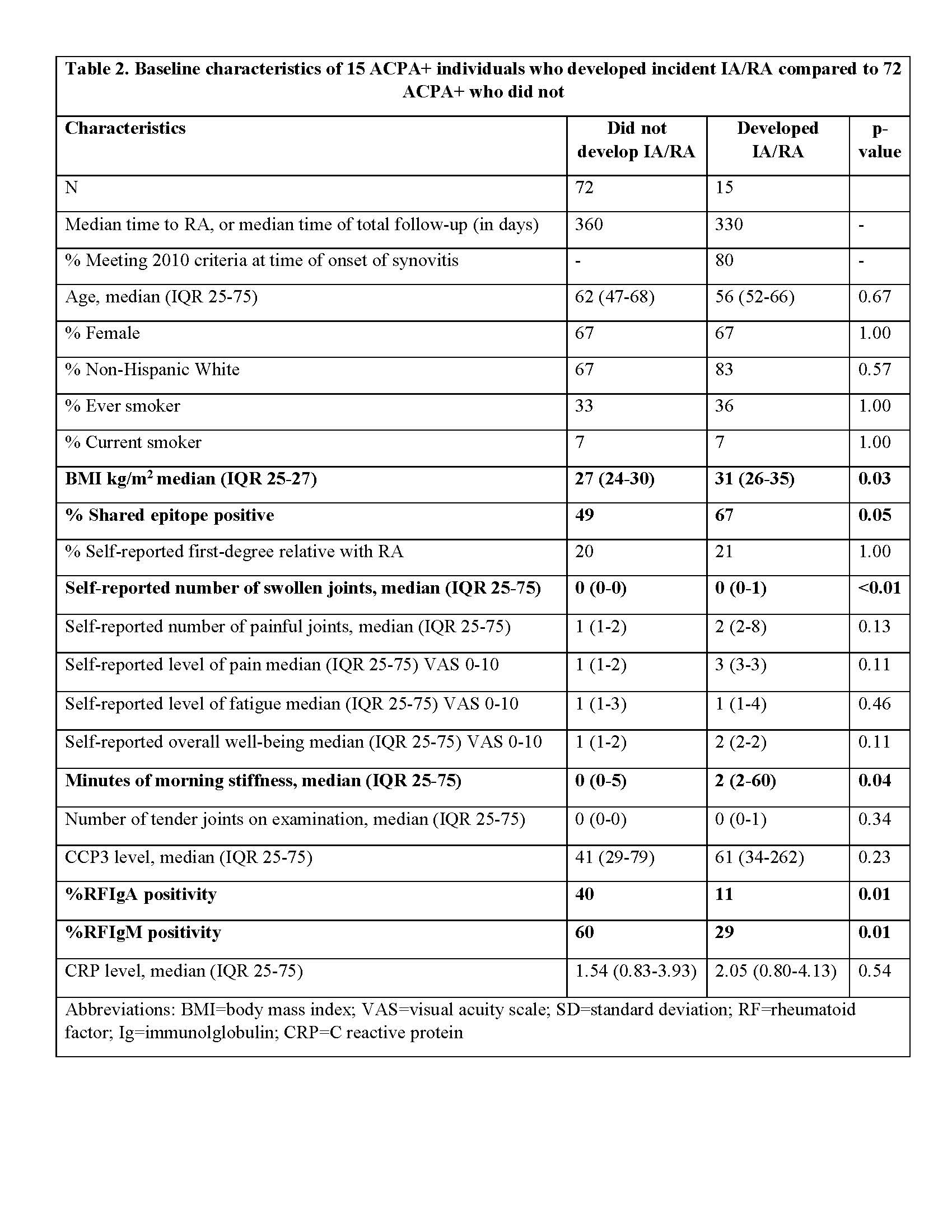
Results: The baseline characteristics of ACPA+/- subjects are presented in Table 1. Self-reported fatigue was higher in ACPA+ vs ACPA- subjects. In addition, within ACPA+ subjects, current smoking was associated with increased morning stiffness, and higher CRP was associated with increased fatigue. Within ACPA+ subjects, 15 (17%) developed IA/RA a median of 330 days after baseline. At baseline, higher BMI, greater number of self-reported swollen joints, the presence of the shared epitope (SE) and positivity for RFIgA and M were each associated with increased risk for developing incident IA/RA (Table 2).
Conclusion: Within this cohort, a greater level of fatigue is associated with ACPA positivity. Furthermore, within ACPA+ subjects, smoking and elevated hsCRP are associated with clinical symptoms of stiffness and fatigue, respectively. These symptoms may be part of a prodrome for future RA, but also may indicate a unique ‘autoimmune-opathy’ that warrants further investigation into pathogenesis and treatment. These findings also suggest a role for smoking and increased joint-related symptoms. The association of high BMI with incident IA/RA has been identified prior (de Hair 2013) and the replication of that herein may identify this as a potentially modifiable risk factor for future RA. Furthermore, the risk of incident IA/RA with a higher number of self-reported swollen joints at baseline suggests that individuals may sense joint abnormalities prior to detection of swelling on physical examination. The risk of incident RA with RFIgA and M positivity also highlights the importance of a combination of ACPA and RF in the pathogenesis of joint disease, and the potential role of the SE in transition from ACPA positivity to arthritis is also intriguing. This study will continue with further evaluation of factors that may be predictive of or causally linked to the future onset of RA.
To cite this abstract in AMA style:
Deane K, Nagpal S, Holers V, Firestein G, Boyle D, Seifert J, Buckner J, James E, Moss L, Barzideh S, Posso S, Robinson W, Polinski K, Gilmore R, Baribaud F, Rao N, Vratsanos G. Clinical and Biomarker Factor Associations with Symptoms and Future Development of RA: TIP-RA Collective [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/clinical-and-biomarker-factor-associations-with-symptoms-and-future-development-of-ra-tip-ra-collective/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/clinical-and-biomarker-factor-associations-with-symptoms-and-future-development-of-ra-tip-ra-collective/