Session Information
Date: Monday, November 6, 2017
Title: Systemic Lupus Erythematosus – Clinical Aspects and Treatment Poster II: Damage and Comorbidities
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Childhood-onset SLE (cSLE) often presents with severe disease, managed with high-dose steroids. However, little is known about differences in long-term steroid toxicity between adults with cSLE and adult-onset SLE (aSLE). The goal of this study was to determine whether adults with cSLE are at increased risk for steroid-related and total disease damage as compared to aSLE, and whether they accumulate more disease damage over time.
Methods: Data derive from the 2005-2012 cycles of the Lupus Outcomes Study, a cohort of adults with SLE confirmed by chart review using ACR classification criteria, followed by annual telephone surveys. The Brief Index of Lupus Damage (BILD), a validated, patient-reported measure, was used to assess SLE-associated damage. Participants age 18-63 were included in the analysis (N=897). Those diagnosed at age < 18 years were defined as cSLE (N=113). Outcome variables included total BILD scores at baseline and follow-up (mean=6.3±1.7 years between assessments), and presence of steroid-related damage at any point during the study. Steroid-related damage was defined as a self-reported history of cataracts, osteoporosis, avascular necrosis (AVN) or diabetes mellitus (DM). Logistic regression and negative binomial regression were used to compare cSLE and aSLE groups, adjusting for sex, ethnicity, baseline age and baseline disease duration. General health predictors (hypertension, obesity) and medication predictors (steroid use ever) associated with steroid-related damage were included in the steroid damage analysis.
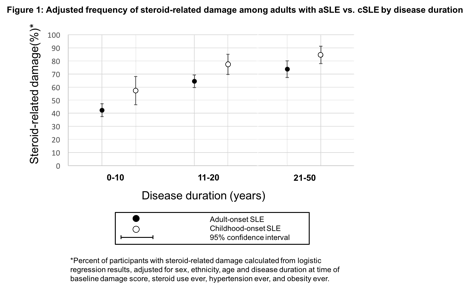
Results: Participants with cSLE were younger (mean age 32±10 vs. 47±10; p<0.001), more likely to be male (12% vs 7%; p=0.05) and less likely to be white (41% vs. 57%; p<0.001). Mean age at diagnosis was 14 (±3) for the cSLE vs. 33 (±10) for aSLE group. Median disease duration was 16 years (range 4-50) for participants with cSLE and 12 years (range 0-42) for aSLE. Nearly all participants reported a history of steroid use. There was no difference in unadjusted frequency of steroid-related damage between cSLE and aSLE groups (59% vs. 60%). However, in adjusted analysis, participants with cSLE were twice as likely to report steroid-related damage (72% vs. 58%, p<0.0001, OR 2.0, 95% CI 1.2-3.4). Steroid-related damage also increased significantly with increased disease duration for both groups (Figure 1). Mean damage score at baseline and increase in damage score over 6.3±1.7 year follow up did not differ between groups in unadjusted or adjusted analyses.
Conclusion: In this large cohort of adults with SLE, childhood-onset predicted increased risk of steroid-related damage. Participants with cSLE and aSLE continued to accumulate disease-related damage at similar frequencies over time. More aggressive use of steroid-sparing management strategies during childhood may be important to prevent increased risk of steroid-related damage in adulthood.
To cite this abstract in AMA style:
Heshin-Bekenstein M, von Scheven E, Hersh AO, Trupin L, Yelin EH, Lawson E. Childhood-Onset Predicts Increased Steroid-Related Damage Among Adults with Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/childhood-onset-predicts-increased-steroid-related-damage-among-adults-with-systemic-lupus-erythematosus/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/childhood-onset-predicts-increased-steroid-related-damage-among-adults-with-systemic-lupus-erythematosus/