Session Information
Date: Thursday, March 30, 2023
Title: Poster Breakout 1 - Lupus: Genetics, Epigenetics, & Social Determinants
Session Type: Breakout Session
Session Time: 5:10PM-5:40PM
Background/Purpose: African-American (AA) ethnicity is a known predisposing factor for childhood onset systemic lupus erythematosus (cSLE) and a predictor of poor outcomes. In addition to race/ethnicity, income and geographical location are known drivers of health care disparities in cSLE. Despite this knowledge, there is lack of literature describing demographic and clinical features of cSLE in a predominantAA cohort. This study aims to characterize demographic and clinical features of cSLE patients in the Southeast United States compared to current literature describing predominantly Caucasian cohorts. The results from this studywill drive future work in comparing outcomes in cSLE and uncovering factors leading to disparities in other regions of the United States.
Methods: This is a cross sectional study of cSLE patients from 2 centers in Southeast United States – University of Mississippi Medical center (UMMC) and University of Alabama at Birmingham (UAB). Prevalent and incident patients with cSLE at UMMC were enrolled after obtaining consent. Demographic, social and clinical data was retrospectively collected by review of the medical charts. Similar data was obtained for the UAB cohort for patients with cSLE via the CARRA registry database. The data from both cohorts was combined and analyzed using SPSS statistical software. Descriptive statistics were used for demographic and clinical features. Unpaired t test and chi square test were used to compare outcomes in this cohort with those reported in the literature.
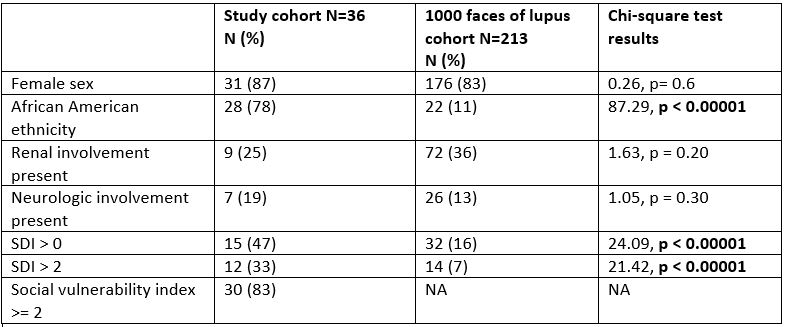
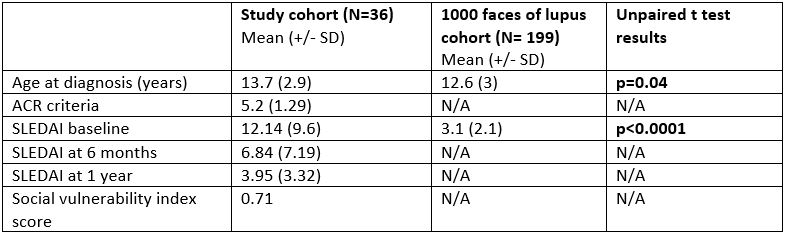
Results: Results are described for a total cohort of 36 patients, comprising 17 from UMMC and 19 from UAB. 31/36 (86.11%) were female, 28/36 (77.78%) were of AA ethnicity, and 23/36 (64%) had Medicaid insurance. Mean age at diagnosis (+/- SD) of SLE for the cohort was 13.7 years (+/- 2.9). Mean ACR score at diagnosis was 5.2 (+/- 1.29), SLICC score was 8.8 (+/- 2.2). Average baseline SLEDAI was 12.14 (+/- 9.6), SLEDAI at 6 months and 1 year respectively was 6.84 and 3.95. Average distance traveled to see a rheumatologist was 74.72 miles compared to a national average of 42.8 miles. 30/36 patients (83.33%) belonged to medium-high or high Social Vulnerability Index group based on zip code. Twenty five percent of patients had some renal involvement. Average SLEDAI compared to a multiethnic Canadian cohort with 10% black population, was significantly higher: 12.14 versus 3.1 (p < 0.00001). 15/36 had SDI > 0 (46.66%) versus 16% reported in the literature (p < 0.0001). 12/36 (33.3%) had SDI >/= 2 compared to 7% reported in the literature (p < 0.0001).
Conclusion: This study described the clinical and socioeconomic characteristics of a predominately AA cSLE population from 2 centers in the Southeastern United States. Compared to multiethnic cohorts of cSLE from Canada, this patient population has significantly higher disease activity and greater damage accrual. Social risk factors for this population include a higher social vulnerability index, longer distance from an academic pediatric rheumatology center, and having Medicaid insurance. The effect of these factors on disparity of disease outcomes needs to be further explored with larger cohorts.
To cite this abstract in AMA style:
Dhanrajani A, Long T, Hagwood S, Johnson L, Karlson C. Characterizing Lupus in African American Children in Southern United States [abstract]. Arthritis Rheumatol. 2023; 75 (suppl 4). https://acrabstracts.org/abstract/characterizing-lupus-in-african-american-children-in-southern-united-states/. Accessed .« Back to 2023 Pediatric Rheumatology Symposium
ACR Meeting Abstracts - https://acrabstracts.org/abstract/characterizing-lupus-in-african-american-children-in-southern-united-states/