Background/Purpose: Central nervous system involvement in Behçet’s disease, usually called neuro-Behçet’s disease (NB), can be classified into acute NB (ANB) and chronic progressive NB (CPNB) based upon the differences in clinical courses and responses to corticosteroid treatment. Previous studies demonstrated that brainstem atrophy was significantly more frequently observed in CPNB than in ANB or non-NB. Noteworthy, in addition to truncal ataxia, neurobehavioral changes are frequently observed in CPNB, which cannot be accounted for by brainstem atrophy. In the present study we examined the volumes of hippocampus in order to determine the responsible lesions for neurobehavioral changes in CPNB.
Methods: A total of 26 patients were studied, including 13 patients with CPNB (11 males and 2 females, age 51.2 ± 12.1 [mean ± SD]) and 13 non-NBD (10 males and 3 females, age 54.4 ± 11.4). All the patients satisfied the international classification criteria for Behçet’s disease. CPNB was defined as intractable, slowly progressive neurobehavioral changes and/or ataxia accompanied by the persistent elevation of cerebrospinal fluid of IL-6 more than 20 pg/mL on two different occasions at intervals of at least 2 weeks (3). The sagittal sections of T1-weighted images on brain MRI were obtained from each patient. Severity of gray matter loss in the hippocampal region and whole brain were investigated by the software for Voxel-Based Specific Regional Analysis System for Alzheimer’s Disease (VSRAD) (Eisai Co., Ltd), calculating the indicators of the degrees of hippocampal region atrophy (HAI) and those of whole-brain atrophy (WBAI). The areas of midbrain tegmentum and pons were measured on mid-sagittal sections of T1-weightened images of brain MRI using image analysis software Image J (NIH, U.S.).
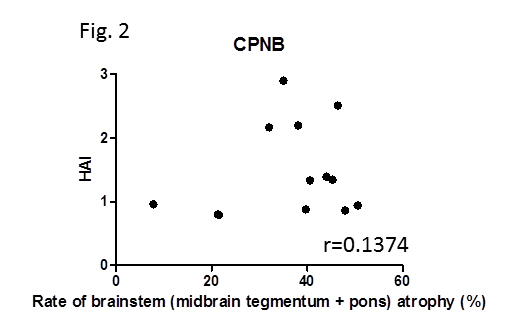
Results: The VSRAD analysis showed that HAI was significantly increased in CPNB (1.46 ± 0.70 [mean ± SD]) compared with in non-NB (0.77 ± 0.40) (p=0.0016) (Fig. 1). Although less markedly, WBAI was significantly higher in CPNB (10.6 ± 5.0) than in non-NB (6.9 ± 1.7) (p=0.0240). Neither HAI nor WBAI was correlated with age. Whereas all the patients with CPNB showed brainstem atrophy, there was no significant correlation between HAI and the rate of brainstem atrophy (Fig. 2).
Conclusion: These results indicate that hippocampus, in addition to brainstem, is a commonly affected lesion in CPNB, accounting for progressive neurobehavioral changes. The lack of correlation between brainstem atrophy and hippocampal atrophy suggest that there might be some predisposing factors determining the preference of affected lesions in CPNB.
Disclosure:
H. Kikuchi,
None;
K. Asako,
None;
M. Takayama,
None;
Y. Kimura,
None;
A. Okamoto,
None;
T. Nanki,
None;
H. Kono,
None;
S. Hirohata,
None.
« Back to 2014 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/atrophy-of-hippocampal-region-in-chronic-progressive-neuro-behcets-disease/