Session Information
Session Type: ACR Abstract Session
Session Time: 4:30PM-6:00PM
Background/Purpose: Recent studies have suggested that peripheral arthritis in patients with spondyloarthritis is associated with HLA-B*15. Studies of white patients with psoriatic arthritis (PsA) have demonstrated associations with HLA-B*27, B*38, B*08 and B*37, whereas B*44 was associated with presence of milder disease. The purpose of this study was to examine HLA-B allele associations with peripheral arthritis and enthesitis in a longitudinal study of outcome in ankylosing spondylitis (AS) where these factors were assessed not only historically but also by systematic clinical assessments.
Methods: This study focused on white patients enrolled in a longitudinal study of outcome in AS. All patients met modified New York Criteria for AS. Study visits were conducted every 4-6 months, and at baseline and every two years a history of peripheral arthritis (and which joints involved), heel pain, plantar fasciitis and Achilles tendonitis. Hip and shoulder involvement was not included in this analysis. Clinical evaluation was carried out by the study rheumatologist at each visit, including joint pain/tenderness/swelling and entheseal involvement by the UCSF Enthesitis Index. HLA-B typing was carried out by single stranded conformational polymorphism (SSCP) analysis. Statistical analyses were carried out by chi square analysis using the EPI-INFO statistical program. In order to control for the high frequency of HLA-B27, relative predispositional effect (RPE) analysis was carried out with HLA-B27 alleles.
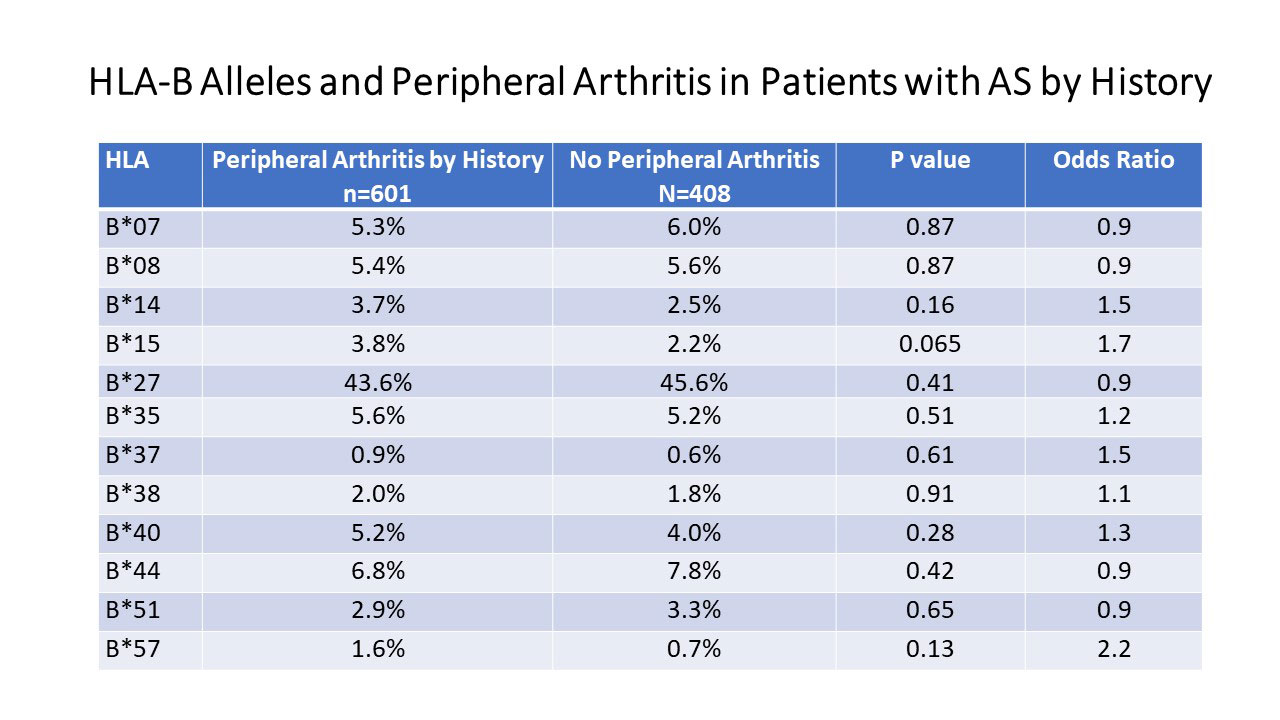
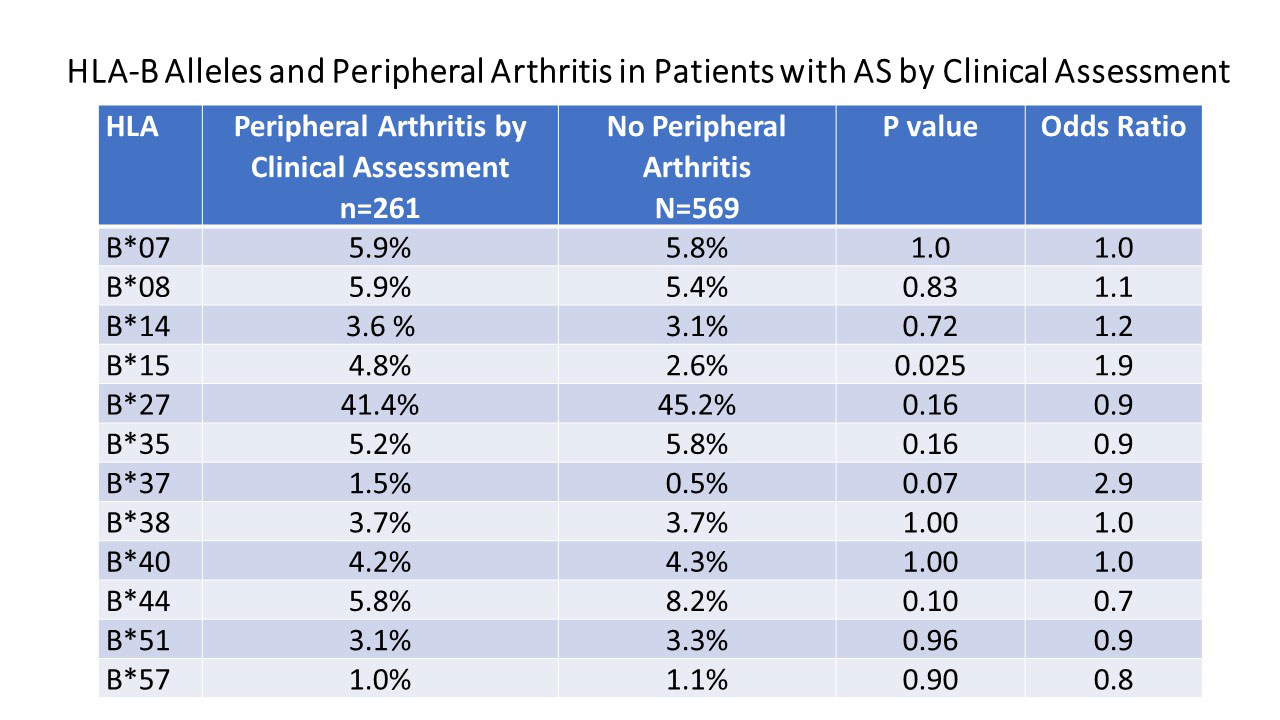
Results: There were 1009 white AS patients with HLA-B typing available included in this analysis. Of these, 158 were seen only once and comprehensive musculoskeletal exam not carried out, though a history of peripheral arthritis, heel pain, plantar fasciitis and Achilles tendonitis attributed to AS recorded. In those patients followed longitudinally, there was an average of 7 study visits conducted. Peripheral arthritis (excluding hips and shoulders) attributed to AS occurred in 64.7% by history. Peripheral arthritis found on clinical evaluation was found in 25.9%. Heel pain by self report occurred in 25.9%, and plantar fascia/Achilles tendon tenderness on clinical evaluation at study visits in 32%. Entheseal tenderness as defined by the UCSF Enthesitis index was observed at least once in 65.5%. No HLA-B associations were encountered with heel pain, plantar fasciitis, Achilles tendonitis by history or plantar/Achilles tendon tenderness. Neither were any associations were observed on the UCSF Enthesitis index or with peripheral arthritis by patient history. HLA-B*15 was increased in frequency in those with peripheral arthritis seen on clinical evaluation (Table 2), which was confirmed on RPE analysis, where a weak negative association with HLA-B*44 was also observed (9.8 vs. 14.9%, p=0.04, OR=0.6).
Conclusion: These data in a large cohort of patients with AS confirms the association of HLA-B*15 with peripheral joint involvement in AS. The HLA-B associations with peripheral joint and entheseal involvement previously reported in PsA are not confirmed in AS suggesting that different mechanisms may be in play in the pathogenesis of peripheral joint and entheseal involvement between AS and psoriatic arthritis.
To cite this abstract in AMA style:
Naovarat B, Weisman M, Gensler L, Ward M, Hwang M, Tahanan A, Lee M, Rahbar M, Ishimori M, Brown M, Reveille J. Associations of HLA-B Alleles, Enthesitis and Peripheral Arthritis in Ankylosing Spondylitis [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/associations-of-hla-b-alleles-enthesitis-and-peripheral-arthritis-in-ankylosing-spondylitis/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/associations-of-hla-b-alleles-enthesitis-and-peripheral-arthritis-in-ankylosing-spondylitis/