Session Information
Date: Monday, November 11, 2019
Title: Epidemiology & Public Health Poster II: Spondyloarthritis & Connective Tissue Disease
Session Type: Poster Session (Monday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Chronic systemic inflammation generated by rheumatic diseases (RD) is related to the increased cardiovascular risk (CVR) in this population. However, the coexistence of traditional CVR factors such as diabetes, hypertension, obesity, smoking, and dyslipidemia, further increases CVR burden. Through an adequate control of this factors, CVR can be decreased. But to achieve this, primary care physicians and rheumatologists should be aware of how relevant it is to make frequent cardiovascular assessment to RD patients. Therefore, the aim of this study is to determine the prevalence of underdiagnosis and inefficient treatment of traditional cardiovascular risk factors in RD patients.
Methods: An observational, retrospective study of patients between 30 and 75 years with rheumatoid arthritis, psoriatic arthritis, systemic lupus erythematosus and ankylosing spondylitis. Patient information was obtained from March 2018 to April 2019 through the REPAIR® software, an electronic records database used at the rheumatology clinic at a University Hospital in northeastern Mexico. Exclusion criteria: previous atherosclerotic cardiovascular disease, overlap syndromes, diabetes, or pregnancy. Evaluation included history of lifestyle, comorbidities, use of corticoids, blood pressure, anthropometry and fasting glucose measures. Framingham-Body Mass Index (FRS-BMI) was used to calculate their predicted CVR to 10 years.
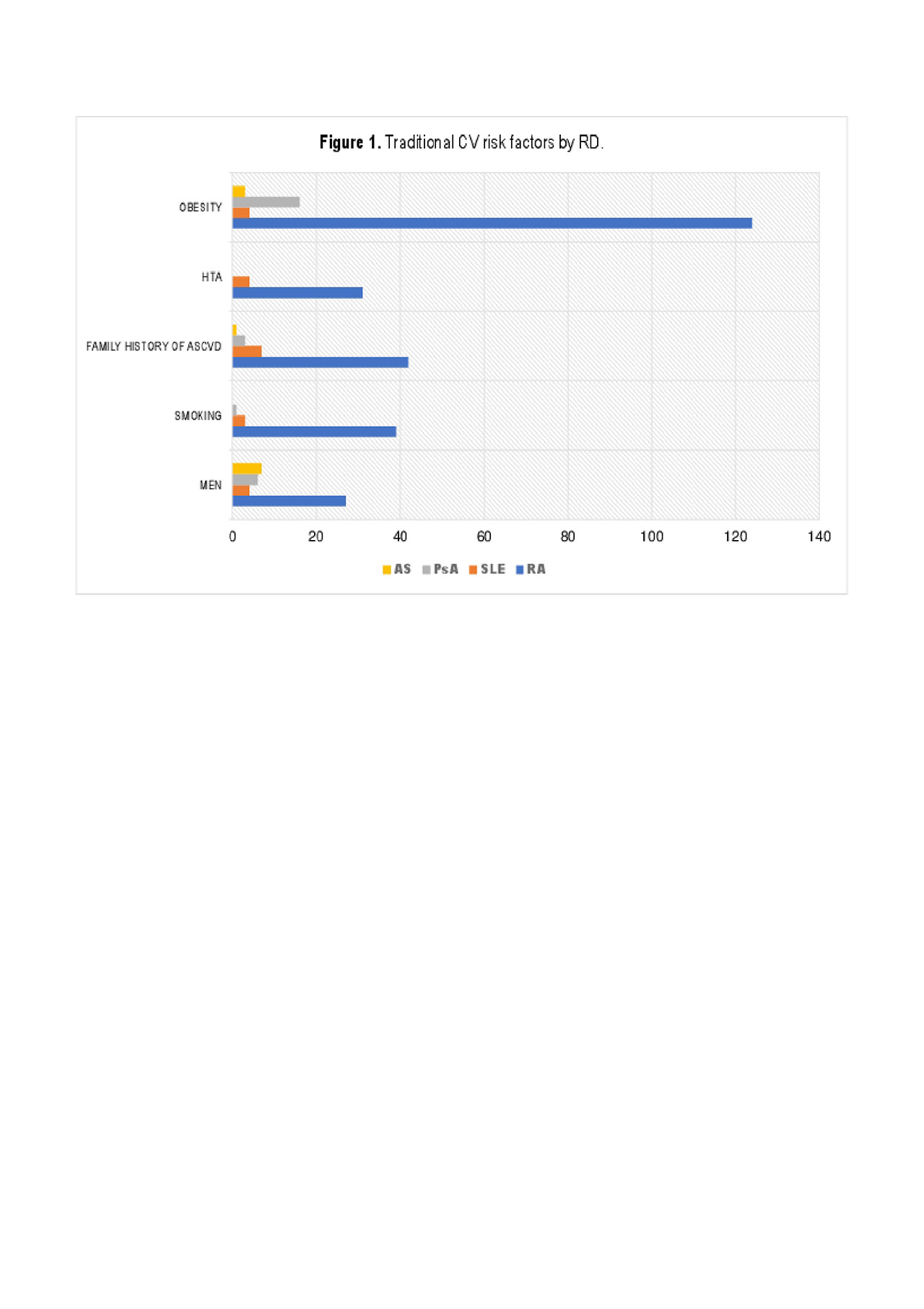
Results: A total of 451 patients were recruited, 90.2% were women, with a median age of 52 years (43-59). In this population, 80.2% of the patients had at least one CVR factor; the presence of traditional CVR factors according to RD is shown in Figure 1. Other population characteristics are in Table 1. More than half of the patients were not in their ideal weight, 37.2% being diagnosed as overweight and 32.8% with obesity. Out of the patients with no previous diagnosis of hypertension (n=416, 92.2%), 25.96% had elevated or high blood pressure levels. From the patients that previously had hypertension, 65.7% did not have an adequate control of their blood pressure, even though they were on pharmacological treatment. History of dyslipidemia was found in 4.9% of patients. Half of them arrived at consultation with a recent lipid profile, having a median LDL of 133.5 (109-158) mg/dL, not meeting target levels. Even though no diabetic patients were included, 22.8% of the patients had hyperglycemia. According to FRS-BMI, 82% of the patients had a low CVR, 13.7% moderate risk, and 4.2% had a high CVR.
Conclusion: This study suggests that traditional CVR factors are underdiagnosed and insufficiently treated in RD patients. The previous is alarming, because 80.2% of the patients have at least one CVR factor, and they could highly benefit from its adequate control. Besides having a RD and at least one traditional CVR factor, 17.9% of the patients had a moderate or high CVR according to FRS-BMI. Rheumatologists should become more aware of the increased CVR in RD patients, and make CV assessment a part of their routine.
To cite this abstract in AMA style:
Galarza-Delgado D, Azpiri-Lopez J, Colunga-Pedraza I, Hernández-Galarza I, Reynosa-Silva I, Cuellar-Calderon K, Castro-Gonzalez M, Martinez-Flores C. Are Rheumatologists Correctly Identifying and Controlling Traditional Cardiovascular Risk Factors? [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/are-rheumatologists-correctly-identifying-and-controlling-traditional-cardiovascular-risk-factors/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/are-rheumatologists-correctly-identifying-and-controlling-traditional-cardiovascular-risk-factors/