Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose : There is a need to standardize platelet-rich plasma (PRP)-derived products and their dosage to evaluate efficacy for each intended indication. Our purpose here was to test the anti-inflammatory effects of PRP releasates (PRP-rs) from PRP with standardized (absolute) platelet concentrations in OA knee and hip chondrocytes stimulated with IL-1B.
Methods : Blood was obtained from healthy volunteers after informed consent. PRPs with different platelet concentrations (0, 0.25, 0.5, 0.75, 1.5, 3, 6 and 15x105platelets/uL) were prepared by first, separating platelets and platelet poor plasma (PPP), and then re-suspending platelets in known absolute numbers. PRPs were then clotted with CaCl2 to obtain their PRP-rs. Human chondrocytes (hCH) were isolated from OA hip and knee joints after informed consent. Co-stimulation of hCH with IL-1B and the different PRP-rs (10% in DMEM) was used to test their anti-inflammatory effect. We assessed the expression of relevant inflammatory markers with qRT-PCR, ELISA and immunocytochemistry. GraphPad Prism software was used for data analysis with both parametric (ANOVA + BonferroniÕs post hoc test) and non-parametric (Kruskal-Wallis + DunnÕs test) approaches.
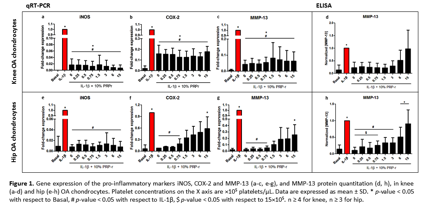
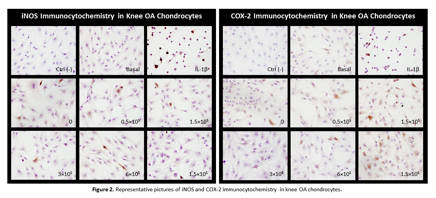
Results : Inflammatory stimulation with IL-1B sharply increased the expression of iNOS, COX-2, PTGES, MMP-13 and IL-6. All PRP-rs showed a significant anti-inflammatory effect in knee OA hCH for all markers, ranging from 80% for COX_2 to 99% for iNOS (Fig.1a-c). Remarkably, this reduction was not dependent on platelet dose; even PPP showed maximum anti-inflammatory effect. As for hip OA hCH, only the lower platelet doses of 0 – 0.75×105/uL reduced the expression of COX-2 (~90%), PTGES and MMP-13 (~90%) significantly (Fig.1f-g). Increasing platelet doses (except for iNOS, Fig.1e) resulted in a progressive loss of this anti-inflammatory effect in hip OA hCH. ELISA quantitation of MMP-13 protein corroborated these trends on knee and hip hCH: all PRP_rs (except 6 and 15×105/uL) reduced MMP-13 to approximately basal levels (Fig 1d, h). Immunocytochemistry of iNOS and COX-2 in knee hCH were concordant with qRT-PCR results as well (Fig 2).
Conclusion : PRP-r can exert anti-inflammatory effects in OA hCH but platelet enrichment is not needed for knee OA hCH, and it is detrimental in hip OA. In this case, only doses below peripheral blood platelet concentration (< 1.5×105platelet/uL) were effective. Therefore, platelet dosages in PRP need to be standardized to evaluate efficacy and might need to be adjusted for different indications.
To cite this abstract in AMA style:
Gato-Calvo L, Vela-Anero Á, Burguera EF, Blanco FJ. Anti-Inflammatory Effects of Standardized Platelet-Rich Plasma Releasates in Knee and Hip OA Chondrocytes [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/anti-inflammatory-effects-of-standardized-platelet-rich-plasma-releasates-in-knee-and-hip-oa-chondrocytes/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/anti-inflammatory-effects-of-standardized-platelet-rich-plasma-releasates-in-knee-and-hip-oa-chondrocytes/