Session Information
Session Type: Poster Session A
Session Time: 9:00AM-11:00AM
Background/Purpose: ANCA-associated vasculitis (AAV) is often studied in the Caucasian population with few studies looking at the disease in other races. Disease presentation and treatment implications of autoimmune conditions vary by ethnicity, as seen in systemic lupus erythematous. A 2014 study of the Chicago area compared AAV in Hispanic and Caucasian patients and found increased disease severity, as defined by the Birmingham Vasculitis Activity Score (BVAS) and the Vasculitis Disease Index (VDI), with greater renal involvement in Hispanics. We performed a similar study examining the differences in AAV in the Hispanic and Caucasian populations living in the Inland Empire region of Southern California.
Methods: A retrospective study was conducted on data extracted from the Loma Linda University Medical Center and the Riverside University Health System’s Electronic Medical Record, using ICD 9 and ICD 10 CM codes pertaining to vasculitis. Data span the dates of January 1, 2003 to December 31, 2019. Vasculitis cases were classified using the Diagnostic and Classification of the Systemic Vasculitis (DCVAS). Data extracted from the electronic charts include demographics, ICU admission due to vasculitis flare, presence of chronic kidney disease or end stage renal disease (ESRD), BVAS on presentation and VDI as detailed on recent clinic visit. We calculated odds ratios for the categorical data and ran Independent sample T-test for the continuous data with alpha equal to 0.05 for statistical significance.
Results: 129 charts were included in the analysis with 66 Hispanics and 63 Caucasians (see table 1). 72 cases of Granulomatosis Polyangiitis (GPA), 47 cases of Microscopic Polyangiitis (MPA) and 10 cases of Eosinophilic Granulomatosis Polyangiitis (EGPA) were identified. Hispanics had a 49% increase in odds of being admitted to the ICU secondary to vasculitis when compared to Caucasians [OR 1.49 (95% CI 0.72, 3.07)]. Hispanics were noted to have more flares with a maximum recorded number of flares for a single patient to be 15 compared to 7 for a Caucasian patient. They also had a 71% increase in odds of having kidney disease in comparison to Caucasians [OR 1.71 (95% CI 0.85, 3.43)]. Of the patients with kidney disease, Hispanics had a 95% increase in odds of having ESRD when compared to Caucasians [OR 1.95 (95% CI 0.68, 5.55)]. See table 2. The BVAS and VDI averages between Hispanics and Caucasians were comparable at 8.53 ± 7.3 vs 7.69 ± 6.3 and 2.32 ± 2.0 vs 2.2 ± 1.5, respectively (p = 0.49; p = 0.70). See table 3. Although we observed differences in disease severity proportions between Hispanics and Caucasians, the measures of association were not statistically significant.
Conclusion: Like the Chicago study, we saw greater incidences of renal disease and increased severity in Hispanics compared to Caucasians, as defined by increased rates of ICU admissions and vasculitis flares, despite analogous average BVAS and VDI scores. Our data shows that conventionally used disease activity scores may not convey the seriousness of renal or pulmonary vasculitis in Hispanic populations. Clinicians treating Hispanic patients with AAV should have a high index of suspicion for more severe disease in this patient population when compared to Caucasians.
 Table 1. Observed Attributes of Hispanic and Caucasian patients with ANCA-associated Vasculitis.
Table 1. Observed Attributes of Hispanic and Caucasian patients with ANCA-associated Vasculitis.
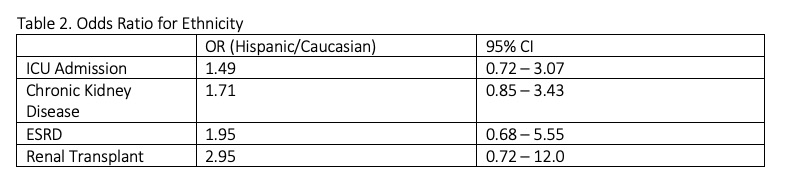 Table 2. Odds Ratio for Ethnicity
Table 2. Odds Ratio for Ethnicity
 Table 3. Independent Sample T-test of BVAS and VDI.
Table 3. Independent Sample T-test of BVAS and VDI.
To cite this abstract in AMA style:
Lee S, Injean P, Tran P, Panikkath D, Downey C. ANCA-associated Vasculitis in Caucasian and Hispanics of the Inland Empire of Southern California [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/anca-associated-vasculitis-in-caucasian-and-hispanics-of-the-inland-empire-of-southern-california/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/anca-associated-vasculitis-in-caucasian-and-hispanics-of-the-inland-empire-of-southern-california/
