Session Information
Date: Monday, November 9, 2015
Title: Education Poster I
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose:
Internal medicine (IM) trainees should be proficient in rheumatologic knowledge and skills. Our prior data show that a curriculum including an attending-led multimodal simulation training session (MSTS) improves residents’ self-confidence in rheumatologic history, physical exam, procedures, and patient care. This academic year, we elected to have the second year rheumatology fellows lead the MSTS. To assess effectiveness, we conducted pre/post self-assessment surveys of residents completing the rheumatology curriculum and compared them to the prior year.
Methods:
All Post Graduate Year 1(PGY 1) IM residents rotating on the ambulatory rheumatology block during the 2014 and 2015 academic years participated in a two-part training session. Residents performed a rheumatologic history and exam on a standardized patient presenting with knee pain and practiced knee joint aspiration with a mannequin. In 2015, second year rheumatology fellows completed a six session teaching training period. After this training, fellows directed the MSTS program for PGY1 trainees.
All PGY 1 residents completed an online, self-assessment survey on self-confidence (0=not confident, 100=extremely confident) in performing a rheumatologic history, physical examination, common procedures, and interpreting rheumatologic lab tests pre/post their rheumatology block in addition to a MSTS evaluation. We compared the pre/post survey results in residents’ self-assessed confidence from the 2014 and 2015 academic years using the Wilcoxon signed-rank test. The Institutional Review Board approved the study.
Results:
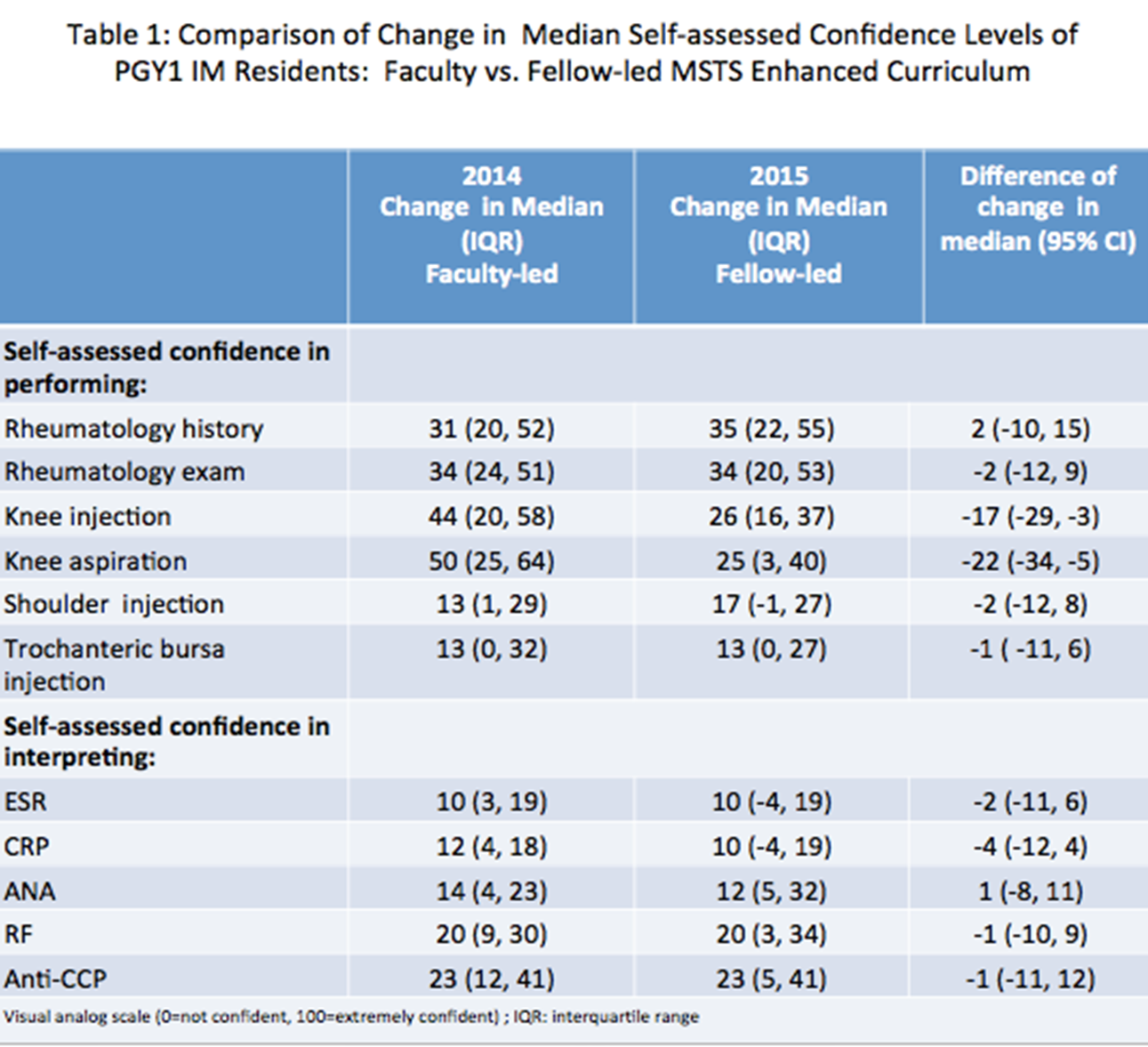
A total of 40/44 (91%) and 25/29 (86%) PGY1 trainees from 2014 and 2015 respectively completed the pre/post-surveys. Both cohorts increased their self-assessed confidence ratings from pre to post in all variables (Table 1). There was no significant difference in improved self-confidence levels on pre/post rotation in performing a rheumatologic history or exam and in interpreting common rheumatologic labs. However, compared to the 2015 fellow-taught cohort, the 2014 faculty-taught cohort had a significantly higher improvement in median self–assessed confidence in performing knee injection [median 44; IQR (20-57.5) vs. 26; IQR (16-37)] and knee aspiration [median 50, IQR (25-64) vs. 25; IQR( 3-40)] (Table 1). In both cohorts, over 98% of PGY1 IM residents strongly agreed or agreed that the MSTS was a valuable training exercise.
Conclusion:
Our results indicate that the fellow-led MSTS enhanced curriculum is as effective as an attending-led MSTS enhanced curriculum in improving residents’ self-confidence in performing a rheumatologic history and exam, but not in knee aspiration and injection. These results suggest that a fellow-led MSTS program can be effective, however, alternative methods for training fellows to teach joint injections and aspirations should be investigated.
To cite this abstract in AMA style:
Zaha OE, Harwell SA, Chung CP, Davidson MA, Johnstone DA, Skaug LA, Dewey CM, Kroop SF. Ambulatory Rheumatology Curriculum: Effect of Fellow Teaching Multimodal Simulation Curriculum Enhancement [abstract]. Arthritis Rheumatol. 2015; 67 (suppl 10). https://acrabstracts.org/abstract/ambulatory-rheumatology-curriculum-effect-of-fellow-teaching-multimodal-simulation-curriculum-enhancement/. Accessed .« Back to 2015 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/ambulatory-rheumatology-curriculum-effect-of-fellow-teaching-multimodal-simulation-curriculum-enhancement/