Session Information
Date: Wednesday, November 13, 2019
Title: 6W011: RA – Diagnosis, Manifestations, & Outcomes V: Treatment (2870–2875)
Session Type: ACR Abstract Session
Session Time: 9:00AM-10:30AM
Background/Purpose: The last 25 years, treatment of rheumatoid arthritis (RA) has changed considerably. Although clinically relevant joint damage has become infrequent, it is less established to what extent other long-term outcomes have improved. Moreover, anti-citrullinated anti-bodies (ACPA)-positive and ACPA-negative disease subsets were discovered and it is unknown they have benefited equally from these improvements. Therefore our aim was to investigate the influence of improved treatment strategies on disease activity (DAS), sustained drug-free remission (SDFR) and functional disability, and if this differed for ACPA-positive and ACPA-negative RA-patients.
Methods: In the Leiden early arthritis cohort, consecutive patients with RA (1987 criteria) were included between 1993-2016. Patients were treated in routine care; initial and subsequent treatment changed over time; divided in 5 inclusion periods: 1993-1996 delayed mild disease modifying anti-rheumatic drug (DMARD) initiation; 1997-2000 early mild DMARDs; 2001-2005 early methotrexate; 2006-2010 early methotrexate followed by treat-to-target treatment adjustments; 2011-2016 idem plus additional efforts for very early referral.
SDFR was defined as persistent absence of synovitis after DMARD-cessation and was determined during all follow-up. Disease activity was measured yearly by the DAS28-ESR and functional disability by health assessment questionnaires (HAQ) and analysed with linear mixed models; time to SDFR with Cox regression. Analyses were stratified for ACPA (IgG anti-CCP2).
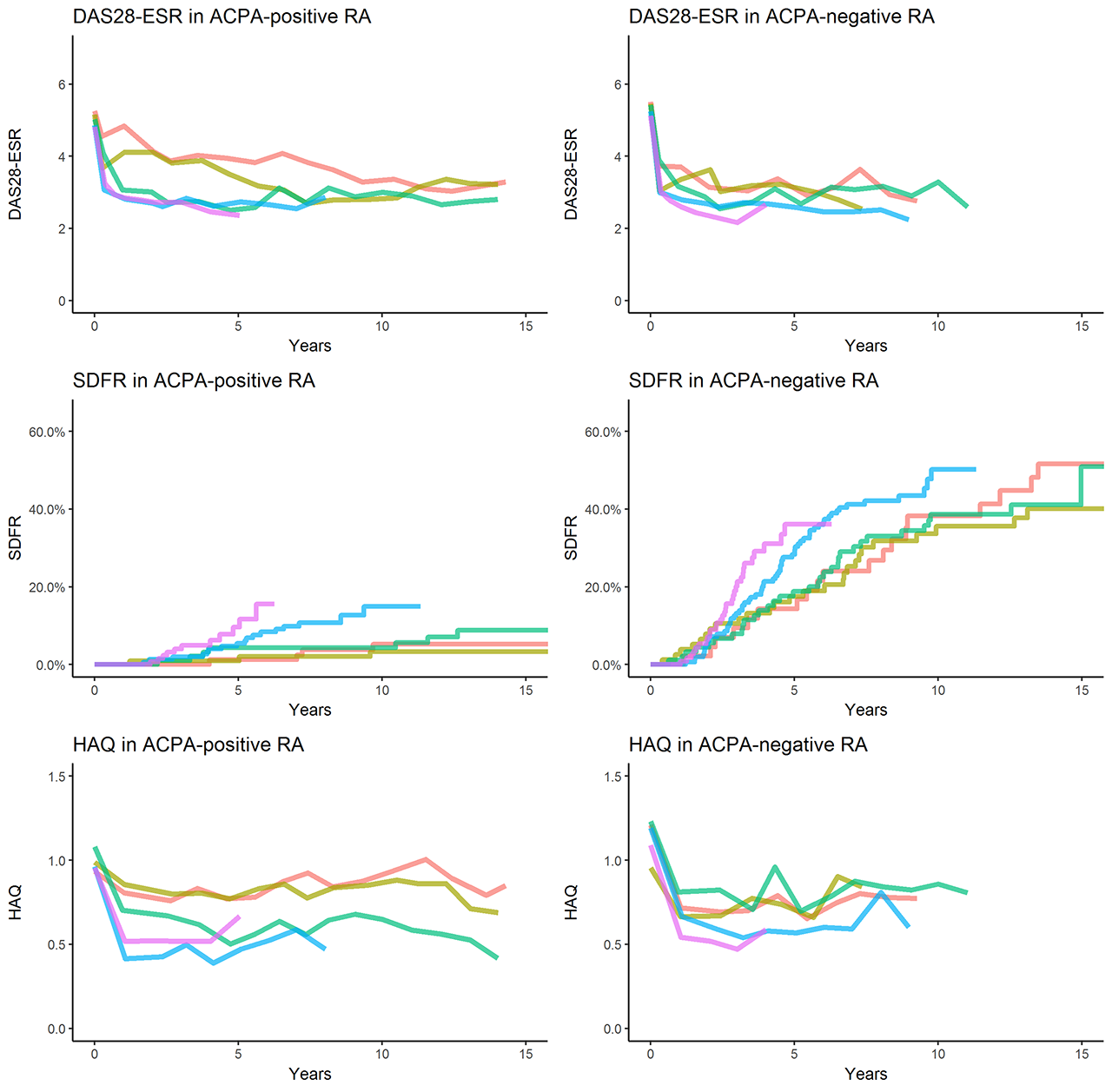
Results: In total 1291 RA-patients were included (168, 185, 210, 338 and 390 in the respective inclusion periods); baseline age, gender and ACPA-status were similar. All outcomes improved significantly over time (Figure 1) and this differed between ACPA-positive and ACPA-negative patients (Figure 2). In the reference period (1993-1996), ACPA-positive RA had worse outcomes than ACPA-negative RA in DAS (Difference of 0.81 points (0.48;1.13)), SDFR (HR 0.07 (0.02;0.21)) and HAQ over time (Difference of 0.15 points (-0.02;0.32)). Compared to the reference period, DAS improved gradually and significantly in ACPA-positive RA whereas the improvement was significantly less in ACPA-negative RA. SDFR-rates increased significantly in ACPA-positive RA, whereas there was no significant improvement in ACPA-negative RA. Functional disability over time improved more in ACPA-positive RA (improvement of -0.18 points in 2001-2005, -0.35 in 2006-2010 and -0.29 in 2011-2016) than in ACPA-negative RA (improvement of -0.19 in 2011-2016). In the most recent inclusion cohort (2011-2016), HAQ was similar in ACPA-positive and ACPA-negative RA. SDFR rates had become more similar although they remained higher in ACPA-negative RA.
Conclusion: ACPA-positive RA, traditionally the most severe RA-subset, benefited most from the improvements in treatment strategies, whereas ACPA-negative RA benefited little; This further demonstrates that these are indeed separate disease subsets that deserve equal attention.
Legend: For DAS28-ESR and HAQ mean values of imputed data from visits that were attended are shown; When <15% of patients attended the visit, lines were truncated.
Legend: Inclusion periods: Red: 1993-1996; Yellow: 1997-2000, Green 2001-2005, Blue 2006-2010, Purple 2011-2016. RA: Rheumatoid Arthritis; SDFR: Sustained drug-free remission. For DAS28-ESR and HAQ mean values of imputed data from visits that were attended are shown; When <15% of patients attended the visit, lines were truncated.
To cite this abstract in AMA style:
Matthijssen X, Niemantsverdriet E, Huizinga T, van der Helm-van Mil A. Advances in Treatment of Rheumatoid Arthritis: ACPA-positive Patients Benefited More Than ACPA-negative Patients; 25 Year Results of a Longitudinal Cohort Study [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/advances-in-treatment-of-rheumatoid-arthritis-acpa-positive-patients-benefited-more-than-acpa-negative-patients-25-year-results-of-a-longitudinal-cohort-study/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/advances-in-treatment-of-rheumatoid-arthritis-acpa-positive-patients-benefited-more-than-acpa-negative-patients-25-year-results-of-a-longitudinal-cohort-study/