Session Information
Date: Tuesday, November 9, 2021
Title: RA – Treatments Poster III: RA Treatments & Their Safety (1674–1710)
Session Type: Poster Session D
Session Time: 8:30AM-10:30AM
Background/Purpose: Interstitial lung disease (ILD) is a severe complication of Rheumatoid Arthritis (RA). Usual interstitial pneumonia (UIP) is considered to be more frequent and severe in RA than non-specific interstitial pneumonia (NSIP). Abatacept (ABA) and Rituximab have demonstrated efficacy in RA-ILD [Fernández-Díaz C, et al. Semin Arthritis Rheum. 2018 Aug;48(1):22-27; Fernández-Díaz C, et al. Rheumatology (Oxford). 2020 Dec 1;59(12):3906-16; Atienza-Mateo B, et al. J Clin Med. 2020 Sep 23;9(10):3070]. Our aim was to compare the efficacy of ABA in RA-ILD patients according to radiological patterns of UIP or NSIP.
Methods: From an observational multicenter study of 263 RA-ILD patients treated with ABA, we selected those with UIP or NSIP. We analyzed in the 2 groups from baseline up to 24 months the following outcomes: a) Forced Vital Capacity (FVC), b) Carbon monoxide diffusing capacity (DLCO), c) Chest High Resolution Computed Tomography (HRCT), and d) dyspnea. Differences between final follow-up and basal visit were calculated as the average difference and 95% Confidence Interval (95% CI). Multivariable linear regression was used to assess the differences between the 2 groups.
Results: We studied 190 patients with UIP (n=106) and NSIP (n=84). Patients with UIP were older, had more positivity for rheumatoid factor and had received more sulfasalazine (Table 1). ILD duration up to ABA initiation was relatively short in both groups, with a median [IQR] of 16 [4-50] and 11 [2-36] months in UIP and NSIP patterns, respectively. Mean baseline values of FVC and DLCO were > 80% and > 60%, respectively, in the 2 groups, with a lower FVC in UIP (82% vs 89% in NSIP, p< 0.05). The evolution of FVC and DLCO is shown in Figure 1. Both parameters remained stable during 24 months of ABA therapy. Available chest HRCT images improved/ stabilized in 73.1% and 72.9% of UIP and NSIP patterns, respectively. With multivariable linear regression analysis, no differences were found in the changes of FVC, DLCO, or HRCT images. Stabilization or improvement of dyspnea was found in 91% and 95% of UIP and NSIP patterns, respectively.
Conclusion: ABA seems to be equally effective in stabilizing of DLCO, FVC and HRCT in UIP and NSIP in RA-ILD. Our results suggest that an early administration of ABA in ILD, before significant structural lung damage development, may be preferable to prevent interstitial progression, regardless of the radiological pattern.
 Table 1. Main general features at baseline. ABA, abatacept; ACPA, anti-citrullinated protein antibodies; DMARD, disease-modifying antirheumatic drug, ILD, Interstitial lung disease; MTX, methotrexate; NSIP, non-specific interstitial pneumonia; RA, rheumatoid arthritis; TNF, tumor necrosis factor; UIP, usual interstitial pneumonia.
Table 1. Main general features at baseline. ABA, abatacept; ACPA, anti-citrullinated protein antibodies; DMARD, disease-modifying antirheumatic drug, ILD, Interstitial lung disease; MTX, methotrexate; NSIP, non-specific interstitial pneumonia; RA, rheumatoid arthritis; TNF, tumor necrosis factor; UIP, usual interstitial pneumonia.
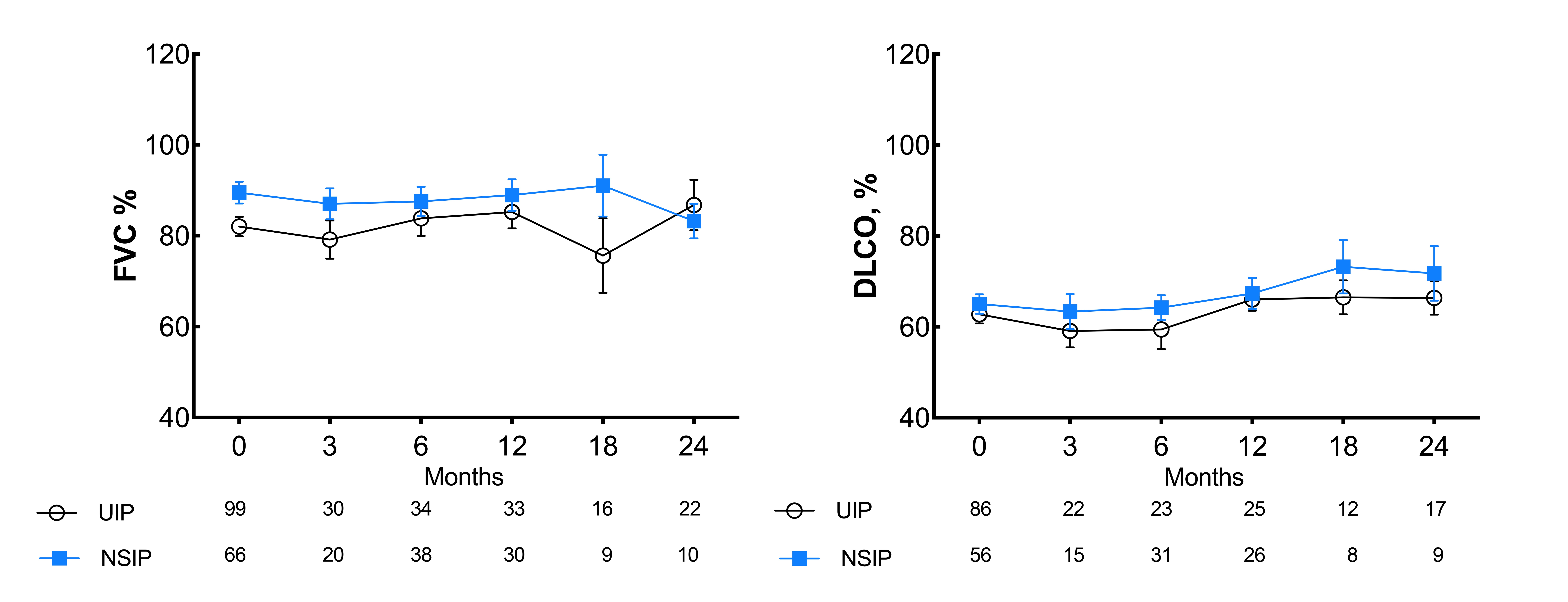 Figure 1. Evolution of pulmonary function tests in RA-ILD patients with UIP and NSIP patterns. FVC and DLCO are expressed as mean (95%CI) and compared between the 2 groups.
Figure 1. Evolution of pulmonary function tests in RA-ILD patients with UIP and NSIP patterns. FVC and DLCO are expressed as mean (95%CI) and compared between the 2 groups.
To cite this abstract in AMA style:
Atienza-Mateo B, Fernández-Díaz C, Castañeda S, Melero R, Ortiz-Sanjuán F, Casafont I, Rodríguez-García S, Ferraz-Amaro I, gonzalez-Gay M, Blanco R. Abatacept in Usual and in Non-Specific Interstitial Pneumonia Associated to Rheumatoid Arthritis. National Multicenter Study of 190 Patients [abstract]. Arthritis Rheumatol. 2021; 73 (suppl 9). https://acrabstracts.org/abstract/abatacept-in-usual-and-in-non-specific-interstitial-pneumonia-associated-to-rheumatoid-arthritis-national-multicenter-study-of-190-patients/. Accessed .« Back to ACR Convergence 2021
ACR Meeting Abstracts - https://acrabstracts.org/abstract/abatacept-in-usual-and-in-non-specific-interstitial-pneumonia-associated-to-rheumatoid-arthritis-national-multicenter-study-of-190-patients/
