Session Information
Session Type: ACR Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose:
APS ACTION
International Clinical Database and Repository was created to study the natural
course of persistently antiphospholipid antibodies (aPL)-positive patients ± autoimmune
disorders over 10 years. Cluster analysis (CA) is a data driven method that can
group patients in a way that patients in the same group (cluster) are more
similar to each other than to those in other groups. Previously, we identified three
different clinical phenotypes of aPL-positive patients discriminated by aPL
profile, lupus, or cardiovascular (CV) risk factors (Ann Rheum Dis 2015;74(S2):813-4). As
a follow-up analysis, our objective was to analyze different clinical
phenotypes among female patients with a special focus on obstetric manifestations.
Methods: A
secure web-based data capture system is used to store patient demographics,
pertinent aPL history, and aPL profile.
The inclusion criteria include aPL positivity according to updated Sapporo APS
Classification Criteria. CA, using Ward’s minimum-variance
hierarchical method, was performed on the baseline characteristics; 15 clinical
data points were included in the CA to cover a broad spectrum of aPL-positive
patients. To identify differences between clusters, ANOVA and χ2
test of independence were used with adjustment using the Bonferroni correction
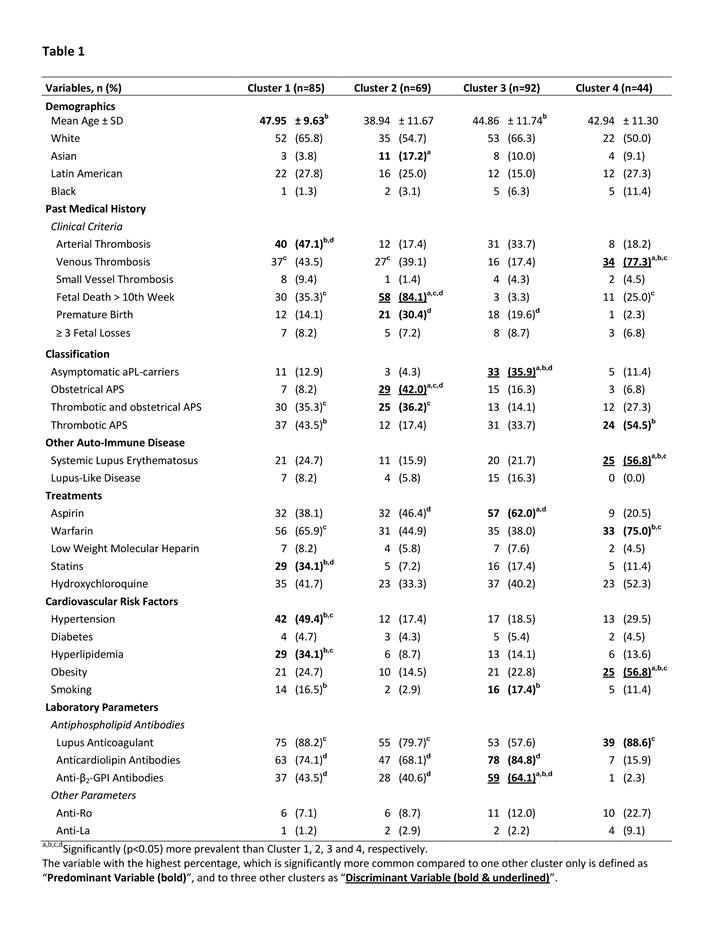
to identify predominant and discriminant variables (Table).
Results:
As of June 2015, of
573 aPL-positive patients recruited from 24 centers, 283 were excluded (139
male, 130 without history of pregnancy, and 14 with missing data). Finally, 290
female patients with a history of at least one pregnancy were included. Four main
exclusive clusters with different combinations of features were (Table): a)
Cluster 1: older female patients with arterial thrombosis and CV risk
factors; b) Cluster 2: female patients with pregnancy morbidity only; c)
Cluster 3: asymptomatic aPL-positive female patients with aCL/antiβ2GPI antibodies treated with aspirin;
and c) Cluster 4: female patients with venous thrombosis obesity, SLE, lupus
anticoagulant, and treated with warfarin.
Conclusion: Our CA identified four different
clinical phenotypes of aPL-positive female patients discriminated by pregnancy
morbidity, CV risk factors, aPL profile, and lupus. Our results: a) support the
heterogeneity of aPL-positive patients; and b) provide a foundation to
understand disease mechanisms, create new approaches for APS classification,
and ultimately to develop new management approaches.
To cite this abstract in AMA style:
Zuily S, Chighizola CB, WAHL D, Meroni PL, Erkan D. Antiphospholipid Syndrome Alliance for Clinical Trials and International Networking Clinical Database and Repository Cluster Analysis: Identification of Different Clinical Phenotypes Among Antiphospholipid Antibody-Positive Female Patients [abstract]. Arthritis Rheumatol. 2015; 67 (suppl 10). https://acrabstracts.org/abstract/antiphospholipid-syndrome-alliance-for-clinical-trials-and-international-networking-clinical-database-and-repository-cluster-analysis-identification-of-different-clinical-phenotypes-among-antiphospho/. Accessed .« Back to 2015 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/antiphospholipid-syndrome-alliance-for-clinical-trials-and-international-networking-clinical-database-and-repository-cluster-analysis-identification-of-different-clinical-phenotypes-among-antiphospho/