Session Information
Date: Monday, November 14, 2016
Title: Rheumatoid Arthritis – Clinical Aspects - Poster II: Co-morbidities and Complications
Session Type: ACR Poster Session B
Session Time: 9:00AM-11:00AM
Background/Purpose: Lower serum vitamin D levels have been shown to be associated with various autoimmune disorders including Rheumatoid Arthritis (RA). We undertook this study to evaluate vitamin D status and assess the relationship if any between vitamin D levels and disease activity and disability in patients with RA.
Methods: A total of 100 adult patients (82 females, 18 males) of RA (ACR/EULAR-2010 criteria) presenting to Rheumatology department and 50 healthy controls drawn from hospital staff matched for age and gender (42 female, 8 male) were enrolled. Exclusion criteria comprised severe hepatic, and/or renal disease, uncontrolled diabetes, granulomatous disease. Disease activity and disability was evaluated by DAS28(ESR) and Indian HAQ disability index (HAQ-DI) respectively. Serum total 25(OH)D3 levels were measured by electrochemiluminescence assay. Vitamin D insufficiency was defined as <30 ng/ml. Unpaired t-tests, chi square, ANOVA, Kruskal Wallis, Pearson and multivariate regression were applied as appropriate.
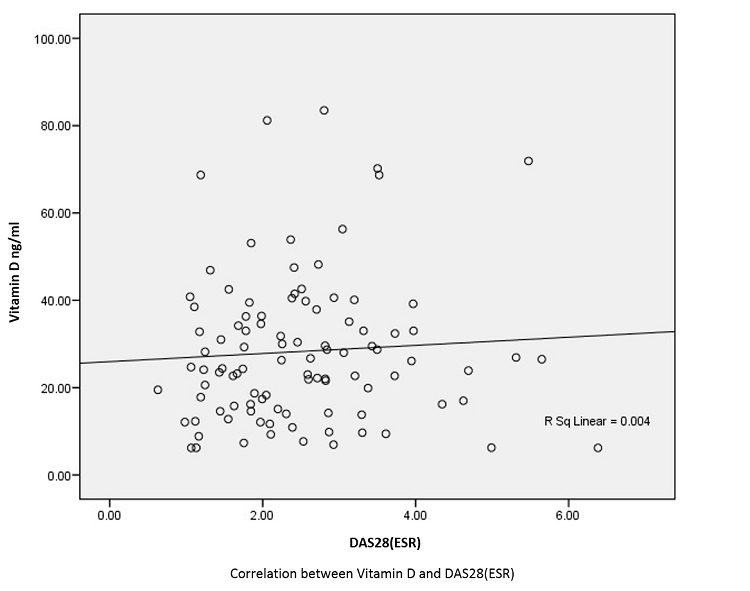
Results: The mean 25(OH)D3 levels in cases and controls were 28.29±16.67 and 15.59±10.58 ng/ml respectively (p-value=0.000). As many as 62% of the patients and 88% (44/50) of the controls had vitamin D insufficiency (p-value<0.001). Mean serum vitamin D levels were significantly higher in patients who were on high dose (oral 60,000 IU/week or injection within last 6 months) of vitamin D supplementation (40%) (39.55±17.00 ng/ml) (p-value<0.001) compared to that of those who had received either none (23%), 250 IU/day (23%) or 500 IU/day (14%). Vitamin D levels were not significantly different in patients who were in remission, low, moderate and high disease activity (27.05±15.05, 32.44±18.52, 27.49±17.30 and 32.88±27.75 ng/ml respectively, p-value=0.709). No significant correlation was seen between mean vitamin D levels and age, BMI, SJC, TJC, ESR, General Health (GH), DAS28(ESR), HAQ-DI and serum PTH. Only duration of illness was positively correlated with vitamin D level (r=0.212, p-value=0.035). Vitamin D levels were also not different with regard to gender, menopause, deformity, hypothyroidism, RF, anti CCP status and current glucocorticoid use. On multivariate analysis, vitamin D levels were not related to various disease activity and disability variables [SJC, TJC, ESR, GH, DAS28(ESR) and HAQ-DI].
Conclusion: Vitamin D insufficiency was widespread both in patients with RA (62%) and in hospital staff without any disease (88%). No correlation was found between mean 25(OH)D3 levels and disease activity, disability and other variables. Longer disease duration of RA was associated with higher vitamin D levels. This could be because of greater use of vitamin D supplements by patients with long standing disease. The healthy hospital staff had low vitamin D possibly due to greater time spent indoors.
To cite this abstract in AMA style:
Vaishnav B, Meghnathi B, Patil A, Upadhyaya S, Gupta SJ, Handa R. Vitamin D Insufficiency in Patients with Rheumatoid Arthritis and Healthy Controls and Correlation Between Vitamin D Levels and Disease Activity and Disability in RA Patients [abstract]. Arthritis Rheumatol. 2016; 68 (suppl 10). https://acrabstracts.org/abstract/vitamin-d-insufficiency-in-patients-with-rheumatoid-arthritis-and-healthy-controls-and-correlation-between-vitamin-d-levels-and-disease-activity-and-disability-in-ra-patients/. Accessed .« Back to 2016 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/vitamin-d-insufficiency-in-patients-with-rheumatoid-arthritis-and-healthy-controls-and-correlation-between-vitamin-d-levels-and-disease-activity-and-disability-in-ra-patients/