Session Information
Session Type: ACR Concurrent Abstract Session
Session Time: 2:30PM-4:00PM
Background/Purpose :
Epidermal growth factor (EGF) mediates distal tubular epithelial cell function and regeneration. Monocyte chemoattractant protein-1 (MCP-1) participates in recruitment of leukocytes to areas of inflammation. Urinary EGF (uEGF) and MCP-1 (uMCP-1) predict active and chronic renal disease in primary glomerulopathies. This study examined the utility of uEGF and uMCP-1 as biomarkers of renal disease in patients with ANCA-associated vasculitis (AAV).
Methods:
Data from patients with AAV enrolled in a prospective multicenter cohort were included. uEGF and uMCP-1 were measured at baseline, an active renal disease visit (index), 1-2 visits prior to and after the index visit, and at 1 year follow-up. Chronic kidney disease (CKD) was defined as eGFR< 60 mL/min/1.73 m2 for >3 months. Index was defined as the first visit with a new/worse BVAS/WG renal item since prior visit. uEGF and uMCP1 were converted to log2 uEGF/urinary creatinine and log2 uMCP1/urinary creatinine ratios for all analyses. To assess the association of each biomarker with disease activity, a mixed effect model was used, adjusting for ANCA type (MPO or PR-3), albumin/creatinine ratio, eGFR, and visit type. To assess time to CKD outcome, a Cox proportional hazard model was used, adjusting for sex, age, race, ANCA type, albumin/creatinine, and eGFR.
Results:
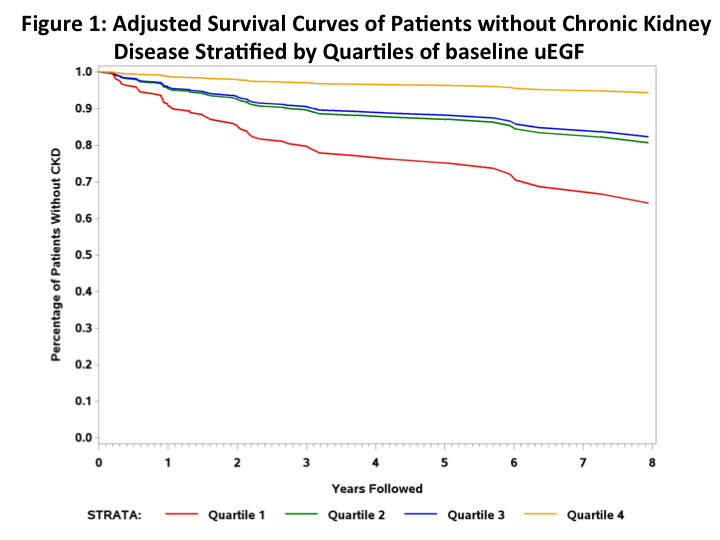
At baseline, 165 of 544 (30%) patients had CKD. For each unit increase in baseline uEGF/Cr there was a lower risk of CKD [HR=0.62, (0.43, 0.88), p=0.01)]. After adjusting for sex, age, race, ANCA type, eGFR, and albumin/Cr, the percentage of patients surviving without CKD was significantly lower (p<0.01) in patients with lower uEGF at baseline (Quartile 1) compared to patients with higher levels of uEGF at baseline (Quartile 4) (Figure 1). Higher baseline uMCP-1/Cr didnÕt predict risk of CKD [HR=1.14, (0.88, 1.48), p=0.33)]. In the same adjusted model, the percentage of patients surviving without CKD was not significantly different (p=0.06) in patients with lower uMCP1 at baseline (Quartile 1) compared to patients with higher levels of uMCP1 (Quartile 4) (Figure 2).
112 patients had active renal disease. uEGF/Cr levels did not significantly differ between pre-, post-, and index visits. Compared to index visit, uMCP-1/Cr was lower at pre- and post-index visits (p=0.04 and p<0.01, respectively) after adjusting for the mixed effect model variables.
Conclusion:
In patients with AAV, uEGF predicts progression to CKD independently of urine albumin/creatinine and eGFR. uMCP-1, but not uEGF, is associated with renal disease activity. uEGF and uMCP-1 are useful biomarkers in AAV.
To cite this abstract in AMA style:
Najem CE, Ju W, Nair V, Cuthbertson D, Rhee RL, Mariani L, Carette S, Khalidi NA, Koening CL, Langford CA, McAlear CA, Monach PA, Moreland LW, Pagnoux C, Seo P, Specks U, Sreih AG, Ytterberg SR, Krischer J, Kretzler M, Merkel PA. Urinary Epidermal Growth Factor and Monocyte Chemoattractant Protein-1 As Biomarkers of Renal Involvement in ANCA-Associated Vasculitis [abstract]. Arthritis Rheumatol. 2017; 69 (suppl 10). https://acrabstracts.org/abstract/urinary-epidermal-growth-factor-and-monocyte-chemoattractant-protein-1-as-biomarkers-of-renal-involvement-in-anca-associated-vasculitis/. Accessed .« Back to 2017 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/urinary-epidermal-growth-factor-and-monocyte-chemoattractant-protein-1-as-biomarkers-of-renal-involvement-in-anca-associated-vasculitis/