Session Information
Date: Sunday, November 8, 2020
Title: SLE – Diagnosis, Manifestations, & Outcomes Poster II: Comorbidities
Session Type: Poster Session C
Session Time: 9:00AM-11:00AM
Background/Purpose: African-Americans have a higher incidence/prevalence of SLE, more lupus nephritis, higher rates of end stage renal disease and higher mortality than Caucasians. The aim of this study was to look at the trajectory of cumulative and individual organ damage accrual in a large longitudinal prospective SLE cohort in which African-American and Caucasian ethnicities were well represented, with a mean follow-up time of 13 years.
Methods: We analyzed data on 2,436 patients (43% African-American, 57% Caucasian, and 92% female) until January 2020. Patients met the revised ACR or SLICC classification criteria. The SLICC/ACR Damage Index (DI) was calculated based on organ damage that occurred after diagnosis until the last visit. Poisson regression allowing for overdispersion for each organ system with an offset term accounting for time followed since diagnosis was used. The outcome variable was the damage score of each organ system at the last available cohort visit. The associations were adjusted for sex, age, income, education, and insurance. We used Cox regression model to determine the association between individual damage items and ethnicity. These associations were adjusted for sex, age, and education.
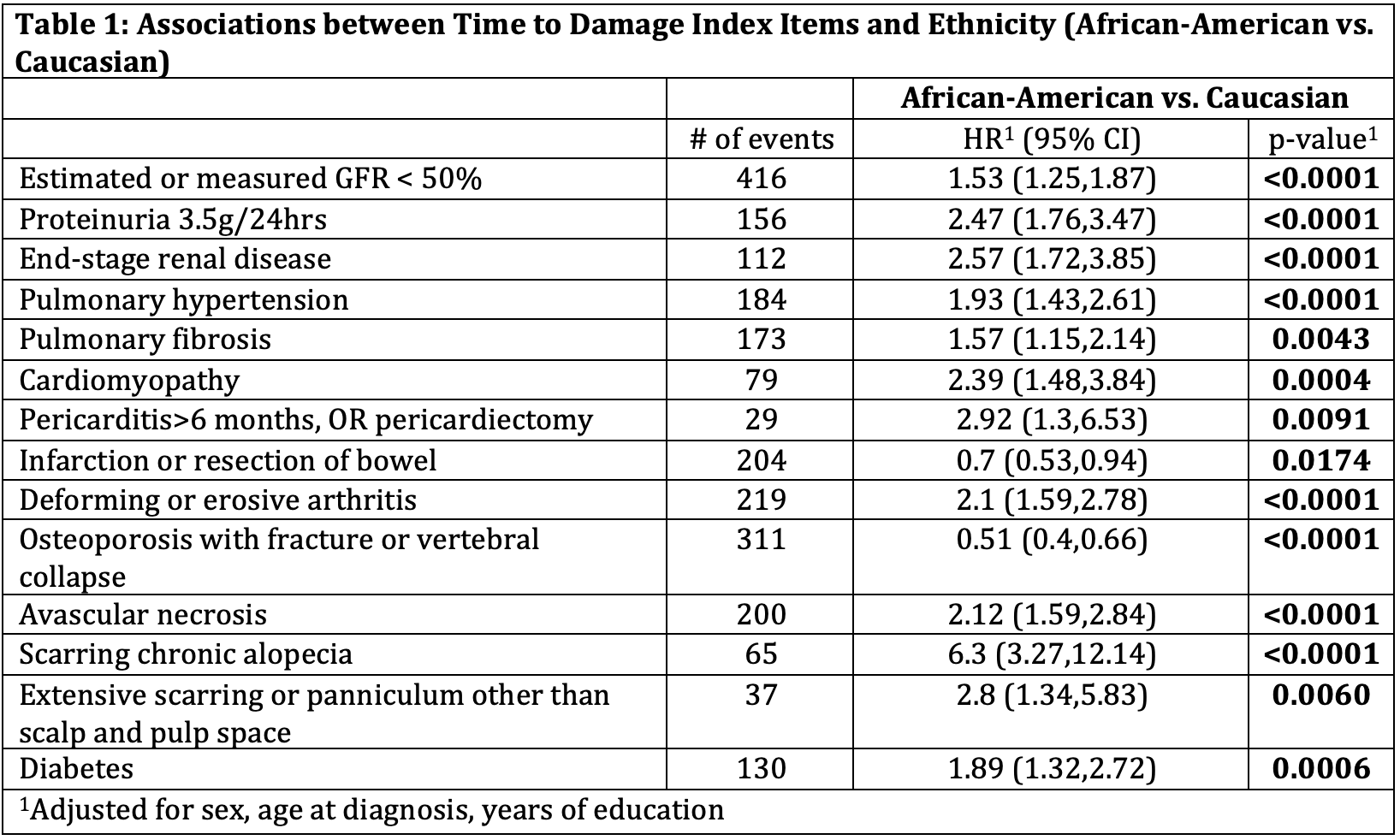
Results: The mean total SLICC/ACR DI was 1.9 (SD=2.3). There was a linear relationship between time since diagnosis and mean DI with no plateau. By 5 years after SLE diagnosis, 44% of African-Americans vs. 36% of Caucasians had accrued damage. The rate of cumulative damage accrual was significantly higher in African-Americans (p-value 0.01). The mean time to onset of damage was 6.6 (SD 7.1) years from SLE diagnosis in Caucasian and 5.5 (SD 6.3) years in African-Americans. The divergence of the curves started early in the disease course. Renal (p-value < 0.0001), pulmonary (p-value 0.0066), and skin (p-value < 0.0001) damage in African-Americans accumulated at a higher rate compared to Caucasians (Figure 1). African-Americans had a higher risk of renal insufficiency, proteinuria 3.5g/24hrs, end-stage renal disease, pulmonary hypertension, pulmonary fibrosis, cardiomyopathy, pericardial damage, deforming or erosive arthritis, avascular necrosis, skin damage, and diabetes than Caucasians at any time during follow-up. On the other hand, Caucasian patients were at higher risk for osteoporosis with fracture or vertebral collapse and infarction or resection of bowel (Table 1).
Conclusion: At any point during the disease, the SLICC/ACR DI was higher and accrued at a faster rate in African-American compared to Caucasian SLE. Damage in most organ systems progressed at a faster rate in African-Americans with the exception of osteopenic fracture and bowel infarction/resection. Of particular concern was the linear increase in damage in both ethnicities over time.
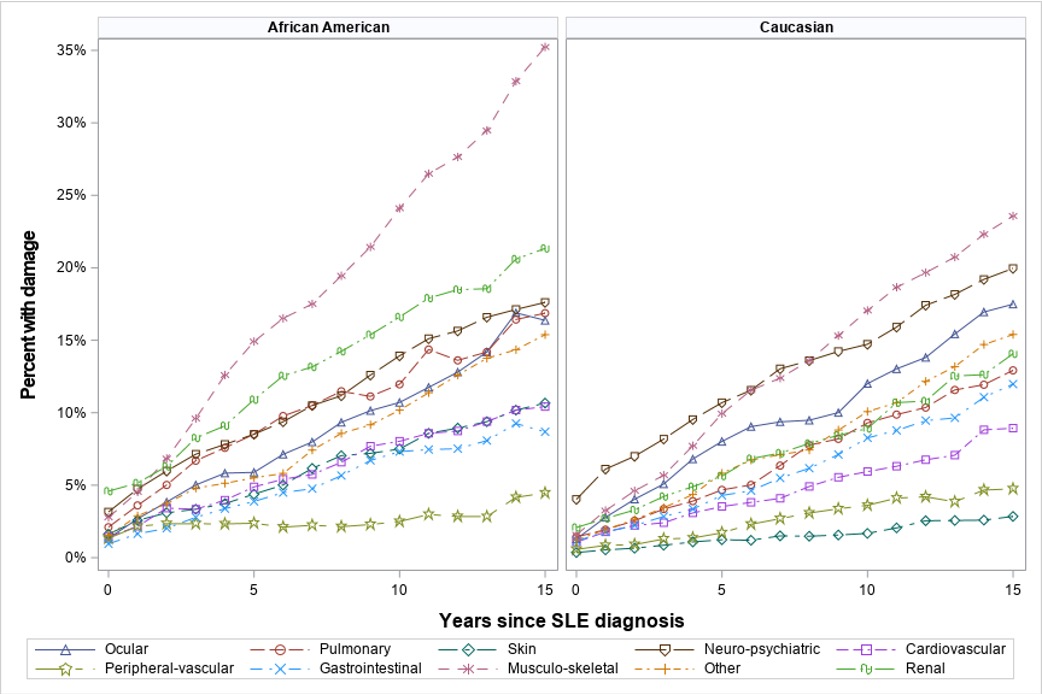 Figure 1: Damage accrual rate of each organ over time in African-American and Caucasian patients
Figure 1: Damage accrual rate of each organ over time in African-American and Caucasian patients
To cite this abstract in AMA style:
Kallas R, Li J, Goldman D, Petri M. Trajectory of Damage Accrual in African-American vs. Caucasian Systemic Lupus Erythematosus [abstract]. Arthritis Rheumatol. 2020; 72 (suppl 10). https://acrabstracts.org/abstract/trajectory-of-damage-accrual-in-african-american-vs-caucasian-systemic-lupus-erythematosus/. Accessed .« Back to ACR Convergence 2020
ACR Meeting Abstracts - https://acrabstracts.org/abstract/trajectory-of-damage-accrual-in-african-american-vs-caucasian-systemic-lupus-erythematosus/