Session Information
Date: Tuesday, November 12, 2019
Title: Epidemiology & Public Health Poster III: OA, Gout, & Other Diseases
Session Type: Poster Session (Tuesday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Pain is the hallmark symptom of many rheumatologic conditions and chronic pain management is a major part of clinical practice in rheumatology. Therefore, as the country and medical community evaluate and respond to the opioid epidemic, rheumatologists should be in the forefront of these discussions and response. In rheumatoid arthritis (RA), chronic opioid use doubled from 2002 to 2015, with peak use in 2010 (Curtis JR et al, Arthritis Rheum, 2017). However, it is still unclear in which diseases in rheumatology opioid use is most prevalent and how rheumatologists have changed their management in response to the crisis. Recent studies suggest an inclination for providers to seek alternate methods of pain control, and focus on the treatment of concomitant psychiatric disease (Yvonne LC et al, Arthritis Rheum, 2018). The purpose of this study was to evaluate changes in opioid and other medication use in the management of chronic pain for common rheumatologic conditions in an outpatient rheumatology clinic of an academic medical center.
Methods: Institutional review board approval was obtained and a retrospective electronic medical chart review was performed. Patients with the primary diagnosis of fibromyalgia (FMS), osteoarthritis (OA), and RA seen in the outpatient rheumatology clinic were randomly selected from 2011 and 2017. Records were reviewed to confirm primary diagnosis, demographic information, and medication use. Specifically, opioid use with consecutive prescriptions for at least 3 month duration, and gabapentin, pregabalin, tramadol, muscle relaxant, and selective serotonin reuptake inhibitor (SSRI) use were evaluated. Chi squared tests were used to analyze differences in medication use prevalence between 2011 and 2017.
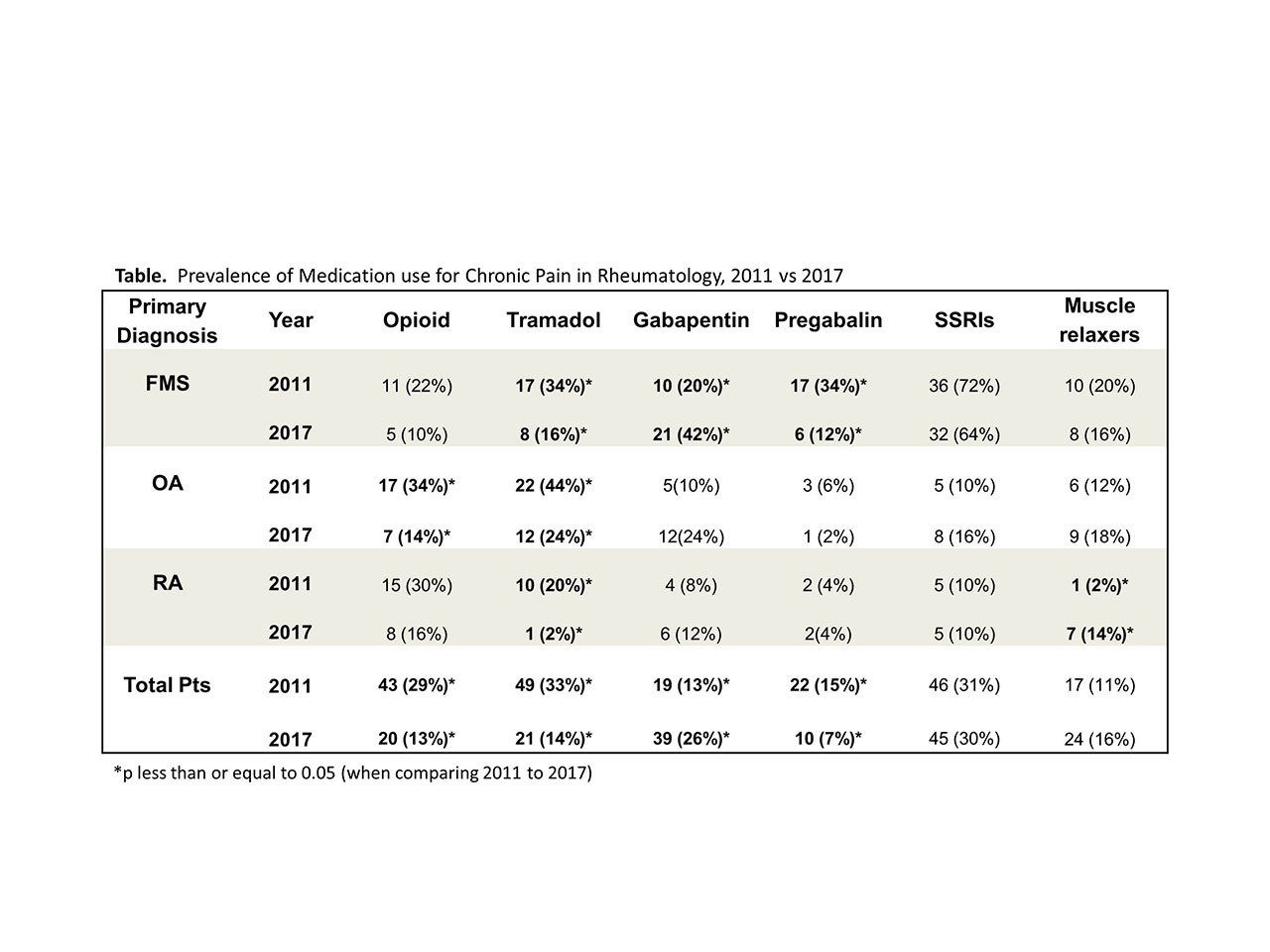
Results: A total of 300 patients were evaluated, 50 in each diagnosis group from 2011 and 2017. Results are summarized in the Table. In 2011, prevalence of opioid use was 34% in OA, 30% in RA, and 22% in FMS. In the groups overall, there was a significant decrease in opioid (p< 0.001), tramadol (p< 0.001) and pregabalin (p=0.022) use from 2011 to 2017. There were also significant increases in gabapentin use (p=0.028). These trends were fairly similar for all groups. Interestingly, no significant changes in prevalence were found for SSRI use any group and muscle relaxant use significantly increased in the RA group only.
Conclusion: The opioid epidemic is a national crisis. In the medical community, rheumatologists are primary contributors to the management of chronic pain and directly affected by this crisis, considering that nearly 30% of these patients were on chronic opioids in 2011. It appears that the clinical community has responded to this epidemic quite dramatically over a 6 year period by decreasing use of opioids, and interestingly tramadol, by nearly 50%, as well as increasing gabapentin use by 50%. Notably, SSRI use did not increase, but remained relatively high at 30%. Rheumatologists should be major contributors to the discussions regarding management of chronic pain and we should continue to evaluate optimal chronic pain management regimens that provide improved quality of life for our patients without substantial risk.
To cite this abstract in AMA style:
Grant M, Kwiatkowski A, Shakoor N. The Opioid Epidemic: The Rheumatology Response to Management of Chronic Pain [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/the-opioid-epidemic-the-rheumatology-response-to-management-of-chronic-pain/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-opioid-epidemic-the-rheumatology-response-to-management-of-chronic-pain/