Session Information
Title: Rheumatoid Arthritis - Clinical Aspects (ACR): Comorbidities, Treatment Outcomes and Mortality
Session Type: Abstract Submissions (ACR)
Background/Purpose: Fatigue is common and burdensome in Rheumatoid Arthritis (RA). Though RA fatigue progression varies significantly between individuals, to date, published analyses have only considered average changes in fatigue. The aim of the current study was to determine if it is possible to distinguish participants who follow distinct trajectories of fatigue reporting over time and thus potentially inform to whom specific management should be targeted.
Methods: Participants from the Norfolk Arthritis Register (NOAR), a long-term inflammatory polyarthritis (IP) inception cohort, who met 1987 ACR RA criteria reported levels of fatigue (0-100mm visual analogue scale (VAS)) at recruitment and annually thereafter for four years. Among those with clinically relevant fatigue at recruitment (VAS≥20mm), changes in fatigue were calculated over the four years of follow-up; clinically significant improvements were defined as ≥10mm. Latent fatigue trajectory groups were determined using sex-stratified group-based trajectory modelling. Baseline variables (demographic, clinical and patient-reported) were compared between identified groups using descriptive statistics (p<0.05 considered significant).
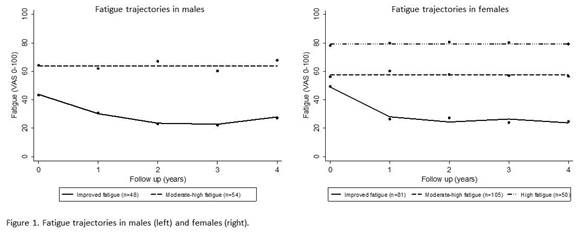
Results: In 338 participants (30.2% male), there were only small average improvements in fatigue from recruitment to one (6.0mm, SD 26.9) and four years later (5.5mm, 29.3), yet improvements were clinically significant for 45.2% and 56.0% of participants at these follow-ups, respectively. The best fitting models revealed two fatigue trajectories in men (improved, and moderate-high), and three trajectories in women (as the male group, plus an additional ‘High’ trajectory (Figure 1)).
To determine the characteristics of those likely to benefit from fatigue-specific interventions, baseline variables were compared between those who improved and all other participants (‘non-improved’). In both sexes, non-improvers reported significantly poorer scores for disability, pain, fatigue and sleep problems, at baseline. Female non-improvers were significantly younger, reported more disease activity and use of antidepressants and NSAIDs. Whereas, in males, the use of analgesics at recruitment was greater among non-improvers; as was the proportion of patients unable to work due to illness.
Conclusion: Among a group of patients who, on average, show only small improvements in fatigue, significant variation in fatigue progression exists. At presentation, it is possible to identify and characterise sub-groups of patients who do not improve. Such patients are most likely to require early and targeted interventions, to alleviate fatigue.
Disclosure:
K. L. Druce,
None;
G. T. Jones,
None;
G. J. Macfarlane,
None;
S. M. Verstappen,
None;
N. Basu,
None.
« Back to 2014 ACR/ARHP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/the-longitudinal-course-of-fatigue-in-rheumatoid-arthritis-results-from-the-norfolk-arthritis-register/