Session Information
Session Type: Poster Session (Monday)
Session Time: 9:00AM-11:00AM
Background/Purpose: Idiopathic inflammatory myopathies (IIM) are chronic autoimmune diseases with systemic features and multiple comorbidities. Of the myositis associated antibodies seen in this population, anti-SSA/SSB are most frequently reported. However, limited literature has been published on their utility in clinical risk assessment.
Aim: To describe the spectrum of organ involvement and frequency of comorbidities in IIM patients and relation to anti-SSA/SSB positivity.
Methods: We queried the Northwell Myositis Center database for patients with IIM between 1/1/2007 to 4/6/2018. Patients were selected if they met 2017 European League Against Rheumatism (EULAR)/American College of Rheumatology (ACR) classification criteria for IIM and had anti-SSA/SSB data available. Anti-SSA/SSB was measured using a commercially available fluorescent bead-based immunoassay. Anti-SSA and SSB were combined and analyzed as a single group because anti-SSB was only found in association with anti-SSA in this cohort. The frequency of myositis specific antibodies, organ involvement and comorbidities was collected. Statistical analyses included Chi-square, Fisher’s Exact test, and Wilcoxon Rank Sum test to determine statistical differences in group distributions and McNemar’s test was performed to compare groups.
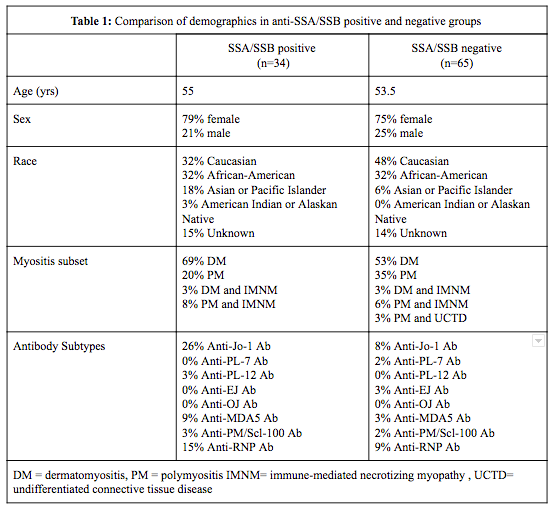
Results: Ninety-nine (99) patients were included in this analysis. The SSA/SSB positive (n=34) and negative (n=65) groups had similar distributions for age, gender, and race (Table 1). Despite the presence of muscle weakness during their clinical course, the majority (82/99) did not show evidence of muscle atrophy on magnetic resonance imaging (MRI). There was no difference in the prevalence of calcinosis, cardiac, or gastrointestinal involvement between groups. As anticipated, the frequency of ILD was significantly higher in the anti-SSA/SSB positive cohort (56% of SSA/SSB positive in comparison to 25% of SSA/SSB negative, p-value= 0.0084). The overall frequency of diabetes in our cohort was 42%, four times higher than reported for general population. The frequency of hypertension in our cohort was also as high (40%). There was no significant difference in the rate of diabetes, hypertension, or cardiovascular events between SSA/SSB positive and negative groups. There was 4% (4/99) myocardial infarctions and no cerebrovascular accidents. Venous thromboembolic events (VTE) were observed in 10% of patients with the majority (83%) occurring within three years of diagnosis. Presence of anti-SSA/SSB did not confer additional risk for VTE. Finally, SSA/SSB positivity was not associated with malignancies in our cohort. Neoplasms occurred in 14 anti-SSA/SSB negative patients (compared with 2 anti-SSA/SSB positive), though more than 18 years prior IIM diagnosis and not likely associated with the autoimmune disease.
Conclusion: Patients with IIM had high frequencies of diabetes, hypertension and VTE which was independent of anti-SSA/SSB status. We observed a statistically significant increase in prevalence of ILD in the anti-SSA/SSB positive IIM cohort patients suggesting that the presence anti-SSA/SSB antibodies is a harbinger of pulmonary manifestations in IIM.
To cite this abstract in AMA style:
Valle A, Marder G, Barilla-Labarca M, Narain S. Spectrum of Organ Involvement in Idiopathic Inflammatory Myopathies, Frequency of Comorbidities, and Relationship to Anti-SSA/SSB Positivity [abstract]. Arthritis Rheumatol. 2019; 71 (suppl 10). https://acrabstracts.org/abstract/spectrum-of-organ-involvement-in-idiopathic-inflammatory-myopathies-frequency-of-comorbidities-and-relationship-to-anti-ssa-ssb-positivity/. Accessed .« Back to 2019 ACR/ARP Annual Meeting
ACR Meeting Abstracts - https://acrabstracts.org/abstract/spectrum-of-organ-involvement-in-idiopathic-inflammatory-myopathies-frequency-of-comorbidities-and-relationship-to-anti-ssa-ssb-positivity/